Tea Tree Oil Treatment of MRSA
The prevalence of Methicillin-resistant Staphyloccocus aureus (MRSA) as a pathogen in hospitals and other community settings underscores the importance of eradicating the infection.1 As MRSA is not susceptible to commonly used antibiotics, alternative antimicrobial agents are being sought for its eradication. One area of interest involves the use of tea tree oil, which studies have shown to effectively treat infections of drug-resistant bacteria, including MRSA.2
Introduction
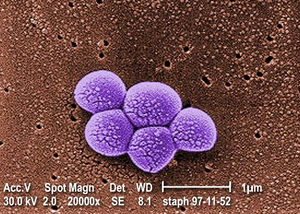
Staphyloccocus aureus, more commonly known as staph bacteria or MRSA, is a Gram-positive coccus-shaped anaerobic bacterium pictured in Figure 1.1 MRSA is a type of staph bacteria that is resistant to beta-lactam antibiotics, such as penicillin, amoxicillin, oxacillin, and methicillin. MRSA is also becoming resistant to mupirocin, the current standard antibiotic used in the treatment of MRSA infection.3. MRSA often colonizes on the skin or nostrils of healthy individuals, and is relatively harmless at these sites.1 If S. aureus enters the body (e.g., wounds, cuts), it may cause infections. In such instances, the MRSA infection may range from mild (e.g., pimples) to life-threatening (e.g., infection of bloodstream, joints, or bones).1 MRSA is spread through contact and most commonly contracted in public settings, namely hospitals.
Tea tree oil (TTO) is the essential oil derived through steam distillation from the Australian native plant Melaleuca alternifolia. Tea tree oil has been used for centuries as a topical antiseptic. TTO is believed to have antibacterial, antifungal, antiviral, and anti-inflammatory properties when used topically.4 TTO may be found as additives in beauty and health products, including shampoo, soap, and nasal spray. Although historical anecdotes endorse TTO's medicinal properties, few clinical studies have been conducted to support such claims. Clinical studies, however few, indicate that tea tree oil can treat the skin infection caused by MRSA.4 Tea tree oil's anti-microbial properties are attributed to belonging to a class of chemicals known as terpenes, specifically terpinen-4-ol.4 Tea tree oil's bactericidal effects make this plant extract a plausible addition or supplement to a MRSA treatment plan.
Tea Tree Oil Composition and Chemistry
Commercially available TTO is a composition of nearly 100 chemical compounds determined by gas chromatography-mass spectrometry.5 TTO is primarily composed of a class of chemicals called monoterpenes. Typically, monoterpenes are volatile, aromatic hydrocarbons that are lipophilic, meaning that they can dissolve in fats or lipids.4
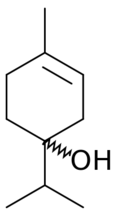
Terpinen-4-ol, pictured in Figure 2, is the specific monoterpenic compound believed primarily responsible for TTO's anti-microbial activity. This hydrocarbon compound has one alcohol group attached to the fourth carbon. Like all monoterpenes, terpinen-4-ol’s mostly hydrocarbon structure gives the molecule lipophilic properties.4 Researchers claim that the lipophilic nature of monoterpenes contributes to its antimicrobial activity, though the exact details of the antimicrobial mechanism are not currently known.4 Other monoterpenic compounds in TTO include 1,8-cineole, terpinolene, and α-terpineol, whose medicinal properties are also under investigation.4
TTO composition is commercially available in various chemotypes. The most common chemotype is the terpinen-4-ol chemotype where terpinen-4-ol comprises between 30 to 40% of commercially available TTO.4 A relatively high composition of terpinen-4-ol is more common in commercial production due to its demonstrated broad spectrum of biological activities. 4,5
Antimicrobial Activity: Cytoplasmic Membrane Damage

The target of TTO's antimicrobial activity, and the primary reason for its laboratory and clinical effectiveness, is reported to be the cytoplasmic membrane of MRSA. The bacterial cell membrane physically separates the cell's internal environment from the external environment. It is selectively permeable to organic molecules and ions. As such, it regulates the movement of water and other substances into and out of the cell.6 If the membrane permeability were compromised, then the barrier between the internal and external environment would be weakened. Consequently, foreign material could enter the cell more easily while cytoplasmic material could leave it more easily (as shown in Figure 3).7,2
Based on the lipophilicity of the terpinen-4-ol molecule and other TTO components, researchers have proposed that TTO can insert itself into and damage the lipid-rich biological membranes.4 Studies examining membrane integrity after TTO treatment indicate that the essential oil disrupts the vital function of the biological membrane 7,2
An in vitro (i.e. laboratory) study by Cox et al. found that TTO treatment disturbed the MRSA membrane permeability, which allowed propidium iodide, a foreign substance, to enter the cell and potassium ions, part of the cytoplasmic material, to leave the cell.7 Another in vitro study demonstrated that TTO-treated MRSA had increased susceptibility to sodium chloride (NaCl), a cell toxin.2 From this evidence, researchers believed that TTO altered the cell membrane.
The loss of intracellular material and the inability to maintain osmotic regulation is consistent with a mechanism of action involving the loss of membrane integrity. Despite evidence of cytoplasmic membrane damage, the molecular mechanism of this impairment is still unknown and warrants further research.4
Treatment and Effectiveness
Efforts to validate the therapeutic properties of tea tree oil (TTO) have yielded in vitro and clinical studies showing that TTO treatment eradicates and reduces MRSA infection, respectively. While TTO displays in vitro and clinical efficiency, TTO has not been demonstrated to prevent initial MRSA colonization. Several studies described below and illustrated by Figure 4, support the claims upheld by traditional healers that TTO is an effective antimicrobial agent.
In vitro Effectiveness
The efficacy of tea tree oil (TTO) against MRSA has been demonstrated in laboratory studies using cultured S. aureus samples. An in vitro study by May et al. showed that 99.9% of the MRSA isolate was killed by TTO within 4 hours and that all was eradicated after 6 hours of continuous exposure to 5% TTO.8 These results suggest that TTO's antimicrobial properties make this a good agent to control MRSA and reduce its transmission among humans.
Clinical Efficiency

The efficiency of TTO in eradicating MRSA cultures in vitro led to clinical testing with human patients using products enhanced with TTO. TTO may be added to commercial products, such as body wash, skin cream, and nasal ointment due to its antimicrobial properties. The clinical efficacy of TTO body wash and creams as a decolonization agent for MRSA has been supported by Caelli et al. and Dryden et al..9, 3 Both researchers found that TTO treatment is as effective as the standard treatment regimen, indicating that TTO treatment may enhance a MRSA eradication regimen.
Caelli et al. clinically determined that TTO treatment was as effective as the standard MRSA medical treatment.9 Caelli compared the effectiveness of TTO treatment to that of standard treatments against MRSA, as measured by post-treatment MRSA concentrations on the skin and within the nose of human patients.9 Compared to the standard treatment, the tea tree oil topical regimen reduced or eradicated MRSA infection in more subjects. Despite this optimistic finding, the small sample size prevented this result from being statistically significant. Consequently, Caelli concluded that TTO treatment had a similar effect as standard medical treatment at eradicating MRSA 5
In a similar study, Dryden et al. found that TTO cleared up MRSA-related skin infections better than the standard medical treatment.3 Dryden's clinical study found that the daily application of 5% TTO body wash and 10% TTO cream was more effective than standard treatment at clearing skin lesions associated with MRSA infection.3 Although research suggests the efficacy of TTO against MRSA, more clinical studies would have to be performed in order to comprehensively assess TTO's effects on MRSA patients. From these experiments, TTO was deemed to be sufficiently effective, safe, and well-tolerated to be considered part of a MRSA eradication regimen.3
Dermal Toxicity
Despite characterizing TTO’s antimicrobial properties, researchers have not done much work on the safety and toxicity of using TTO topically. The rationale for continued topical use of TTO primarily rests on anecdotal evidence of its safe usage at low concentrations.4 No human deaths due to TTO exposure have been reported.4 Though there are few substantial scientific studies regarding TTO’s safety, TTO can cause irritant or allergic reactions when applied to the skin.4 More concrete evidence of TTO’s toxicity would be necessary in order to determine its optimal concentration for safe usage.
Susceptibility to Antibiotic Resistance after TTO Exposure
The available forms of TTO range from pure oil to retail products for personal health care, home care, and pet care.10 Commercial TTO preparations, which may vary in its components' concentrations, provide users more opportunity to apply TTO at ineffective concentrations. The growing use of TTO also implies that a diversity of microbes is coming into contact with sub-lethal TTO concentrations.10 There is concern that exposing MRSA to sub-lethal concentrations of TTO may lead to decreased antibiotic susceptibility (i.e. increased antibiotic resistance). 11
TTO-Induced Antibiotic Resistance is Unlikely

Whether TTO exposure decreases antibiotic susceptibility in MRSA remains a subject of investigation. Evidence has been presented for both sides of this debate by McMahon et al and Thomsen et al.12,13 Both researchers used similar experimental design: they examined the changes in minimal inhibitory concentrations (MIC) of various antibiotics before and after MRSA was inoculated with tea tree oil for 72 hours. 12,13 McMahon’s key study reported that habituating MRSA isolates to a sub-lethal concentration of TTO increased MRSA’s resistance to antibiotics.12 During an attempt to replicate McMahon’s findings, Thomsen instead found that habituating MRSA isolates to a sub-lethal concentration of TTO did not increase MRSA’s antibiotic resistance.13 Although McMahon’s findings couldn’t be confirmed, their key study prompted a number of further studies regarding the possibility of MRSA-induced antibiotic resistance.
Further investigation reports that it is unlikely that TTO induces antibiotic resistance. A study by Hammer et al. seconded Thomsen’s idea that exposure to sub-lethal levels of tea tree oil was not linked to development of antibiotic resistance.14 Hammer also claimed that since monoterpenes target the “structure, function, and integrity of microbial membranes, it seems unlikely that true resistance will arise” from TTO usage.14
Implications of TTO-Induced Antibiotic Resistance
Given the unexplored clinical significance regarding TTO-induced antibiotic resistance, the discussion of TTO-induced antibiotic resistance remains relevant.12 If found to impact antibiotic susceptibility, TTO concentrations in retail products may be increased so that there is less exposure to sub-lethal TTO concentrations.12 This may be achieved through legislation or regulation of TTO formulation.
Conclusion
Discovering alternative therapy for the treatment of MRSA is very important as antibiotic resistance becomes more prevalent. MRSA's increasing resistance to mupirocin, the primary antibiotic in standard MRSA eradication treatments, has been noted by Dryden.3 Since TTO shows little sign of inducing antibiotic susceptibility in MRSA upon treatment, one alternative treatment is the use of tea tree oil as an antimicrobial agent.13
The application of a TTO regimen is comparable to standard MRSA treatment in eradicating MRSA.9,3 The reported mechanism for TTO's bactericidal effects is damage to the cytoplasmic membrane, thus making the membrane more permeable to substances, such as water.2 Impaired osmoregulation may lead to cell lysis.2
Current research focuses on TTO's mechanism of action, safety, and effect on antibiotic susceptibility. Though cytoplasmic membrane damage is believed to be the major bactericidal effect, the mechanism is still largely unexplored. Other research examines commercial tea tree oil's cytotoxic effects if applied topically to human skin.15 Such investigations would determine the safety of applying TTO on a regular basis and hopefully, the optimal strength of TTO for pharmaceutical formulation.
References
10."Tea tree oil" American Cancer Society Web site. 28/11/2008 Revised. 16/04/2013 Accessed.
[Edited by Karen Leung, a student of Nora Sullivan in BIOL187S (Microbial Life) in The Keck Science Department of the Claremont Colleges Spring 2013.

