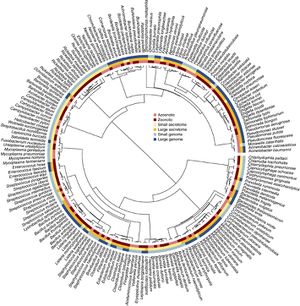
Pathology of Mycoplasma fermentans
Classification
a. Higher order taxa
Bacteria (Domain), Terrabacteria group (Kingdom), Tenericutes (Phylum), Mollicutes (Class), Mycoplasmatales (Order), Mycoplasmataceae (Family), Mycoplasma (Genus), fermentans (Species) (1)
b. Species
Mycoplasma fermentans
Description and significance
a. Description
Mycoplasma fermentans is a Gram-negative (2) non-motile (3), and cell wall-less bacterium (4) found in humans (2).
M. fermentans is a co-infector in immunocompromised individuals and acts as an opportunistic pathogen; that is, M.fermentans will only infect host cells in a person whose immune system is already weakened by another preexisting infection.
By using and/or sequencing the genomes of M64 (2), JER (4), and PG18 (5) strains of M. fermentans, and identifying common environments in which M. fermentans have been found, researchers have been able to identify the genome structure, cell structure, metabolic processes, and ecology of these strains of the bacterium. The strains of this bacterium are highly heterogenous, and thus, the information provided about M64, JER, and PG18 can not necessarily extend to all strains of M. fermentans (6). These particular strains are three that have been sequenced in current research. M64 and JER strains were isolated from non-immunocompromised individuals, whereas PG18 was isolated from an immunocompromised patient with arthritis (2-5). M64 and JER strains contained large amounts of genomic content that allow them to become pathogenetic (2, 4), yet these strains would not have been pathogenetic in the samples from which they were isolated, because they were from individuals with normal immune function.
b.Significance to human society
M. fermentans carries pathogenic characteristics which negatively affect humans, specifically immunocompromised individuals, and has been shown to become resistant to certain antibiotics (3, 4, 7-9). M. fermentans has the ability to act as a co-infector in immunodeficiency disorders, such as in HIV/AIDS, Amyotrophic Lateral Sclerosis, and rheumatoid arthritis (5; 10-12). M. fermentans is capable of becoming resistant to specific types of antibiotics, such as macrolides and fluoroquinolones (8). M.fermentans infects host cells by adhering to cell membrane surface components, leading to internalization (3). Furthermore, the ability of M. fermentans to adhere to host cells increases in immunocompromised human cells, leading to cell death (3).
Key pathogenic characteristics
a. Genome structure
The M64 strain of M. fermentans contains a high density of transposable elements (2). These elements play a large role in recombination and mutation. The genome of the JER strain of M. fermentans consists of proteins involved in replication and recombination (4). Thus, the genome structure of different strains of M. fermentans allows these strains of bacteria to replicate, mutate, and participate in homologous recombination, which are all ways that M. fermentans can develop antibiotic resistance.
b. Cellular structure
Antibiotics that target cell wall synthesis in order to kill pathogenic bacteria, such as penicillin, are ineffective against M. fermentans due to the lack of a cell wall (2, 4). Additionally, the lack of a cell wall minimizes the distance in between the bacterium and host cells, allowing M. fermentans to invade cells quickly through direct contact (13). The JER strain of M. fermentans contains a high density of ABC transporters, lipoproteins, and nucleases and proteases (4). Pathogenic bacteria use ABC transporters to intake nutrients from the host cells they attack (4). Lipoproteins defend mycoplasmas against the immune response of host cells (4). Nucleases and proteases break down host cell DNA and proteins (4). Thus, these cellular components allow M. fermentans to engage in pathogenic activity (4).
c. Metabolic structure
Components of M. fermentans are necessary for glycolysis pathway and arginine deiminase (ADI) pathway (4), meaning that M. fermentans can use glucose and arginine for metabolism. Both glucose and arginine are found in human cells (14).
d. Ecology
M. fermentans grows well at 37 degrees Celsius (2). This means that M. fermentans can incubate and grow well in the human body. Specifically, M. fermentans is most commonly found that in the genitourinary and respiratory tracts of humans (2).
Mode of infection
Mycoplasma fermentans is a non-motile bacterium that can adhere to, internalize into, and thus infect host cells using a surface protein and a protease (3). As discussed previously, M. fermentans is also more likely to infect immunocompromised host cells than cells with normal immune function because it is an opportunistic bacterium, as discussed previously. Yavlovich et al studied how M. fermentans specifically binds and invades to HeLa cells (3), a cell line of immunocompromised cervical cancer cells conserved from the 1950s for research purposes (15). Host cells can contain surface proteins called plasminogen, and M. fermentans contains receptor sites to which plasminogen binds (3). The binding of M. fermentans to these host cells enhances the conversion of plasminogen to plasmin by the urokinase-type plasminogen activator (uPA) (3). M. fermentans bound to plasminogen in the presence of uPA was able to invade HeLa cells, while M. fermentans without uPA was not (3). Thus, the adherence and invasion of M. fermentans to HeLa cells is dependent upon the plasminogen binding in the presence of uPA (3).
Additional factors that increase the internalization of M. fermentans into host cells are lipid raft networks containing cholesterol in host cell membranes, and the presence of divalent cations such as Mg2+ and Ca2+ in the environment, while factors that decreases the ability of M. fermentans to invade host cells are environmental temperatures lower than 37°C (the human body temperature) and environments of high osmolarity (3).
Prevalence of co-infection
One of the main roles of Mycoplasma bacteria is to exist as opportunistic co-infectors in a wide range of autoimmune and nervous system diseases. M. fermentans, specifically, has been widely documented as a co-infector in Human Immunodeficiency Virus (HIV)-positive patients (10). For example, M. fermentans has been found present in HIV-positive patients with a degenerative renal condition, but not inAIDS-infected patients with normal renal function (10). M. fermentans may be directly responsible for the pathogenesis of HIV-related disorders, such as this renal condition, HIV-associated nephropathy (HIVAN), or the bacteria may colonize tissues of patients with such conditions common in immunocompromised individuals (10).
Mycoplasmas have been linked to multiple autoimmune disorders, including rheumatoid arthritis. M. fermentans is present in high percentages in the blood of patients with rheumatoid arthritis, but is not present in healthy individuals (5). In addition to the presence of M. fermentans in the blood of these patients, the antibodies IgM and IgG for the M. fermentans strain PG18 were found more frequently in patients with rheumatoid arthritis than in healthy patients (5), showing that more M. fermentans is present in patients with rheumatoid arthritis.
There is a link between mycoplasmal infections and Gulf War Illness, a specific subset of Amyotrophic Lateral Sclerosis (ALS) patients who served in the Gulf War (12). Patients with Gulf War Illness experienced systemic M. fermentans infections, and these infectious can significantly contribute to the morbidity of ALS (12). While a variety of mycoplasmas were found in patients with ALS in one particular study, M. fermentans was the only strain present in all patients, proving to be the dominant mycoplasma in ALS infections (12). Furthermore, M. fermentans may be associated with the effects of ALS because this bacterium is able to penetrate the central nervous system (CNS) and cause neurological deficits in addition to being involved in coinfections (12).
M. fermentans is also implicated in Chronic Fatigue Syndrome (CFS). While the direct cause of CFS remains elusive, the prevalence of M. fermentans was found to be dramatically higher in CFS-positive blood samples than in CFS-negative samples in one study (16). Additionally, M. fermentans in rats can trigger the production of nitric oxide, a chemical which is found to contribute to oxidative stress, which is a symptom that CFS patients experience (17). The presence of M. fermentans in rat host cells increases the production of signaling molecules that cause inflammation, demyelination, and neural damage in neurodegenerative diseases like CFS (18).
Antibiotic resistance
M. fermentans has been shown to be resistant to antibiotics that target cell wall synthesis, in addition to some antibiotics that target protein synthesis. In one journal article, all strains studied of M. fermentans showed the most resistance to erythromycin and clarithromycin out of the macrolide antibiotics; ampicillin out of the penicillins; and streptomycin out of the aminoglycosides (7). Another study revealed that M. fermentans exhibited resistance against macrolides, lincosamides, streptogramins, and ketolides, nicknamed MLSK because these antibiotics are all structurally related (8). Furthermore, aminoglycosides, beta-lactam antibiotics (including penicillins), and fosfomycin, which attack cell wall synthesis, do not affect M. fermentans at all because of the lack of cell wall (9).
M. fermentans is capable of becoming resistant to antibiotics that were once effective in killing M. fermentans cells because of its ability to mutate using its genomic content. Tetracyclines and macrolides, which inhibit protein synthesis, and fluoroquinolones, which inhibit DNA synthesis and are commonly used to treat urinary and respiratory diseases, are the most effective antibiotics used against all mycoplasmas (9, 19). However, once a patient with M. fermentans uses these antibiotics, M. fermentans can develop resistance to them by causing conformational changes to ribosomal subunits and mutations in genes that code for enzymes involved in transcription and translation (9). This is problematic, especially for immunocompromised individuals, because clinicians tend to prescribe macrolides to control infections caused or exacerbated by M. fermentans for these patients (9). Furthermore, the ability of M. fermentans strains to exhibit resistance to all antibiotics increases in immunocompromised individuals (7).
Current research
Current research on M. fermentans studies the use of chemicals and drugs besides antibiotics to treat infections caused by M. fermentans, so as to avoid the concern for antibiotic resistance. For example, one study from 2014 showed that hydrogen sulfide (H2S) weakens the inflammatory response of cells infected with M. fermentans (20). The H2S “gasotransmitter” does this by targeting the NF-KB pathway during transcription (20) . This study gives an example of how to combat M. fermentans infections without the use of antibiotics, which is advantageous because of the ability of M. fermentans to develop resistance against some antibiotics.
Another area of current research shows the link of M.fermentans to the effectiveness of anti-cancer drugs. Anti-cancer drugs, also known as camptothecins (CPTs), work to decrease Topoisomerase I activity in cancerous cells because it is involved in DNA replication and transcription by preventing DNA supercoiling (21). However, the presence of M.fermentans in cancerous tumors inhibited Topoisomerase I activity before being treated with CPTs, diminishing the effects of the anti-cancer drugs, which presents a danger to cancer patients (21). In the last decade, lipoproteins in M.fermentans have also been shown to cause cells to express oncogenes and inhibit apoptosis in tumors (21). While it is unclear whether these results will happen in vivo in patients, as this test was done to understand the effects of mycoplasma infections on tumors and anti-cancer drugs, it paves the way for future research regarding cancer treatment and mycoplasma infections (21).
References
1: National Center for Biotechnology Information. n.d.. Taxonomy Browser: Mycoplasma fermentans JER [Database]. Retrieved from https://www.ncbi.nlm.nih.gov/Taxonomy/Browser/wwwtax.cgi?mode=Info&id=637387&lvl=3&p=mapview&p=has_linkout&p=blast_url&p=genome_blast&lin=f&keep=1&srchmode=1&unlock
2: Shu et al. 2011. Genome sequence of the repetitive-sequence-rich Mycoplasma fermentans strain M64. Journal of Bacteriology, 193 (16): 4302-4303.
3: Yavlovich, A., A. Katzenell, M. Tarshis, A. A.-R. Higazi, and S. Rottem. 2004. Mycoplasma fermentans binds to and invades HeLa cells: Involvement of plasminogen and urokinase. Infection and Immunity, 72(9), 5004–5011.
4: Rechnitzer et al. 2011. Genomic features and insights into the biology of Mycoplasma fermentans. Microbiology Society, 157: 760-773.
5: Gil, C., A. Rivera, D. Bañuelos, S. Salinas, E. Garcia-Latorre, and L. Cedillo. 2009. Presence of Mycoplasma fermentans in the bloodstream of Mexican patients with rheumatoid arthritis and IgM and IgG antibodies against whole microorganism. BMC Musculoskeletal Disorders 10(97).
6: Pitcher, D. and J. Hilbocus. 1998. Variability in the distribution and composition of insertion sequence-like elements in strains of Mycoplasma fermentans. FEMS Microbiology Letters. 160(1):101-109.
7: Hannon, P.C.T. 1995. Antibiotic susceptibility of Mycoplasma fermentans strains from various sources and the development of resistance to aminoglycosides in vitro. Journal of Medical Microbiology, 42 (6): 421-428.
8: Pereyre et al. 2002. Mutations in 23S rRNA account for intrinsic resistance to macrolides in Mycoplasma hominis and Mycoplasma fermentans and for acquired resistance to macrolides in M. hominis. Antimicrobial Agents and Chemotherapy 26 (10): 3142-3150.
9: Chernova, O.A., E.S. Medvedeva, A.A. Mouzykantov, N.B. Baranova, and V.M. Chernov. 2016. Mycoplasmas and their antibiotic resistance: The problems and prospects in controlling infections. Acta Naturae. 8(2): 24-34.
10: Bauer, F., D. Wear, P. Angritt, and S. Lo. 1991. Mycoplasma fermentans (incognitus strain) infection in the kidneys of patients with acquired immunodeficiency syndrome and associated nephropathy: a light microscopic, immunohistochemical, and ultrastructural study. Human Pathology 22(1): 63-69.
11: Kawahito, Y., S. Ichinose, H. Sano, Y. Tsubouchi, M. Kohno, T. Yoshikawa, and K.M. Teruaki Nakano. 2008. Mycoplasma fermentans glycolipid-antigen as a pathogen of rheumatoid arthritis. Biochemical and Biophysical Research Communications, 369: 561–566.
12: Nicolson, G. L., M. Y. Nasralla, J. Haier, and J. Pomfret. 2002. High frequency of systemic mycoplasmal infections in Gulf War veterans and civilians with Amyotrophic Lateral Sclerosis (ALS). Journal of Clinical Neuroscience 9(5): 525-529
13: Rottem, S. 2003. Interaction of Mycoplasmas with host cells. Physiological Reviews. 83(2): 417 LP-432.
14: Morris, S. M. 2006. Arginine: Beyond protein. The American Journal of Clinical Nutrition. 83(2): 508S–512S.
15: Biography. n.d. [Reviewed: 10/17/17]. Henrietta Lacks. https://www.biography.com/people/henrietta-lacks-21366671 [Webpage]. (Accessed Oct 23, 2017).
16: Vojdani, A., P.C. Choppa, C. Tagle, R. Andrin, B. Samimi, and C.W. Lapp. 1998. Detection of Mycoplasma genus and Mycoplasma fermentans by PCR in patients with Chronic Fatigue Syndrome. FEMS Immunology and Medical Microbiology, 22(4), 355–365.
17: Montoya, J. G., T.H. Holmes, J.N. Anderson, H.T. Maecker, Y. Rosenberg-Hasson, I.J. Valencia, and M.M. Davis. 2017. Cytokine signature associated with disease severity in chronic fatigue syndrome patients. Proceedings of the National Academy of Sciences, 114(34), E7150–E7158.
18: Brenner, T., A. Yamin, and R. Galilly. 1994. Mycoplasma triggering of nitric oxide production by central nervous system glial cells and its inhibition by glucocorticoids. Brain Research 641(1): 51-56.
19: Online Textbook of Bacteriology. N.d. (Reviewed: 2012]. Antimicrobial Agents in the Treatment of Infectious Disease. http://textbookofbacteriology.net/antimicrobial_2.html [Webpage]. (Accessed Oct 23, 2017).
20: Benedetti et al. 2014. Sulfur compounds block MCP-1 production by Mycoplasma fermentans-infected macrophages through NF-KB inhibition. Journal of Translational Medicine. 24(12): 145.
21: Afriat, R., S. Horowtiz, and E. Priel. 2013. Mycoplasma fermentans inhibits the activity of cellular DNA topoisomerase I by activation of PARP1 and alters the efficacy of its anti-cancer inhibitor. PLoS One 8(8): e72377
22. Cann, A. J. 2013. Mycoplasma pneumoniae. Flickr. Retrieved from https://www.flickr.com/photos/ajc1/8726402100.
23. McNally, L., M. Viana, and S.P. Brown. 2014. Cooperative secretions facilitate host range expansion in bacteria. Nature Communications. 5.