Toxoplasmosis: Difference between revisions
| Line 69: | Line 69: | ||
<br />3 [http://www.waterbornepathogens.org/index.php?option=com_content&view=article&id=65&Itemid=73 Sarah Staggs and Eric Villegas. Waterborne Pathogens: Toxoplasma. Last Updated: 04 April 2012] | <br />3 [http://www.waterbornepathogens.org/index.php?option=com_content&view=article&id=65&Itemid=73 Sarah Staggs and Eric Villegas. Waterborne Pathogens: Toxoplasma. Last Updated: 04 April 2012] | ||
<br />4 [http://www.cfsph.iastate.edu/Factsheets/pdfs/toxoplasmosis.pdf Iowa State University. The Center for Food Security and Public Health. Toxoplasmosis: Toxoplasma Infection. Last Updated: May 2005] | <br />4 [http://www.cfsph.iastate.edu/Factsheets/pdfs/toxoplasmosis.pdf Iowa State University. The Center for Food Security and Public Health. Toxoplasmosis: Toxoplasma Infection. Last Updated: May 2005] | ||
<br />5 [http://www.mayoclinic.com/health/toxoplasmosis/DS00510/DSECTION=treatments-and-drugs The Mayo Clinic Staff. Toxoplasmosis: Treatment and Drugs. Last Updated: June 24, 2011] | |||
Created by Magdalene C. Shaughnessy, student of Tyrrell Conway at the University of Oklahoma | Created by Magdalene C. Shaughnessy, student of Tyrrell Conway at the University of Oklahoma | ||
Revision as of 17:17, 22 July 2013

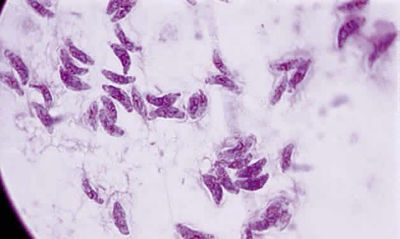
From: http://www.oculist.net/downaton502/prof/ebook/duanes/pages/v4/v4c046.html

From: http://www.economist.com/node/16271339
Description/Etiology/Taxonomy
Toxoplasma gondii is an obligate, intracellular parasitic protozoan that infects most species of warm blooded animals, including humans, and is the causative agent of the disease Toxoplasmosis. While T. gondii may infect humans to asexually reproduce and cause disease, the only host in which the protozoa may complete its life cycle and sexually reproduce are family Felidae, more commonly referred to as domestic cats and their relatives. [1]
Taxonomy of Toxoplasma gondii
Domain: Eukaryota
Kingdom: Chromalveolata
Superphylum: Alveolata
Phylum: Apicomplexa
Class: Conoidasida
Subclass: Coccidiasina
Order: Eucoccidiorida
Family: Sarcocystidae
Subfamily: Toxoplasmatinae
Genus: Toxoplasma
Species: Toxoplasma gondii
Pathogenesis
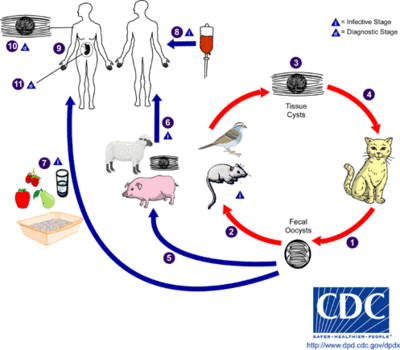
Transmission
Lifecycle
The only hosts in which Toxoplasma gondii can mature and reproduce are members of the family Felidae. Infected domestic cats (and those related to them) will shed large numbers of unsporulated oocysts in their feces for approximately one to two weeks. Oocysts released into the environment take from one to five days to form spores and become capable of causing infection. Intermediate hosts, commonly birds and rodents as they are typical prey of felines, may then become infected by consuming materials contaminated with T. gondii spores. After ingestion, oocysts develop into tachyzoites which localize in neural and muscle tissues to develop into cyst bradyzoites. Members of the family Felidae become infected after consuming intermediate hosts that have these cysts in their tissues. Additionally, other animals may become infected with cysts after ingesting T. gondii spores from the environment. [1]
Infecting humans
Humans may become infected with Toxoplasma gondii by a variety of routes. The most common methods of infection include: consuming undercooked meat of animals that had tissue cysts, consuming food or water contaminated with infected cat feces, consuming food or water contaminated by infected environmental samples (e.g. soil, cat litter), receiving a blood transfusion or organ transplant from individuals harboring tissue cysts, and infection of a fetus transplacentally from the mother. Unlike its lifecycle in felines and intermediate hosts, T. gondii commonly forms cysts in the skeletal muscle, brain, eyes, and myocardium of the human host. Additionally, rather than being shed in feces like the feline host, the cysts in a human host may remain for the entire life of the human host. [1]
Colonization
Infectious dose
There is no known specific infectious dose, or approximate number, of Toxoplasma gondii organisms required to cause disease, however it has been suggested that the number is very low. [2] However, there are three stages of the T. gondii lifecycle in which it is infectious. The first infectious phase of the T. gondii lifecycle is during the oocyst stage; T. gondii oocysts may be found in soil or water and can survive in the environment for several months. The second infectious phase is the tachysoite stage, a phase of rapid replication in the tissues of the host; this is the stage responsible for the onset of acute toxoplasmosis. Finally, the third infectious stage of the T.gondii lifecycle is the bradyzoite stage in which the parasite slowly replicates in the muscle and brain tissue of the infected host. [3]
Incubation period
The incubation period, or the time between exposure to the organism and the onset of symptoms, of Toxoplasma gondii in a human host is 10 to 23 days after consuming contaminated food or water, and 5 to 20 days after exposure to infected cat feces. [4]
Virulence factors
Clinical features
Epidemiology
It is estimated that 22.5% of the United States population over age 12 is infected with Toxoplasma gondii. In other countries, the infection rates are close to 95% of infected persons within a population. Toxoplamsa gondii infects a greater percentage of people in areas of the world that lower in altitude and have hot, moist environments. [1]
Symptoms
In healthy Individuals
Healthy individuals who become infected with Toxoplasma gondii are often asymptomatic. Occasionally, a non-immunosuppressed individual will develop flu like symptoms for a few weeks that eventually fade. [1]
In immunocompromised individuals
Immunocompromised individuals, for example individuals who have HIV/AIDS, suffer a wide range of symptoms from Toxoplasma gondii infection including inflammation of the lung tissue, myocarditis, and acute inflammation of the brain. [2]
Pregnancy-associated infection
If a woman becomes infected with Toxoplasma gondii while pregnant, especially in the early stages of pregnancy, the parasite may be congenitally transmitted to the unborn child. Results of a congenital infection often result in a miscarriage or still birth. Some children may be born asymptomatically and develop symptoms such as vision loss, mental disability, and seizures later in life. [1]
Morbidity/mortality
Toxoplasmosis infection is asymptomatic is 80-90% of infected healthy individuals and immunity typically remains consistent throughout the life of the host unless they become immunocompromised. However, in immunosuppressed patients, the mortality rate from infection is very high. For example, Toxoplasma-related encephalitis occurs in 25% of AIDS patients and was 84% fatal in this particularly immunosuppressed group. Additionally, the earlier on in a pregnancy that a fetus becomes congenitally infected, the higher the likelihood is that they would develop severe disease. [4]
Diagnosis
Diagnosis of Toxoplasmosis is generally achieved via serology, or the examination of plasma or other bodily fluids to determine whether the body has produced antibodies in response to a specific antigen. Additionally, Toxoplasmosis may be diagnosed via the identification of T.gondii cysts in a tissue sample taken from a suspected infected individual. Diagnosis of Toxoplasmosis infection before birth may be determined by confirming the presence of T. gondii DNA in amniotic fluid. [1]
Treatment
In healthy Individuals
Since 80-90% of Toxoplasmosis infections in healthy individuals are asymptomatic, the majority of infections go unnoticed and do not require treatment. When the rare occasion arises that an otherwise healthy individual presents with symptoms of acute Toxoplasmosis, a combination of pyrimethamine, an anti-malaria medication, and sulfadiazine, an antibiotic, may be prescribed. Folic acid is often prescribed along with pyrimethamine to avoid potentially harmful side effects of this drug. [5]
In immunocompromised individuals
The treatment for an immunocompromised individual (i.e. one with HIV/AIDS) is also a combination of pyrimethamine and sulfadiazine. In some cases clindamycin may be prescribed as an alternative to sulfadiazine. Unlike immunocompetent patients, immunosuppressed patients may have to remain on these medications for life in order to keep the infection at bay. [5]
Pregnancy-associated infection
Pregnant women infected with toxoplasmosis whose fetus remain unaffected by Toxoplasmosis may be given the antibiotic spiramycin. This drug reduced the likelihood that the infant will become infected and suffer severe disease symptoms later on in life. Pyrimethamine and sulfadiazine are typically not prescribed to pregnant women whose babies are already infected as the drug will not repair any damage that has already been done, and the drugs come with serious risk of side effects for the unborn child. [5]
Prevention
Host Immune Response
References
1 Centers for Disease Control (CDC). General Information Toxoplasmosis. Page last updated: January 10, 2013
2 Public Health Agency of Canada. Toxoplasma gondii - Material Safety Data Sheets (MSDS). Date Modified: 2011-02-18
3 Sarah Staggs and Eric Villegas. Waterborne Pathogens: Toxoplasma. Last Updated: 04 April 2012
4 Iowa State University. The Center for Food Security and Public Health. Toxoplasmosis: Toxoplasma Infection. Last Updated: May 2005
5 The Mayo Clinic Staff. Toxoplasmosis: Treatment and Drugs. Last Updated: June 24, 2011
Created by Magdalene C. Shaughnessy, student of Tyrrell Conway at the University of Oklahoma
