Host Defense Evasion Mechanisms of Rabies Virus
(Currently being edited)
Rabies Virus
Rabies virus (RABV) is a prototypical neurotropic virus and is often counted as one of the most deadly zoonotic diseases. Both wild and domestic animals can be afflicted with the disease and it is most commonly spread to humans via the saliva of an infected animal entering a bite wound or scratch. In Asia, most rabies infections are caused by rabid dogs. However in the Americas, and recently Australia and Western Europe, bat rabies has become a public health threat. Rabies is present on all continents except Antarctica, but the majority of rabies related deaths occur in Asia and Africa [1].
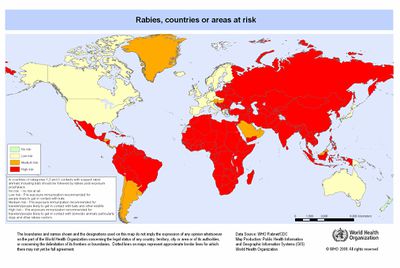
RABV infections occur mainly in remote, rural communities where measures such as vaccinating dogs to prevent animal to human transmission have not occurred. Due to lack of resources and preventative measures, 95% of rabies related human deaths occur in Africa and Asia. Most at risk populations generally do not have the ability to access nor the money for the rabies vaccine or post-exposure prophylaxis, turning a rabies infection into a death sentence [1]. Most patients survive for seven days after the onset of symptoms [2].
There are two main phylogroups of RABV which cause two distinct types of symptoms. Classical rabies, also known as furious rabies, causes 70% of animal and human infections while non-classical or paralytic rabies causes the remaining 30% of cases. Classical rabies is the more well-known strain and is characterized by symptoms such as hydrophobia, hallucinations, excited behavior, hyperactivity, and occasionally aerophobia. Paralytic rabies is less dramatic, as the patient’s muscles slowly become paralyzed with the paralysis radiating from the infection site. The patient eventually falls into a coma and dies. This non-classical form of rabies is often misdiagnosed, leading to an underrepresentation of the incidences of rabies [1][2]. Both forms of rabies cause death through cardiorespiratory arrest [1].
Great progress has been made in developing new rabies vaccines and preventative measures, but much of the molecular mechanisms of rabies virus remain a mystery. Improved genetic techniques that allow for direct manipulation of the rabies viral genome have given researchers a more detailed picture of rabies pathogenesis and a greater insight into virus-host cell interactions [2]. Understanding viral-host cell interactions are key to understanding how rabies virus is able to evade the host’s immune response and make its way from the site of infection to the central nervous system and the brain. A better understanding of these mechanisms could help improve neuronal labeling and nuerotracer studies and treatments for other central nervous system diseases [2].
Host Cell Mediated T Cell Apoptosis
T cells are the host’s method of controlling infections in the nervous system (NS). However, the T cell response in rabies victims is insufficient as it is inactivated by the virus [3].This inactivation was identified through immunohistochemical studies demonstrating that the host’s T cells were dying instead of the RABV infected neurons (cited in [3]). Infiltrating T cells have a difficult time in the NS as several neuropeptides and nuerotransmitters downregulate T cell activity [4]. Using attenuated RABV, it has been observed that infected brains upregulate expression of molecules such as somatostatin that are involved in limiting T cell activity in the NS [5]. However, it is important to note that attenuated and fatal strains of RABV act in different ways so whether the wild type encephalitic RABV elicits this response is uncertain.
Studies done in vitro and in vivo have shown that RABV uses an evasive strategy similar to that of tumor cells by upregulating certain surface molecules such as FasL and HLGA that trigger apoptosis in T cells [6][7]. It has been found that in mice lacking the functioning FasL ligand, there was a lower level of T cell apoptosis in the NS compared to control mice. This reduction in T cell apoptosis is possibly a contributing factor to the lower rates of RABV morbidity and mortality in these mice.
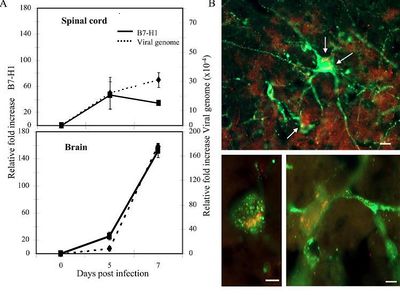
In silico experiments lead Lafon et al. to believe that B7-H1 is also involved in RABV’s immunoevasive strategy [8]. B7-H1 is a ligand of programmed cell death 1 (PD-1) and ligation of these two proteins inhibits T cell proliferation and cytokine production, leading to a lower immune response (cited in [8]). In human neuroblastoma cell cultures, RT-PCR was used in conjunction with flow cytometry to demonstrate that not only is B7-H1 upregulated in RABV infected cells versus non-infected cells, but that the upregulation of B7-H1 also leads to more surface expression [8]. RT-PCR and immunohistochemistry performed using samples from RABV infected mouse models, provide an in vivo example in upregulation of B7-H1 in the NS (Fig 2). Figure 2A shows a correlation between a relative fold increase of B7-H1 and relative fold increase of RABV genome in both the spinal cord and brain of infected mice [8]. Transcripts were measured at day 0, 5, and 7, post infection to get an accurate representation of expression levels in non-infected (day 0), early stage (day 5), and late stage (day 7) infected cells. In the immunohistochemistry experiment, it was discovered that B7-H1 (red) was expressed not only by infected neurons (green), but by non-infected cells as well (Figure 2B). This allows for an even greater immunoevasive environment.
Lafon et al. also went on to find that without B7-H1, RABV mortality drops significantly [8]. B7-H1 knockout mice were created and infected with either a viral dose of 100 or 50. Viral doses were determined by the amount of virus needed to reach 100% or 50% mortality in wild type mice. Wild type mice behaved according to expectations, while B7-H1 knockouts had a 50% mortality rate with a viral dose of 100 and a 0% mortality rate at a viral dose of 50 [8]. Additionally, B7-H1 mice were spared some of the symptoms of encephalitis such as hunchback. These results suggest that RABV nueroevasiveness was hindered with the absence of B7-H1 [8].
Strikingly, B7-H1 expression is only activated by innate immune responses such as interferons (IFNs), tumor necrosis factor alpha (TNF-alpha), and Toll-like receptors (TLRs) [8]. Therefore, neural B7-H1 should require activation of the innate immune system to be upregulated. This seems slightly paradoxical, as an immune response is required to increase expression of a protein that is used to kill T cells, another aspect of immune response. RABV has been shown to induce a strong type I IFN response in addition to a robust chemoattractive and inflammatory response [9]. This response is likely the cause for upregulation of B7-H1 in non-infected astrocytes and neurons. However, the INF response is quickly dampened, making it seem more like a quick burst [8]. RABV is able to evade and subvert this response as it likely that it uses this opportunity to establish B7-H1 production to ward off T cell in later stages of the infection.
RABV uses the immunosubversive molecules FasL and B7-H1 to protect against the host’s T cells. Cells expressing FasL and B7-H1 trigger apoptosis pathways in T cells expressing the Fas and PD-1 ligands upon binding. When the upregulation of these immunosubversive molecules is blocked, RABV virulence is drastically attenuated. However, these pathways cannot be turned on without an IFN response. Essentially, RABV hijacks systems already in place to create a more immunoevasive environment.
Prevention of Neuronal Apoptosis
While some neurotropic viruses such as West Nile virus or polio virus effectively kill motor neurons, RABV actively seeks to prevent neuronal degradation. RABV enters the NS through a neuromuscular junction or by passing through a synapse and utilizes the central nervous system as a transport system to the brain and salivary glands. Neuronal cell bodies, and possibly dendrites, are used for viral propagation and the virions travel in a retrograde direction towards the brain. Due to its dependence on neurons and the neuronal network the virulence of RABV might correlate to the survival of neurons [3]. In fact, motor neurons of non-human primates infected with RABV showed no signs of degradation four days post infection (cited in [3]).
To determine the nature of this correlation, Prehaud et al. compared the PDZ binding site of the envelope glycoprotein (G) in a virulent and attenuated strain of RABV [10]. PDZ domain activation is often used in signaling pathways and are used to regulate catalytic activity [3][10]. In preliminary in silico experiments, it was found that the cytoplasmic domain of the G protein had a putative PDZ binding site (PDZBS). The only differences between two virulent (VIR) and attenuated (ATT) strains of RABV are mutations in the cytoplasmic domain of the G protein. VIR has a His->Lue mutation in the cytoplasmic domain while ATT has a Gln->Glu mutation in the PDZBS of the G protein [10].
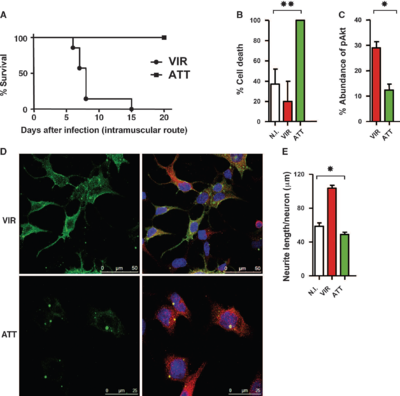
In vivo survival experiments were performed on mice exposed to either the VIR or ATT strain [10]. Over a 20 day period, 100% of mice infected with ATT survived while the VIR infected mice all succumbed to the disease by day 15 (Figure 3A). Human neuroblastoma cells were also infected with both strains and percent cell death, percent abundance of pAkt, and neurite length were all measured (Figure 3B, C and E). Cells infected with ATT had a significantly higher percent cell death than the VIR and non-infected cells, further supporting the idea that attenuated phenotype stems from higher levels of cell apoptosis (Figure 3B). Percent pAKt was measured as pAkt suppresses cell apoptosis pathways and the percent pAkt levels correlate with the percent cell death as ATT infected cells had significantly lower levels than VIR infected cells (Figure 3C)[10]. Neurites are neuron appendages such as dendrites and axons and it has been suggested that virulent strains induce neurite growth [3]. Figure 3E supports this theory as the VIR infected neurons had more neurite growth than either the non-infected neurons or the ATT infected neurons. Prehuad et al. were able to visualize morphological differences in cells infected with either VIR or ATT strains using immunohistochemistry (Figure 3D) [10]. In VIR infected cells, there are higher levels of proliferation and more neurite growth compared to ATT infected cells. This is indicated by the more intense green fluorescence in VIR infected cells and the more normal looking localization of the neuronal tubulin (Figure 3D). These results suggest that the G protein and more specifically, the PDZBS play an important role in RABV virulence.
After performing pull down assays using the two different G proteins as bait, it was found that the ATT G protein had less specific binding than the VIR G protein [10]. The VIR G protein bound only to microtubule associated serine-theronine kinases 1 and 2 (MAST1 and MAST2) while the ATT G protein also associated with non-receptor protein tyrosine phosphatase 4 (PTPN4) and other unrelated PDZ domain proteins. Prehaud et al. propose that the RABV G proteins of VIR and ATT are competing with the endogenous binding partners of MAST2 and PTPN4 and these interactions are causing the different survival phenotypes. MAST2 inhibition has been shown to induce neurite growth and it has been found that PTPN4 induces apoptosis [10]. Synthesizing all of the data, Prehaud et al. propose that the more nonspecific binding of the ATT G protein PDZBS to PTPN4 causes an infected cell to commit apoptosis and that this pathway has a more dominant effect than the inhibition of MAST2 which would explain the lack of neurite growth[10].
If this model were correct, it would demonstrate the balance that needs to be stuck between RABV and the host cell. To accomplish its goal of reaching the brain and salivary glands, RABV needs the host cells alive. This means hijacking very specific pathways within the cell that lead to a more favorable environment for the virus. The specificity of the G protein suggests that RABV walks a fine line by de-activating some signaling cascades while leaving others intact.
Neuroinflammation and the Blood Brain Barrier
The NS intrinsically limits the inflammation response following injury; however inflammation is still triggered in the NS by most infections. In contrast to most encephalitic viruses, RABV triggers a more limited inflammation response. In fact, the more pathogenic the strain is, the smaller the inflammatory response [11]. It is unclear how exactly RABV is able to limit the inflammatory response, but it has been suggested that the ability correlates to the differences between classical and non-classical strains. By comparing the amount of viral RNA and 18 cytokine mRNAs in twelve different brain regions of dogs infected with classical and non-classical rabies, Laothamatas et al. was able to determine key differences in the inflammatory response triggered [12]. The differences were found early on in infection, with non-classical RABV infected dogs having higher levels of both interleukin-1beta and interferon-gamma (INF-γ) and lower levels of viral RNA. Dogs infected with classical RABV had much higher levels of viral mRNA in brain tissue. Later in infection, there wasn’t much difference between the viral RNA and cytokine mRNA levels in dogs infected with the different strains [12]. The increased nueroinvasiveness of the classical strain probably correlates to the decreased immune response in comparison with the non-classical strain. Strength of the nueroinflammitory response might also correlate to the permeability of the blood brain barrier (BBB).
The permeability of the BBB in rabies infection is important as permeability relates to host cell survival. A more permeable membrane leads to an increased chance of host survival as it allows for passage of more immune cells into the NS. It has been shown that BBB permeability is increased in laboratory attenuated strains of RABV but until experiments carried out by Chai et al., the underlying mechanisms were a mystery [13].
Tight junction proteins (TJPs) are critical to maintaining the BBB, so Chai et al. examined the expression of three TJPs in mice infected with a wild type RABV strain, a lab attenuated strain, or a sham infection [13]. Immunohistochemistry and subsequent Western Blots of mouse brain tissue showed that the TJP expression in the wild type strain infected mice closely resembled that of the sham injected mice, while mice infected with the lab attenuated strain showed significantly lower expression levels. This suggested a correlation between the loss of TJPs in brains of mice infected with the attenuated RABV and the increased permeability of the BBB in these mice. However, this loss of TJ expression is not due directly to attenuated RABV infection as neither the attenuated nor the wild type strains are able to infect brain microvascular endothelial cells (BMECs) in vitro [13].
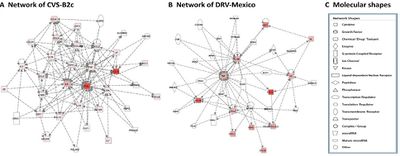
Chai et al. were only able to change the expression pattern of TJPs after exposing cultured BMECs to extracts taken from brains of mice infected with the attenuated RABV strain [13]. This suggested that it was a response triggered by the virus rather than the virus itself that caused the downregulation of TJPs. This lead to the use of a mouse cytokine/chemokine magnetic bead panel to determine if there were differences in the cytokine/chemokine levels in brains of mice infected with either the wild type or attenuated strain. The brains of mice infected with the attenuated strain had higher levels of cytokines/chemokines and a genetic network map was created for each strain (Figure 4) [13].
The network induced by attenuated strain (Fig4 A) contains 26 focus molecules while the wild type strain network (Fig 4B) only has 12. IFN-γ is at the center of the network, which corresponds to the findings of Laothamatas et al. and their non-classical strain induction of higher levels of INF-γ[12][13]. Upon further investigation of INF-gamma’s role in BBB permeability, Chai et al. found that silencing INF-γ causes a decrease in TJ and an increased permeability of the BBB suggesting that the attenuated strain interferes with normal INF-γ signaling [13].
This is another example of the balance RABV has to strike. The higher levels of INF-γ in attenuated strains could come from changes in protein binding like Prehaud et al. found in the PDZBS of the G protein [10]. Or it could be something completely different. Further investigation of this issue is important for understanding RABV and how to stop RABV infection.
Conclusion
RABV is has a two pronged strategy to in evading the immune system. First, RABV uses the host’s natural defense of the NS from excessive immune response to its advantage by making it extremely difficult for lymphocytes to do their job. RABV is able to create a neuroevasive environment in the peripheral nervous system and the spinal cord by upregulating the expression of surface proteins that inhibit T cell activity such as B7-H1 [6][7][8]. Once it reaches the brain RABV is able to avoid triggering an inflammatory response therefore keeping the lymphocytes out of the brain [13]. Second, RABV is able to promote neurite growth and prevent cell mediated apoptosis [10]. This allows virions to utilize the host’s nervous system as a transportation system to the brain.
By examining attenuated strains of the virus, we can learn more about how RABV interacts with host cells. This knowledge will lead to understanding exactly how RABV is able to move through the nervous system undetected and undeterred and how to tip the scales in favor of the host’s immune system. Rabies is still a major problem in quite a few countries and finding more affordable cures and preventative measures will go a long way towards fighting this disease.
References
[1] WHO Fact Sheet 99: Rabies. (2014, September 1). Retrieved November 10, 2014.
[11] Baloul, L., and Lafon, M. (2003). Apoptosis and rabies virus neuroinvasion. Biochimie 85(8):777–788.
Edited by Alexandra Gonzales, student of Joan Slonczewski for BIOL 375 Microbiology, 2014, Kenyon College.
