Blood Glucose Regulation
Introduction
Blood glucose regulation involves maintaining blood glucose levels at constant levels in the face of dynamic glucose intake and energy use by the body. Glucose, shown in figure 1 is key in the energy intake of humans. On average this target range is 60-100 mg/dL for an adult although people can be asymptomatic at much more varied levels. In order to maintain this range there are two main hormones that control blood glucose levels: insulin and glucagon. Insulin is released when there are high amounts of glucose in the blood stream.
Glucagon is released when there are low levels of glucose in the blood stream. There are other hormones that effect glucose regulation and are mainly controlled by the sympathetic nervous system. Blood glucose regulation is very important to the maintenance of the human body. The brain doesn’t have any energy storage of its own and as a result needs a constant flow of glucose, using about 120 grams of glucose daily or about 60% of total glucose used by the body at resting state. [1] With out proper blood glucose regulation the brain and other organs could starve leading to death.
Hormones
Insulin
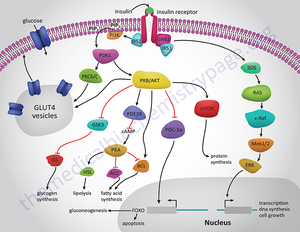
A key regulatory pathway to control blood glucose levels is the hormone insulin. Insulin is released from the beta cells in the islets of Langerhans found in the pancreas. Insulin is released when there is a high concentration of glucose in the blood stream. The beta cells know to release insulin through the fallowing pathway depicted in figure 2. [2,3]Glucose enters the cell and ATP is produce in the mitochondria through the Krebs cycle and electron transport chain. This increase in ATP causes channels to closes. These channels allow potassium cations to flow into the cell. [2,3,]With these channels closed the inside of the cell becomes more negative causing calcium channels to open allowing calcium cations to flow into the cell. Calcium cation ions flow into the cell due to a concentration and elector chemical gradient that favors the influx of calcium cations. Calcium ions are key in the vesicle excretion processes. A protein on the vesicle called the v-SNARE protein becomes entangled with a t-SNARE protein on the beta cell surface. With calcium facilitating the interaction amongst the SNARE proteins the vesicle is forced to merge with the cell membrane and insulin is excreted into the blood stream.[2,3,4,5]
Insulin travels through the blood stream to muscle, brain or adipose tissue. Once there, the insulin binds to a dimeric transmembrane receptor. This receptor autophosphorylates and causes many downstream pathways relating to glucose regulation, energy storage and DNA transcription. For the glucose regulation pathway the receptor autophosphorylates then causes insulin receptor substrate 1 (IRS-1) to be phosphorated[2,3,4]. IRS-1 then phosphorylates Phosphatidylinositol 3-kinase (PI3K). PI3K cleaves Phosphatidylinositol 4,5-bisphosphate (PIP2) leaving diacyl glycerol (DAG) in the cell membrane and inositol 1,4,5-trisphosphate (IP3) in the cytosol. IP3 travels to the smooth endoplasmic reticulum (SER) and cause calcium channels to open in the SER, releasing cations into the cytosol. DAG activates a kinase named protein kinase C which also opens calcium channels in the SER.[2,3] This ambient increase in calcium facilitates the binding of vesicles to the membrane. These vesicles have Glut4 proteins imbedded in the membrane. Glut4 proteins are channel proteins that allow glucose into the cell. Once these vesicles bind with the cell membrane glucose flows through the Glut4 protein and into the cell, reducing blood glucose levels.[2,3] The process by which insulin is degraded and metabolized is poorly understood. However it is known that the liver is responsible for the majority of insulin break down. Since the liver is so important to proper insulin levels when the liver is damaged perhaps by alcohol the regulatory system can be interfered with. Alcohol effects on the regulation of blood glucose will be addressed later in this article. The kidney is also key in the break down of insulin. Peripheral tissue is thought to hold on to insulin perhaps reversibly binding to membrane receptors.[6] These means it is possible for insulin to be removed from the blood stream with out being broken down. Insulin clearance rates are shown to decrease in those who are obese or have diabetes. This may create insensitivity to insulin. [7]
Glucagon
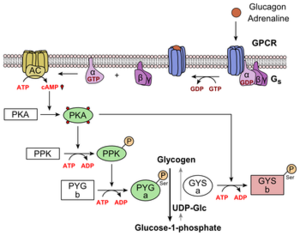
When blood glucose levels are low, glucagon is released which inhibits the break down of glucose, glycolysis and activates the formation of glucose, gluconeogenesis. Gluconeogenesis creates glucose from such molecules as pyruvate, lactate, glycerol, and glucogenic amino acids. Glucagon is released from the alpha cells of the islets of Langerhans in the pancreas.[8] Glucose is brought into the cell through SLC2A1 channel proteins. The glucose is then used to generate ATP. This increase in ATP opens potassium channels unlike in beta cells where they are inhibited. This increase in intercellular potassium causes calcium channels to open which facilitates the binding of vesicles contain glucagon. Glucagon is then released into the blood stream. This pathway is shown in figure 3 Glucagon primarily operates on the liver. Once the hormone has made it through the blood stream to the liver it binds to a transmembrane protein called a G protein coupled receptor(GPCR). The associated G protein is phosphorylated with GTP and the alpha unit of the G protein moves to activate adenylate cyclase (AC). AC converts ATP into cyclic AMP (cAMP). [8,9] Cyclic AMP activates protein kinase A (PKA). PKA phosphorylates phosphofructokinase-2 (PFK-2) and fructose bisphosphatase- 2(FBPase-2). Due to the addition of the phosphate PFK-2 becomes less active. This in turn reduces the amount of fructose 2,6-bisphosphate (F-2,6-BP) being produce. High levels of F-2,6-BP cause glycolysis or the break down of glucose.[8,9] So less active PFK-2 decreases the amount of F-2,6-BP. In addition FBPase-2 is activated which breaks downs F-2,6-BP which also decreases the amount of F-2,6-BP. Low levels of F-2,6-BP cause the activation of FBPase-1 which increase gluconeogenesis. In addition there is no activation of PFK-1, which is involved in glycolysis both of these actions increase the amount of blood glucose.[9]
Epinephrine
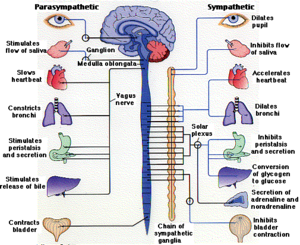
During extreme stimuli the sympathetic nervous system kicks into action. This is colloquially known as the fight or flight response illustrated in figure 4. The brain sends signals throughout the body to increase heart rate, cause bronchial dilation and haptic glucose release. The brain also sends signals to the adrenal glands. Epinephrine is released from the adrenal glands. This hormone is key to the prolonged sympathetic response. [4,10]Epinephrine produces similar results as the initial neuronal signal however it is longer lasting. Epinephrine travels through the blood stream and causes the liver to release glucose thus increasing blood glucose levels in order to be ready for the threat. [4,10] The pathway by which this occurs is outlined here. Epinephrine binds to a transmembrane receptor on the liver known as the beta-adrenergic receptor protein. The receptor activates a G protein which then activates. [4,11]The G protein activates by swapping out at GDP for a GTP. Once activated the G protein diffuses along the membrane. The G protein then binds with and activates adenylyl cyclase. Adenylyl cyclase causes ATP to become cyclic AMP (cAMP).The molecule cAMP binds with protein kinase-A which phosporalayts specific proteins. In this step phosphorylase is phosphorylated.[4,11] Phosphorylase then cuts glucogen creating a glucose-1-phosphate. This is further refined into glucose-6-phosphate by phosphoglucomutase. Glucose-6-phosphate can then be used for energy requirements necessary in the sympathetic nervous system response. This allows for more ATP in the muscle and brain.[4,11] This hormone pathway is reversed when the parasympathetic nervous system takes priority.This system is sometimes referred to as the “rest and digest”.[10,11] An experiment was conducted by Cherrington and colleagues that looked at the effects of blood glucose levels after exogenic epinephrine was inserted. This experiment conducted in conscious dogs looked at hepatic glucose release and showed a 50% increase in hepatic glucose release in response to an amount of epinephrine seen in a moderate stress response.[21,22]
Diabetes Mellitus
When there is a issue with the ability of the human body to use glucose due to a problem with the insulin pathway diabetes mellitus (diabetes mellitus) may be at fault. There are a few types of diabetes mellitus with the most common being: type 1 diabetes mellitus, type 2 Diabetes mellitus and gestational Diabetes mellitus.[12,13]
Type 1
Type 1diabetes mellitus is often discovered early in a persons’ life and has also been called juvenile diabetes mellitus. Type 1 diabetes mellitus is where no insulin is made. This is due to damage to the pancreatic beta cells, often due to an autoimmune disorder. With out insulin the glucose can not go into the cells and will not make energy. As a result treatment for type 1 diabetes mellitus is regular injections of insulin. [12,13]
Type 2
Type diabetes mellitus is a condition where the body becomes resistant to insulin or not enough insulin is made. People who are obese have a high risk for contracting type 2 Diabetes mellitus. Although there is no cure for type 2 careful monitoring of exercise and nutrition can help.
Other effects of the body are in increased rate of stroke and heart issues. Also damage to small blood vessels can occur. This happens particularly in the eyes (diabetic retinopathy) and kidneys (renalopathy). Also due to increased amounts of sugar in the blood stream a diabetic is at a higher risk of infection and wounds will take longer to heal.[12,13]
Alcohol effects on glucose regulation
Alcohol rapidly effects glucose levels in the blood stream which can be a challenge for those dealing with Diabetes mellitus. Alcohol effects many parts of the body and as a result has many pathways for effecting blood glucose levels. Alcohol can cause one to make poor decisions which will effect how you eat, this very directly effects blood glucose levels. [14,15]Alcohol also interacts with the hypothalamus which is responsible for, amongst other things, the drive to feed.[14] Beyond the neurological effects of alcohol on the body there are metabolic effects as well.This effect is more dramatic with drinks high in carbohydrates such a beer. The carbohydrates in beer can be metabolized and create glucose creating a temporary increase in blood glucose levels. Alcohol has energetic properties to its molecular structure and as a result the body can gain energy from it. Through the use of enzymes: alcohol dehydrogenase, cytochrome P450, catalase alcohol is broken down. Alcohol dehydrogenase, the main enzyme in this catabolic reaction, produces NADH.NADH is the energy molecule that drives lactic acid formation. Glucose is turned into pyruvate through the use of ATP and then into lactic acid with NADH. This increase of NADH leads to a decrease in glucose [15]. The enzyme cytochrome P450 is activated when heavy drinking occurs. This enzyme strips an electron from NADPH in the metabolism of alcohol, which requires energy.[15,16] This is another mechanism by which blood glucose levels would fall after drinking. However studies on the effects of alcohol leave one wanting for straight forward data on blood glucose levels in real life situations. In an article published by Gin et al. the findings show no adverse effects on diabetic participants after moderate alcohol consumption. The American Diabetes Association and other medical information outlets concur with this finding, that moderate consumption of alcohol produce no adverse effects. However acute ingestion of alcohol has also been reported to increase insulin secretion, resulting in low blood glucose.[15,17]
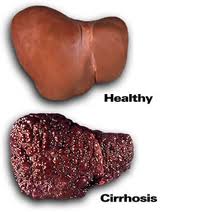
Research also indicates that heavy drinking will cause insulin to become ineffective, resulting in high blood sugar levels. It is unclear if the high blood sugar levels are from heavy drinking alone or are connected to obesity. Further complicating this is a high correlation between heavy drinking and obesity. Also a review of the effects of alcohol indicates that both glycolysis and gluconeogenesis will be inhibited. (cederbaum,2012) As the liver is key in the release of glucose into the blood stream and issue with it can prevent healthy maintenance of blood glucose levels. With heavy drinking the liver will become fatty reducing it’s effectiveness at releasing energy stores. A disease where inflammation of the liver causes problems with the liver function is called alcoholic hepatitis. The liver can also become hard with heavy drinking due to scare tissue formation this is called fibrosis this is shown in figure 5. The pancreas is vital for blood glucose regulation and alcohol can have a significant effect on this organ. The pancreas creates digestive enzymes to metabolize the alcohol and these enzymes destabilize the cell membrane of the pancreatic cells. This leaves the cell liable to auto-digestion.
Gut Bacteria
A connection has been shown between decreased gut bacteria diversity and obesity.[18] Obesity is a risk factor for T2DM. [19] However a causal relationship between gut microbiota and obesity has yet to be proven.[18] In addition obesity doesn't necessarily cause one to have T2DM. In the united states 34% of adults are obese where only 11% have T2DM.[19] It is possible that a change in gut micro flora could cause diabetes but that connection has yet to be shown. An experiment preformed by Bäckhed and colleagues that could shed light on this showed a germ free mice maintained 40% less body weight compared to control mice. This trend was still seen in germ free mice who received a feeding regiment so that their caloric intake was 29% higher than conventionally raised mice. When these mice received gut microbiota their body fat increase 57% and became "dramatically insulin resistant".[18,20]
Conclusion
All cells in the human body require glucose to survive. However excessive amounts of glucose can also be detrimental to the body. In order to maintain this balance the body uses hormonal regulation. The body will detect high levels of blood glucose and release insulin to allow the sugar into cells. If there is not enough blood glucose, glucagon will be released. This hormone will cause the formation of glucose and the release of glucose stores. If the body is presented with a threat it will initiate the sympathetic nervous system. Part of this response is the release of epinephrine which causes haptic glucose release. If the body can not properly regulate blood glucose levels than it may be a form of diabetes. Diabetes type one stems from an inability to produce insulin. Diabetes type two is due to an insensitivity to insulin. Due to the blood glucose regulatory systems wide reach on the body when alcohol which also has a whole body effect a reaction is bond to occur. Blood glucose levels may initially increase however this is only in the case of high carbohydrate alcoholic beverages, such as beer. Due to the metabolism of alcohol glucose will be turned into pyruvate and blood glucose levels will drop. Alcohol's effects on judgment are also likely to lead to a drop in blood sugar.
References
[1] Berg JM, Tymoczko JL, Stryer L. Biochemistry. 5th edition. New York: W H Freeman; 2002. Section 30.2, Each Organ Has a Unique Metabolic Profile. Available from: http://www.ncbi.nlm.nih.gov/books/NBK22436/
[2] Chang, L., Chiang, S.-H., & Saltiel, A. R. (2004). Insulin Signaling and the Regulation of Glucose Transport. Molecular Medicine, 10(7-12), 65–71. http://doi.org/10.2119/2005-00029.Saltiel
[3][ndsuvirtualcell] (Dec 3, 2009) Insulin Signaling (Signal Pathways)(YouTube) Retrieved from:https://www.youtube.com/watch?v=FkkK5lTmBYQ Gin H1, Morlat P, Ragnaud JM, Aubertin J. (1992) Short-term effect of red wine (consumed during meals) on insulin requirement and glucose tolerance in diabetic patients. Retrieved from:http://www.ncbi.nlm.nih.gov/pubmed/1499475
[4][Moof University] (Dec 3, 2013) Insulin Signaling Cascade - Receptor Tyrosine Kinase (YouTube )Retrieved from: https://www.youtube.com/watch?v=2YR1XmYF5hM
[5]Albertsr. (n.d) Essential Cell Biology: Fourth Edition. New York: Garland Science.
[6] WILLIAM C. DUCKWORTH and ABBAS E. KITABCHI(1981) Insulin Metabolism and Degradation Endocrine Reviews 2:2, 210-233 Kovacs B, Stoppler M (2014) Alcohol and nutrition Retrieved from:http://www.medicinenet.com/alcohol_and_nutrition/page4.htm
[7] William C. Duckworth, Robert G. Bennett, and Frederick G. Hamel (1998) Insulin Degradation: Progress and Potential Endocrine Reviews 19:5, 608-624
[8]Quesada, I., Tuduri, E., Ripoll, C., & Nadal, A. (2008). Physiology of the pancreatic -cell and glucagon secretion: Role in glucose homeostasis and diabetes. Journal of Endocrinology, 5-19.
[9] [Moof University] (Dec 3, 2013) Glucagon Signaling Cascade - GPCR (G-Protein Coupled Receptor) (YouTube)Retrieved from:https://www.youtube.com/watch?v=1ImdVTWKiqs9
[10] Bear, M(n.d) Neuroscience: Exploring the Brain. New York: Wolter Kluwer
[11] Krantz,B Principles of Metabolic Regulation, Illustrated with Glucose and Glycogen Metabolism [pdf] Retrieved from:https://mcb.berkeley.edu/labs/krantz/mcb102/lect_S2008/MCB102-SPRING2008-LECTURE7-METABOLIC_REGULATION.pdf
[12] American Diabetes Association. (n.d.). Retrieved December 12, 2015, from http://www.diabetes.org
[13]Dansinger, M. (Ed.). (2014, September 2). Controlling Diabetes: When Pills Are Not Enough, With Pictures. Retrieved December 12, 2015, from http://www.webmd.com/diabetes/controlling-diabetes-14/slideshow-control-your-blood-sugars
[14]Yeomans, M. (n.d.). Short term effects of alcohol on appetite in humans. Effects of context and restrained eating. Appetite, 565-573.
[15] HAMS: Harm reduction for alcohol (How Alcohol Is Metabolized in the Human Body) http://www.hamsnetwork.org/metabolism/
[16]Caton, S., Ball, M., Ahern, A., & Hetherington, M. (n.d.). Dose-dependent effects of alcohol on appetite and food intake. Physiology & Behavior, 51-58.
[17]Cederbaum, A. I. (2012). ALCOHOL METABOLISM. Clinics in Liver Disease, 16(4), 667–685. http://doi.org/10.1016/j.cld.2012.08.002
[18] Musso, G.(2010). Obesity, Diabetes, and Gut Microbiota The hygiene hypothesis expanded?, vol. 33 no. 10 2277-2284.doi: 10.2337/dc10-0556
[19]Eckel, R. (2011). Obesity and Type 2 Diabetes: What Can Be Unified and What Needs to Be Individualized?vol. 34 no. 6 1424-1430.doi: 10.2337/dc11-0447
[20] Bäckhed F, Ding H, Wang T, Hooper LV, Koh GY, Nagy A, Semenkovich CF, Gordon JI: The gut microbiota as an environmental factor that regulates fat storage. Proc Natl Acad Sci U S A 2004;101:15718–15723
[21] Cherrington AD, Diamond MP, Green DR, Williams PE: Evidence for an intra- hepatic contribution to the waning effect of glucagon on glucose production in the conscious dog. Diabetes 31:917–922, 1982
[22] Cherrington AD,(1997) Control of Glucose Uptake and Release by the Liver In Vivo [pdf]. Retrieved from: http://rodrigoborges.hospedagemdesites.ws/principal/pdf/endocrino_07.pdf
