Anthrax in the United States
Introduction
Anthrax, which means 'coal' in Greek, is a severe disease caused by the bacteria Bacillus anthracis, which stays alive in its surroundings by sporulating. Because of this protective measure, the disease itself is fairly old and can be found naturally on all continents, including Asia, southern Europe, sub-Sahelian Africa and Australia [1]. Anthrax can be contracted by humans and herbivorous animals, though other infected mammals and birds have been found [2].
Besides being a threat to the human population, anthrax has also been used in acts of biological warfare. The spores are easily transmitted, and the disease itself (especially inhalational anthrax) has a high mortality rate, making it an effective weapon to spread through a human population.
Description of Anthrax
Anthrax is a zoonotic disease that can infect both humans and animals [3]. Although human contact does not spread the disease, humans can get infected from touching or inhaling spores from contaminated animal products. Even eating rare meat from an infected animal is enough to cause anthrax. Most human cases occur due to contact with sheep, goat, and cattle, as well as wool and hides. Fortunately, anthrax is not a major health concern in today's society, although outbreaks have been know to occur. The largest known epidemic took place in Zimbabwe and lasted for 6 consecutive years (1979-1985). Infected cattle lead to an estimated 10,000 human cases [3].
Anthrax is generally known to be a seasonal disease, simply because temperature can affect how and when an animal may become infected from contact with the spores [4]. Symptoms of the disease will generally appear within 7 days after infection [5]. The infection can affect the skin, respiratory tract, and gastrointestinal tract.
Cutaneous Anthrax
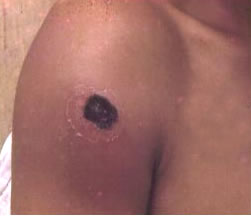
The most common type of anthrax, cutaneous (skin) anthrax, happens when a person has a cut of some type on the skin, allowing the bacteria to enter. An itchy lesion usually forms at this site, but after 1-2 days, it turns into a vesicle, and later, an ulcer. The surrounding lymph nodes are may also be subject to swelling. The ulcer, generally 1-3cm in diameter, contains a black necrotic (dead) center and is typically painless. However, if left untreated, approximately 20% of cutaneous anthrax cases can lead to death [6].
Respiratory (Inhalational/Pulmonary) Anthrax
Respiratory anthrax, also known as inhalational or pulmonary anthrax, is contracted by breathing in the anthrax spores. It has similar symptoms to the cold and flu for the first few days – a sore throat, muscle aches, and fever are often common. However, the disease then deviates, resulting in acute breathing difficulty and shock, which is often fatal. Untreated cases have a 100% mortality rate [3].
Gastrointestinal Anthrax
Gastrointestinal anthrax usually results from eating infected meat. The infection severely inflames the intestines, causing severe diarrhea and vomiting of blood, initially preceded by nausea, decreased appetite, and fever. If it goes untreated for long enough, toxaemia and shock will occur, leading to death. Gastrointestinal anthrax can also occur in the oropharyngeal – the symptoms then become a sore throat, difficulty in swallowing, fever, swollen lymph nodes, and toxaemia. Even with treatment, about 50% of oropharyngeal anthrax infections are fatal. http://www.who.int/mediacentre/factsheets/fs264/en/
The Bacillus anthracis Microbe
Microbewiki Link: Bacillus anthracis
Discovery
In 1887, Robert Koch showed that Bacillus anthracis could form endospores, and caused anthrax when injected into animals. It was also the first organism used to develop a vaccine with a weakened strain. (6)
Structure
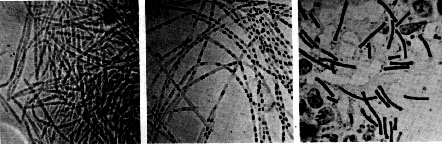
Gram-positive cells share cell walls made of peptidoglycan, techoic acids, lipoteichoic acids, capsular polysaccharides, and S-layer crystalline proteins for their cell structure, but Bacillus anthracis differs by being surrounded by its poly-D-glutamate capsule instead of a polysaccharide capsule, having no techoic acid, and having non-glycosylated S-layer proteins. (7) It is large and rod shaped and about 1-1.2um wide, and 3-5 um long. It is capable of growing both in aerobic and anaerobic conditions. It is similar to Bacillus cereus and Bacillus thuringiensis both genotypically and phenotypically, and all are able to form spores. (8) When faced with starvation, Bacillus anthracis is capable endospore formation. Spores are capable of resisting heat, cold, dessication, radiation, and disinfectant. This allows the spores to survive in inhospitable environments and germinate when conditions are more favorable. (8) Bacillus anthracis is also capable of forming biofilms which allow it to be resistant to the host immune system and antibiotics. (9)
Virulence
Bacillus anthracis has the ability to synthesize virulence factors.(6) Virulence factors pXO1, anthrax toxin, and pXO2, capsule gene, are responsible for the pathogenicity. They are both required for the virulence of Bacillus anthracis. The capsule is made up of a poly-D-glutamate polypeptide. The capsule is either “smooth” or “rough”, which is not virulent. The capsule gene both protects against phagocytosis and mediates the bacterial infection of the bloodstream. Bacillus anthracis capsule and anthrax toxin grow in response to increased atmospheric Co2. (8) Three components contribute to the anthrax toxin, the edema factor (EF), protective antigen (PA), and the lethal factor (LF). The edema factor increases fluid build up in the cells while the lethal factor promotes cell death and bacterium release. (6)
Combinations of these factors cause these results in experimental animals:
PA+LF is lethal
EF+PA causes edema
EF+LF is inactive
PA+LF+EF causes edema and necrosis, and is lethal
(8)
Transmission of disease
How is it transmitted? Is there a vector (animal/insect)?
Problems with Anthrax in America
Outbreak of anthrax in the United States
Although human anthrax was historically known to be contracted from high exposures to animals and animal products that were infected with Bacillus Anthracis [1], the spread of human anthrax in the United States took on a different approach. Moreover, research into prevention and medication of two types of anthrax, cutaneous and inhalation anthrax, were known and established, but the sudden outbreak came as a shock. The problem arises during early October to November in 2001, as the United States of America announced its first ten confirmed cases of human anthrax from bioterrorism [3]. The outbreak of this disease was caused by inhalation of anthrax from exposure of the disease.
Spread of anthrax in the U.S.
Intentional contaminated letters and packages were mailed to various districts of the U.S., targeted victims remained helpless and vulnerable to the Bacillus anthracis spores upon opening and handling. The packages held within them various infective powders and materials anticipated to be delivered to abortion clinics, reproductive health clinics, and other destinations such as government offices [2]. As a result from this event, the U.S. postal office was affected drastically as all of the initial patients were either employees of the postal office, mail handlers and sorters [3].
Effects of anthrax on the U.S. citizens
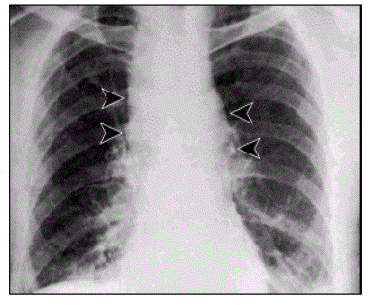
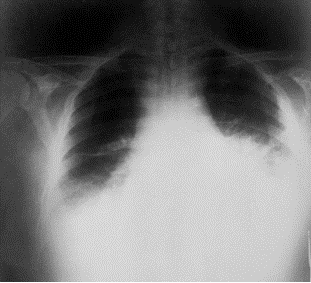
The problem caused by this hazardous disease in America results in various health issues along with social disruption and an economic crisis [2]. Victims experienced chills, a fever, difficulty coughing, constant sweats, fatigue, and typical feelings of morning sickness; nausea and vomiting. As an outcome of the ten initially infected citizens, all displayed abnormal chest x-rays; infiltrates, mediastinal widening, and pleural effusion [3]. With efforts to restore health to the ten patients, methods of multiple drug antibiotics were used along with guidance and supportive care, however only 60% of the initial ten patients survived. Overall, an alarming 22 cases were suspected to be infected from the anthrax contaminated mails . Among the twenty-two infected, five were announced dead, and of those five all were infected with inhalation anthrax [2]. This event not only stimulated a massive public health alarm in the United States, but in international countries as well. The 2001 anthrax attacks organized by bioterrorists proved its ability to cause not only destruction to the citizens of U.S., but also its ability to interfere with social and economic status.
Prevention
In the United States, the primary way to reduce the risk of exposure is through controlling the livestock. Proper disposal of anthrax infected carcasses and vaccination of at risk herds can help reduce exposure. The most effective and proper way of eliminating the exposure is through incineration of the contaminated soil. Patients that have died from anthrax should be isolated and contaminated materials should be properly disposed of through incineration. It is important that following the first detection of an anthrax infection in a herd, the surrounding animals should be removed and isolated from the field. The animals will then need to be monitored for a period of time and all the animals should be vaccinated if needed.
Vaccines
Vaccines can be used to prevent the disease in humans and animals. In the United States however, only high-risk groups such as military personnel are given the vaccine. Vaccine is not recommended for public use in the United States as anthrax cases are very rare and potential adverse side effects have been reported in some patients.
Anthrax Vaccine Adsorbed(AVA)
Anthrax Vaccine Adsorbed (AVA) is the only licensed human vaccine in the United States. The vaccine does not contain any dead or living bacteria cells but rather anthrax protective antigen protein so that vaccine cannot give an infection to the person. In a controlled study in which 379 employees received the vaccines, 414 received placebo, and 340 received neither vaccines or placebo, the study documented a vaccine efficacy of 92.5% for protection against anthrax (cutaneous and pulmonary). The duration of this protection is unknown in humans but in animals it has been known to have an effect from one to two years after two doses.
Treatment
Antibiotics
Antibiotics can be used before and after the patient has come in contact with the disease. This therapy is shown to result in a substantial recovery in individuals and animals infected with anthrax if taken immediately. Antibiotics can also be used for prevention and treatment in asymptomatic patients that may have been in exposed to the anthrax but have shown to have less of an effect on the spore form of the disease. It is important to note that antibiotics can kill the bacteria, but do not have an effect on anthrax toxins so late treatment of the infection can be detrimental.
What else could be done to address this problem
Are there solutions that could be successful but haven't been implemented due to political or economic reasons? Are there successful efforts in other countries? Are there reasons why these efforts may or may not be successful in the country you've focused on? etc. etc.
References
[1] World Organization for Animal Health, World Health Organization, Food and Agriculture Organization of the United Nations. Anthrax in Humans and Animals. 2008. 4th Edition. P. 3, 36-40]
[2] World Health Organization. The World Health Report 2007 - A Safer Future: Global Public Health Security in the 21st Century. 2007. Ch. 3, New Health threats in the 21st Century. p.35-37]
[3] John A. Jernigan, David S. Stephens, David A. Ashford, Carlos Omenaca, Martin S. Topiel, Mark Galbraith, Michael Tapper, Tamara L. Fisk, Sherif Zaki, Tanja Popovic,* Richard F. Meyer,* Conrad P. Quinn, Scott A. Harper, Scott K. Fridkin, James J. Sejvar, Colin W. Shepard, Michelle McConnell, Jeannette Guarner, Wun-Ju Shieh, Jean M. Malecki, Julie L. Gerberding, James M. Hughes, Bradley A. Perkins, members of the Anthrax Bioterrorism Investigation Team, Centers for Disease Control and Prevention, Atlanta, Georgia, USA; Emory University School of Medicine, Atlanta, Georgia, USA; Cedars Medical Center, Miami, Florida, USA; Virtua Health, Mount Holly, New Jersey, USA; Winchester Medical Center, Winchester, Virginia, USA; Lenox Hill Hospital, New York City, New York, USA; and Palm Beach County Department of Public Health, West Palm Beach, Florida, USA. Bioterrorism-Relation Inhalational Anthrax: The First 10 cases Reported in the United States. 8 November 2001. p. 1-36]
[4] World Health Organization, Global Alert and Response. "Guidance on Anthrax."
[5] World Health Organization, Fact Sheet. "Anthrax." 2001.
[6] World Health Organization, Initiative for Vaccine Research. "Zoonotic Infections." p.2.
[7] World Health Organization. "Guidelines for the Surveillance and Control of Anthrax in Humans and Animals." 3rd Edition. p 1-20.
[8] Centers for Disease Control and Prevention. "Anthrax: What You Need To Know." 2003.
[9] Centers for Disease Control and Prevention. "Anthrax: Signs and Symptoms." 2003.
[10] NCBI Entrez Genome Project
[11] Choudhury, B., Leoff, C., Saile, E., Wilkins, P., Quinn, C., Kannenberg, E., and Carlson, R. "The Structure of the Major Cell Wall Polysaccharide of Bacillus anthracis Is Species-specific". J. Biol. Chem. Sep 2006. 281: 27932 - 27941.
[12] Todar, K. "Todar's Online Textbook of bacteriology."
[13]
Lee, K., et al. "Phenotypic and functional characterization of Bacillus anthracis biofilms". Microbiology. 2007. 153. 1693-1701.
[14] National Institute of Allergy and Infectious diseases. "Anthrax."
[15] Centers for Disease Control and Prevention. "Use of Anthrax Vaccine in the United States." Advisory Committee on Immunization Practices Membership, October 2000
[16] World Health Organization. "Anthrax." October 2001.
Edited by Kai Kuo, Maggie Chan, Miya Yoshida, Eric Ku, Stephen Chin, students of Rachel Larsen