Gut Flora and Autism: Difference between revisions
Aamy.yiwang (talk | contribs) |
No edit summary |
||
| Line 1: | Line 1: | ||
{{Uncurated}} | |||
=Introduction= | =Introduction= | ||
Latest revision as of 18:28, 1 October 2015
Introduction
Autism Spectrum Disorder
Autism spectrum disorder (ASD) is the category of which autism falls under. ASD describes a range of neural development disorders which normally manifests in children before 18 months of age but late onset can occur after 18 months [1,2]. There are different degrees of ASD with varying symptoms among individuals. It is usually characterized by difficulties in social interaction, repetitive behaviour and delays in understanding language [2]. The etiology of autism is unknown. However, autistic children have been reported to suffer from severe and frequent gastrointestinal (GI) problems which suggests that there may be a link between autism and the gut [3,4].
The Human Gut
It is estimated that there are about 300-500 different species of bacteria that form a mutualistic interaction with the human digestive tract to provide metabolic, immune and protective functions [5]. Gut flora aid in the fermentation of non-digestible dietary residue and carbohydrates. They also help produce short chain fatty acids. The gut microbiome consists mainly of bacteria from two phylum Firmicutes and Bacteroidetes [5].
Research
GI problems include diarrhea, unformed stools, constipation, bloating and/or gastroesophageal reflux. Among the autistic population, GI problems are a common occurrence, as shown in a 2011 study where 63% of the autistic children had GI problems compared to the 2% of the control group that had GI problems[3]. The control group refers to the group of children who do not have autism.
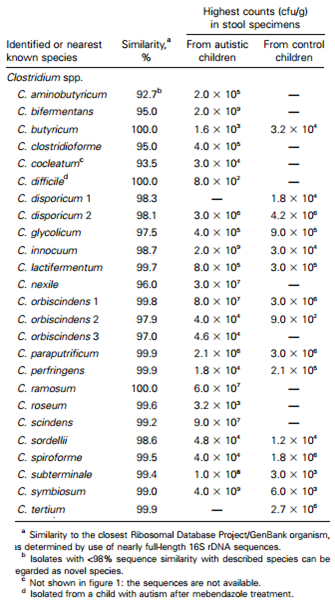
In 2002, stool, gastric juice and duodenal fluid samples from collected from various children hospitals from autistic patients with a history of GI problems and were examined [6]. In total, 25 different species of Clostridium were encountered, 9 of which were found exclusively in the gut of autistic children while 3 species were only found in the control (6). Clostridium difficile, a species that was found only in autistic stools, is known to be a major cause of severe GI diseases through its production of enterotoxin A, which is responsible for various GI symptoms through an unknown mechanism [7]. Another study published in April of 2012 found that those with late onset autism have been shown to have higher counts of Desulfovibrio in their fecal matter via pyrosequencing but Clostridium was not isolated [1].

]
Mechanism
Clostridium is a genus of Gram-positive, obligate anaerobic, spore-forming bacteria while Desulfovibrio is a genus of Gram-negative and aerotolerant bacteria [8]. Their metabolism produces short-chain fatty acids (SCFA) from carbohydrates and amino acids. Increased levels of SCFA present in circulating blood can cross the blood brain barrier where they affect brain development and function [9]. Propanoic acid (PPA) is a type of SCFA known to influence cell signaling, neurotransmitter synthesis/ release, mitochondrial function and gene expression [9]. It interferes with cellular metabolism by overwhelming the metabolic functions of the mitochondria to cause oxidative dysfunction and stress [8]. Increased PPA over the developmental time period may play a role in the development of autism and other neurodevelopment disorders [7].
Rat Model
An experiment performed in 2008 tested the hypothesis that increased levels of PPA resulted in autistic-like characteristics such as impaired social behaviour [10]. 114 adult male rats were randomly selected into the following groups: PPA, propanol control, sodium acetate (SA) control and phosphate buffered saline control (PBS) [10]. Sodium acetate is produced in the gut from carbohydrate fermentation and propanol is a non-acidic analog of PPA.
Behaviour was analyzed with two rats of the same experimental conditions and data was collected on the following variables via a video tracking software: mean distance between rats, percent of time rats spent within 5cm proximity of each other and total distance travelled by an individual rat [10]. Additionally, the rats were videotaped and evaluated for playfulness based on frequency of play initiations, number and type of defenses evoked [10].
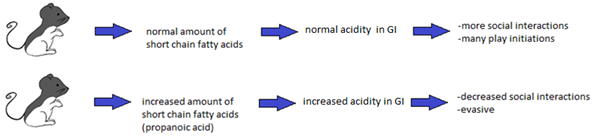
The results showed that the rats with injected PPA had consistently impaired social behaviour. PPA injected rats exhibited a greater distance apart, spent less time within a 5cm proximity to each other, had less play interactions, and were more likely to show evasive defenses [10]. These findings support that increased PPA levels somehow impair social behaviour. SA rats initially showed these behaviours as well, but they decreased as time progressed [10]. Propanol and PBS injected rats did not show any of the above behaviours [10]. The rats were not tested for the presence of Clostridium or Desulfovibrio.
Treatments
There are no studies published on the use of antimicrobial agents against Desulfovibrio but there was a trial study based on the use of oral vancomycin on late onset autistic children with a history of chronic diarrhea. Vancomycin is an antibiotic used to treat infections caused by Gram-positive bacteria, making it very effective against Clostridium but ineffective against Desulfovibrio [11]. The hypothesis was that the protective function of gut flora was compromised due to the use of antimicrobial agents, which allowed the colonization of Clostridium [11].
Post and pre-treatment behaviours of the patients were videotaped and evaluated by a clinical psychologist. It was found that 8 out of 10 of the autistic patients had improved behaviour [11]. They were less aggressive, had increased eye contact and improved in their receptive language and speech. Most of their GI problems also went away. Unfortunately, follow up indicated that the effects of vancomycin were short term and the children returned to their previous behaviour [11]. It is speculated that the spores of Clostridium were unaffected by the treatment which may have led their recolonization [11].
Conclusions
From the above findings, it does seem that there is a strong link between Clostridium and Desulfovibrio species and autism. Though exact mechanisms are unclear, they do seem to produce products as part of their metabolism to somehow disturb the central nervous system. The evidence seems to suggest that the acidity of PPA may affect the gut as the non –acidic analog of PPA did not show any autistic-like behaviour. These findings only relate to a subset of autistic patients who have GI issues and not the entire autistic population.
References
(1) Finegold SM. Desulfovibrio species are potentially important in regressive autism. Med Hypotheses. 2011 8;77(2):270-4.
(2) Gilger MA, Redel CA. Autism and the gut. Pediatrics. 2009 August 01;124(2):796-8.
(3) Adams JB, Johansen LJ, Powell LD, Quig D, Rubin RA. Gastrointestinal flora and gastrointestinal status in children with autism--comparisons to typical children and correlation with autism severity. BMC gastroenterology. 2011;11(1):22-.
(4) Parracho HM, Bingham MO, Gibson GR, McCartney AL. Differences between the gut microflora of children with autistic spectrum disorders and that of healthy children. J Med Microbiol. 2005;54(10):987-91.
(5) Guarner F, Malagelada J. Gut flora in health and disease. The Lancet. 2003 2/8;361(9356):512-9.
(6) Finegold SM, Marlowe EM, Collins MD, Lawson PA, Summanen P, Baysallar M, et al. Gastrointestinal microflora studies in late-onset autism. Clinical Infectious Diseases. 2002;35(S1):S6-S16.
(7) MacFabe DF, Cain DP, Rodriguez-Capote K, Franklin AE, Hoffman JE, Boon F, et al. Neurobiological effects of intraventricular propionic acid in rats: Possible role of short chain fatty acids on the pathogenesis and characteristics of autism spectrum disorders. Behav Brain Res. 2007;176(1):149-69.
(8) Macfabe DF. Short-chain fatty acid fermentation products of the gut microbiome: Implications in autism spectrum disorders. Microb Ecol Health Dis. 2012;23:1-24.
(9) Raymond H Thomas, Melissa M Meeking, Jennifer R Mepham, Lisa Tichenoff, Fred Possmayer, Suya Liu, et al. The enteric bacterial metabolite propionic acid alters brain and plasma phospholipid molecular species: Further development of a rodent model of autism spectrum disorders. Journal of Neuroinflammation. 2012;9(1):153-.
(10) Shultz SR, MacFabe DF, Ossenkopp K, Scratch S, Whelan J, Taylor R, et al. Intracerebroventricular injection of propionic acid, an enteric bacterial metabolic end-product, impairs social behavior in the rat: Implications for an animal model of autism. Neuropharmacology. 2008;54(6):901-11.
(11) Sandler RH, Finegold SM, Bolte ER, Buchanan CP, Maxwell AP, Väisänen ML, et al. Short-term benefit from oral vancomycin treatment of regressive-onset autism. J Child Neurol. 2000;15(7):429-35.