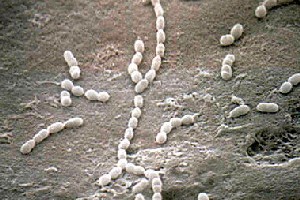
Streptococcus gordonii
A Microbial Biorealm page on the genus Streptococcus gordonii
Classification
Higher order taxa
Bacteria; Firmicutes; Lactobacillales; Streptococcaceae; Streptococcus
Species
|
NCBI: Taxonomy |
Streptococcus gordonii
Description and significance
Describe the appearance, habitat, etc. of the organism, and why it is important enough to have its genome sequenced. Describe how and where it was isolated. Include a picture or two (with sources) if you can find them.
.
Genome structure
Describe the size and content of the genome. How many chromosomes? Circular or linear? Other interesting features? What is known about its sequence? Does it have any plasmids? Are they important to the organism's lifestyle?
Cell structure and metabolism
Describe any interesting features and/or cell structures; how it gains energy; what important molecules it produces.
The human oral cavity provides a limited and varying source of nutrition for microbes inhabiting the oral micro flora (3). Oral streptococci, including S. gordonii, rely on sugars derived mainly from carbohydrates as an energy source. Fructose, a major component in the human diet, can be obtained via glucosyltransferases and from fructans via fructanases. Oral streptococci depend mainly upon the phosphotransferase system (PTS) to transport carbohydrates by means of phosphorylation and translocation through the membrane. The phosphoenolpyruvate-dependent PTS is the main pathway of transportation of sugars especially at low sugar concentrations (3).
The mammalian extracellular matrix is abundant in glycosaminoglycans (GAGs) consisting of recurring beta-linked dissaccharide units. When glycosaminoglycans are degraded, beta-linked disaccharides are released. S. gordonii ferments these beta-glucoside sugar substrates, including cellobiose, arbutin, salicin and esculin, to produce energy. In a recent study, beta-glucoside metabolism-encoding genes were expressed in Streptococcus gordonii colonization of saliva-coated hydroxyapatite (sHA) and impaired heart valves in rabbits (2). The beta-glucoside metabolism genes contained “a binding protein-dependent sugar transport and metabolism” and two phosphoenolpyruvate-dependent phosphotransferase systems (PTS). Several putative regulons contain these genes encoding for essential enzymes for metabolism. Bgl contains genes encoding subunits of a PTS enzyme II permease while bfr genes encode beta-glycosidase (BglF). Another regulon, ‘’esc,’’ enables the metabolism of beta-glucoside esculin and oligochitosaccharides by containing genes encoding for regulation (EscR), transport (EscP), and metabolism (EscA) of PTS (2).
Additional PTS operons have been identified such as fruK, encoding for enzymes that phosphorylate fructose-1-phosphate to fructose 1,6-bisphosphate and ‘’fruR,’’ encoding for catabolite reprossion. ‘’fruK’’ and ‘’fruI’’ are also thought to facilitate biofilm formation (3).
Ecology
Describe any interactions with other organisms (included eukaryotes), contributions to the environment, effect on environment, etc.
Dental plaque biofilm formation begins with pioneer organisms which attach to tooth surfaces in the human oral cavity. Streptococus gordonii is one of these pioneer organisms which initiate colonization and assist the further colonization of other organisms including Porphyromonas gingivalis, a periodontal pathogen.
In a recent study, S. gordonii was found to contain essential genes that facilitate the accrual of free floating P. gingivalis cells into the beginnings of a functioning biofilm. These genes were integral components in extracellular capsule biosynthesis, intercellular or intracellular signaling, biofilm architectural development and maintainance of adhesive proteins.
Initialy, Streptococcus gordonii initiates colonization through formation of a monospecies biofilm. S. gordonii cells at the surface of the tooth initiate a signal transduction pathway, known as BrfAB, which regulates adhesive activity. The S. gordonii monospecies biofilm then acts as a binding site for attachment of other more pathogenic organisms such as P. gingivalis by a process called coadhesion. Specifically, the long fimbriae (FimA) of P. gingivalis binds to glyceraldehydes-3-phosphate dehydrogenase (GAPDH) contained in the S. gordonii surface. The short fimbriae (Mfa) of P. gingivalis allows the cells to interact with the streptococcal SspA/B (antigen I/II) adhesions via an 80 amino acid binding epitope of SspA/B (BAR).
Human volunteers who have introduced P. gingivalis into their mouths have shown that P. gingivalis is found solely in areas of streptococcal rich plaque. Furthermore, biofilms between P. gingivalis and other streptococci, such as Streptococcus mutans and Streptococcus cistatus, are nonexistent. S. gordonii, therefore, may influence the constituents of oral biofilms by the specificity of adherence and signaling mechanisms. In in vitro studies, P. ginigivalis was also shown to coadhere with S. gordonii and this binding interaction promotes degradation of dentinal tubules by the otherwise non-dentin invasive P. gingivalis.
Pathology
Although S. gordonii initiates dental plaque and the colonization of other pathogenic bacteria on tooth surfaces, S. gordonii is not directly pathogenic in the oral cavity. On the other hand, once S. gordonii enters the blood stream via oral bleeding it can colonize damaged heart valves causing endocarditis in humans (4). Blood platelets, cell fragments that facilitate blood clotting, bind to fibrinogen on the damaged heart valves and endocardium, the heart’s inner lining, and form platelet-fibrin thrombi. This platelet-fibrin thrombi can become colonized by S. gordonii causing damage to the heart valves and dysfunction of the heart (4).
During bleeding of the oral cavity more than seven hundred bacterial species may enter the blood stream although of these seven hundred, the oral streptococci are the most common causes of endocarditis (6). S. sanguis, S. oralis, and S. gordonii are the top three enodcarditis causing pathogens. It is curious that oral streptococci are efficient in binding to blood platelets especially since the blood stream is not their natural habitat. Recent studies have addressed this phenomenon and concluded that oral streptococci have adapted specialized mechanisms to recognize and bind with sialic-acid containg structures in the mouth, their natural habitat, which also allows for efficient interaction with platelet sialoglycoprotein GPI-alpha, located on the platelet membrane. In S. gordonii, Hsa and GspB proteins facilitate adhesion with both sialylated salivary molecules like mucin, MG2, as well as platelet surface proteins, GPI-apha and GPIIb. Clearly, an evolutionary adaptation in one habitat has allowed S. gordonii and other oral streptococci to invade another habitat (4).
Bacterial endocarditis occurs in humans who most often have artificial heart valves, heart disorders, or hypertrophic cariomyopathy (5). Dental surgery, oral trauma, urologic or gynecologic surgery, skin infections and intravenous drug use will increase the chances of endocarditis. Some symptoms of bacterial endocarditis include “fatigue, loss of appetite, night sweats, chills, headaches, joint discomfort, and tiny pinpoint-sized hemorrhages on the chest and back, fingers, or toes.” Treatment consists of intravenous antibiotic therapy and sometimes oral antibiotics for several weeks (5).
Application to Biotechnology
Does this organism produce any useful compounds or enzymes? What are they and how are they used?
Current Research
Enter summaries of the most recent research here--at least three required
References
(2) Kilic, A., Tao, L., Zhang, Y., Lei, Y., Khammanivog, A., Herzberg, M. "Involvement of Streptococcus gordonii Beta-Glucoside Metabolism Systems in Adhesion, Biofilm Formation, and In Vivo Gene Expression". Journal of Bacteriology. 2004. Volume 186. p. 4246-4253.
(3) Loo, C., Mitrakul, K., Voss, I., Hughes, C., Ganeshkumar, N. "Involvement of an Inductible Fructose Phosphotransferase Operon in Streptococcus gordonii Biofilm Formation". Journal of Bacteriology. 2003. Volume 185. p. 6241-6254.
Edited by Tanya Budiarto student of Rachel Larsen