The pathogenesis of Bacillus anthracis
Overview

By [Tony Amolo]
Anthrax is an infectious disease caused by the bacteria Bacillus anthracis. Bacillus anthracis is a microorganism from the family Bacillaceae. Unlike other bacillus microorganisms which are harmless saprophytes, bacillus anthracis is an obligate bacillus pathogen in mostly vertebrates. Based on its physical characteristics, bacillus anthracis can be categorized with other microorganisms such as Bacillus cereus, Bacillus thuringiensis and Bacillus mycoides. This classification holds because it is difficult to characterize these organisms based on their 16s rRNA sequences (10). Organisms from the bacillus genus are thermophilic, psychrophilic, acidophilic, alkaliphilic, halotolerant, and halophilic. They have the ability to grow in severe conditions which other microorganisms cannot withstand (4).
Anthrax is as old as man, it was given its name by a Greek physician named Hippocrates because of the black sore it causes on the skin of human and animals(1). It generally affects warm blooded animals including humans. Aloys Pollender, a German physician who was acknowledged for identifying the disease described bacillus anthracis as “chyllus corpuscles” after analyzing the abdomen of infected cows that had died of anthrax (2). Anthrax was broadly studied in the 1870s by Robert Koch and Louis Pasteur. Koch used suspended drop culture methods to trace the complete life cycle of the bacteria and found that the spores formed could remain viable for long period of adverse environments (3).Koch’s studies on Bacillus Anthracis helped him come up with the germ theory of disease.
.
Cell Structure and Metabolism
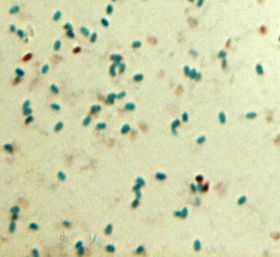
Bacillus anthracis is a gram positive, endospore forming bacteria. It is capsulated, immobile and rod shaped. Bacillus anthracis has the ability to make ATP in the presence or absence of oxygen. Bacillus anthracis cannot be seen unless with a microscope. It is 5-6 micrometer in length by 1-1.5micrometer wide and looks like bamboo canes in tissue (13). Despite its small size, the diverse abilities of many species of its genus allows them to survive in different environments (4). They have the ability to form chains, colonies and biofilms.
Habitat and Ecology
Bacillus anthracis is a soil borne bacteria. It lives best in black steppe soils with lots of calcium and at pH levels between (7-9). Endemic anthrax areas have been associated with warmer temperatures, higher soil moisture content and topography (15).
Spore Formation, Anatomy and Germination
Bacillus anthracis forms one endospore per cell. Its spores form when its non reproductive cells are in need of specific nutrients (Figure 2). The spores are oval in shape and sporulation occurs within 48 hours. Bacillus anthracis requires oxygen to sporulate. Spores can tolerate heat, cold, dehydration, radiation and even antibacterials (8). The formation of spore commences when cells septate asymmetrically to create a forespore and a mother cell. After septation, the mother cell swallows the forespore and covers it with different layers. The spore is made up of several layers. These layers are the coat, the exosporium and the cortex. The innermost layer is the core. It contains proteins which holds the chromosome. Half of the spore is composed of the spore coat. The flexibility of the spore coat enable the spore to hold the core during germination. It protects the spore from harmful chemicals and aids germination. The cortex containing peptidoglycan protects the spore from radiation, heat and makes the core dry. The exosporium is the outermost layer of the spore. It is a protein rich, balloon-like, loose fitting structure covering a spore(8). The exosporium has been studied to understand the use of anthrax as a weapon. The disintegration of the mother cell to produce the spore indicates the completion of spore formation. The mature spores have a structured arrangement that enables them withstand and endure physical damage and severe environmental conditions. Outside a host, the mature spores of bacillus anthracis are inactive. Upon entry into a host, they have the ability to germinate and become non reproductive cells that can easily replicate all around the host's internal organs.The availability of host’s environment with sufficient nutrients causes germination to occur (17). Non reproductive cells transform back to spores whenever the host dies. Germination and growth of spores in the host cells are essential for the release of its virulence factors.
Pathogenesis and Virulence factors
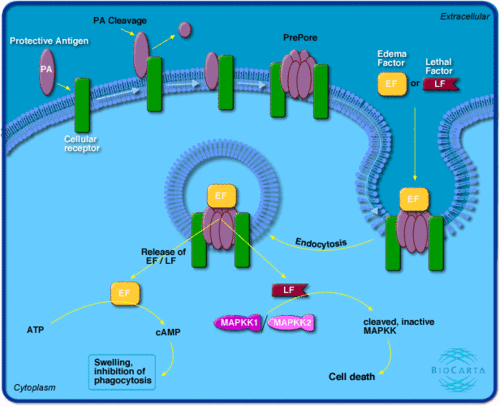
Bacillus anthracis depends on two toxic factors from two plasmids:
the pX01, 182kb,this plasmid encodes the genes for the lethal factor (LF), the edema factor (EF) and the protective antigen (PA),
pX02, 96kb, this plasmid encodes the genes for the biosynthesis of the capsule. The pathogenic effect of bacillus anthracis is through its capsule and through the production of toxin(EF, LF and PA)(13)(Figure 3).The lethal toxin(LT, the combination of PA and LF) and edema toxin (ET, the combination of PA and EF) are enough to produce and cause the anthrax infection.(7) Of the three factors, the PA plays an important role in the toxic action of Bacillus anthracis. Protective antigen (735 amino acids) plays an important role in anthrax intoxication by allowing the attachment and entry of the lethal factor and Edema factor into the cytosol. It contains regions involved in binding to the cell receptor, binding LF and EF, membrane insertion, and translocation of the anthrax toxin. Protective antigen is a major immunogen present in anthrax vaccines(11). The edema factor(89kDa) is a calcium and calmodulin-dependent adenylate cyclase that causes an increase in cytoplasmic cAMP. This leads to an imbalance of water homeostasis in the cell. The edema toxin disrupts the cytokine response of monocytes which may increase the chance of the host being infected by the disease(11). The lethal factor is a Zn2+ dependent metalloprotease that attaches major pathways to surface receptors for the transcription of certain genes within the nucleus(12) while the capsule inhibits the phagocytosis of bacillus anthracis.
They study of Anthrax toxins has provided a mechanism of trans-membrane translocation of proteins and the discovery of plasmids pXO1 and pXO2 which allowed the study of toxic factors at a genetic level(5).
Transmission and Pathology
Bacillus anthracis is not an invasive organism. The ways of transmission of the anthrax disease are through wounds, mucous membranes of the mouth, pharynx, gastrointestinal tract, the digestive tract after ingestion of spore contaminated food or water, skin abrasions, sore, lesions caused by biting flies and the inhalation of dust containing spores. After transmission through one of these route, the spores of Bacillus anthracis are carried from the site of entry to the draining lymph nodes where they begin to multiply rapidly and the produce spores which germinate to produce the toxic factors (13). The pathogenicity of Bacillus anthracis depends on the sensitivity of the host, the infectious dose(amount of toxin produced), the quality of the capsular coat and the route of penetration (13).
Symptoms
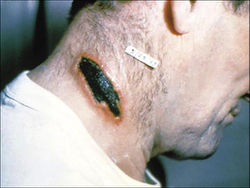
Anthrax in Humans
Cutaneous anthrax
Cutaneous anthrax is also called malignant pustule. It is usually localized around the face, arms, hands, and neck. It occurs when a contaminated cut creates a path of entrance for the organism. A primary lesion is formed with a few days and a ring of vesicles develops around the central papule. This dries up to form a black lesion (Figure 4). The lesion develops for 12-14 days leaving a shallow ulcer that heals in 2-3 weeks. Patients show symptoms of headaches, fever of up to 102 degree Fahrenheit, discomfort and even death.
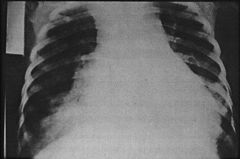
Pulmonary(inhalation) anthrax
Also known as woolsorter’s disease, pulmonary anthrax is caused by inhaling the anthrax spores. Spores are phagocytosed by alveolar macrophages and carried to the lymph nodes where they germinate and multiply (Figure 5). Fatal bacteraemia and toxaemia then occurs. (10) During the initial stage, the patient experiences mild fever, malaise, fatigue and cough. The second stage include symptoms like acute dyspnea, cyanosis and profuse perspiration.
Gastrointestinal anthrax
Also known as splenic fever, gastrointestinal anthrax is extremely rare and occurs mainly in Africa, the Middle East and central and Southern Asia. It is caused by eating an insufficiently cooked meat contaminated with spores. Symptoms include diarrhea, ulcer, liver disease and fever. Another rare form of anthrax in man is anthrax meningitis. (6)
Vaccines and Treatment
The first bacterial disease that a preventive treatment (prophylaxis) was developed for was the Anthrax disease(11). Prophylaxis helped in controlling anthrax in animals and preventing the spread of the infection.
Several vaccines have been produced for the anthrax disease since Louis Pasteur first produced the attenuated anthrax vaccine in 1881 (2). The vaccines used to fight anthrax are composed of spores from weakened strains of Bacillus anthracis. They are classified into two categories namely;
Live attenuated vaccines, capsulated and atoxigenic cap
Live attenuated spore vaccines, not capsulated and toxigenic cap. For example, Sterne and sexually transmitted infection (STI) vaccines. (13)
Other vaccines include non-living vaccines, In vitro protective antigen, Boor and Tresselt vaccine, production in non-proteinaceous media, UK vaccine, American vaccines(Aerobic antigen and Anaerobic antigen) and Russian antigen (6). Special therapy can also be provided to treat anthrax if it is applied immediately to the infected animal or human. Aside from vaccines, antitoxin and antibiotics have been used to treat the disease. Penicillin, doxycycline and ciprofloxacin have been used for treatment of susceptible strains of anthrax (14). Several methods have been adopted to create an improved human vaccine. Recombinant DNA methodology is being used to create live vaccine strains of Bacillus anthracis. The goal is to create a new vaccine that is safe, non reactogenic, efficacious against all disease and requires a little number of inoculations to achieve maximum lasting immunity (11). The challenging and difficult aspect of evaluating the efficacy of anthrax vaccine is making an assessment in humans because it is not safe to be tested on humans. Animals can be used as a model but the process can be dangerous.
Application to Bioterrorism
Out of many pathogenic bacteria, Bacillus anthracis is one that can be used for bioterrorism. It makes a good model weapon for bioterrorism because it spores can be produced in the lab,last for a long time in the environment and can be found easily in nature. Also because of its small size, it can be placed in food and letters like in 2001 when powdered anthrax was mailed to the U.S postal office. Twenty-two cases of anthrax infections were confirmed. Half of these cases involved cutaneous anthrax and no death resulted. The remaining eleven were identified as inhalational anthrax and produced five deaths. A global awareness should be created to reject the development of such weapons and provide means of developing a vaccine for this deadly disease.
References
1] Annabel Guicharda, Victor Nizetb, c, Ethan Biera "New insights into the biological effects of anthrax toxins: linking cellular to organismal responses." 2012.
2] Joseph A Witkowski,Lawrence Charles Parish "The story of anthrax from antiquity to the present: a biological weapon of nature and humans."2002.
3] George Sternbach "The history of anthrax."2003.
4] Peter C. B. Turnbull "Bacillus."1996.
5] Maxime Schwartz "Dr. Jekyll and Mr. Hyde: A short history of anthrax."2009.
6] Peter Hambleton, J.Anthony Carman, Jack Melling "Anthrax: the disease in relation to vaccines."1984.
7] Mahtab Moayeri, Stephen H Leppla "The roles of anthrax toxin in pathogenesis."2004.
9] W. Beyer, P.C.B. Turnbull. "Anthrax in animals."2009.
10] Les Bailliea, , Timothy D Read. "Bacillus anthracis, a bug with attitude!."2001.
11] Stephen F Little, Bruce E Ivins. "Molecular pathogenesis of Bacillus anthracis infection."1999.
14] Martin Hugh-Jonesa, Jason Blackburn. "The ecology of Bacillus anthracis."2009.
16] [1]
17] Adam Driks. "The Bacillus anthracis spore."2009.
Edited by student of Joan Slonczewski for BIOL 238 Microbiology, 2009, Kenyon College.
