Mycobacterium
A Microbial Biorealm page on the genus Mycobacterium
Classification
Higher order taxa:
Bacteria; Actinobacteria; Actinobacteria (class); Actinobacteridae; Actinomycetales; Corynebacterineae; Mycobacteriaceae; Mycobacterium; Mycobacterium tuberculosis complex
Species:
Mycobacterium tuberculosis, M. leprae
|
NCBI: Taxonomy Genome: M. leprae M.tuberculosis |
Description and Significance
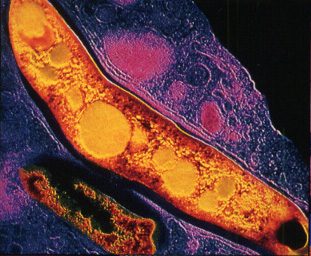
Both leprosy and tuberculosis, caused by Mycobacterium leprae and Mycobacterium tuberculosis respectively, have seriously plagued mankind for centuries. With the emergence of antibiotic resistant strains of tuberculosis, research into mycobacteria has become all the more important in combatting these modern mutants of ancient pathogens.
Genome Structure
Both the genomes of Mycobacterium tuberculosis and Mycobacterium leprae have been sequenced with hopes of gaining further understanding of how to defeat the infamously successful pathogens. The genome of M. tuberculosis is 4,411,522 base pairs long with 3,924 predicted protein-coding sequences, and a relatively high G+C content of 65.6%. At 4.4 Mbp, M. tuberculosis is one of the largest known bacterial genomes, coming in just short of E. coli, and a distant third to Streptomyces coelicolor.
The genome of Mycobacterium leprae is 3,268,203 base pairs long, with only 1,604 predicted protein-coding regions, and a G+C content of about 57.8%. Only 49.5% of the M. leprae genome contains open reading frames (protein-coding regions), the rest of the genome is comprised of pseudogenes, which are inactive reading frames with recognizable and functional counterparts in M. tuberculosis (27%), and regions that do not appear to be coding at all, and may be gene remnants mutated beyond recognition (23.5%). Of the genome of M. tuberculosis, 90.8% of the genome contains protein-coding sequences with only 6 pseudogenes, compared to the 1,116 pseudogenes on the M. leprae genome.
Operating on the assumption that M. leprae was once approximately the size of other mycobacteria, it has significantly downsized and degraded to its current state. If all the genes on the M. leprae genome were active, it would have about 3,000 open reading frames, compared to the 4,000 proteins of M. tuberculosis. Total, over its evolutionary history, M. leprae has lost more than 2,000 genes.
Cell Structure and Metabolism
Mycobacteria are rod-shaped, Gram-positive aerobes, or facultative anaerobes. As deduced from its genome, M. tuberculosis has the potential to manufacture all of the machinery necessary to synthesize all of its essential vitamins, amino acids, and enzyme co-factors. On the other hand, the inability to culture M. leprae, suggests that it has lost many of its metabolic capabilities, and is now an obligate parasite, dependent on its host for most of its nutritional needs. This goes in accordance with its severely degenerated genome. M. tuberculosis has an unusual cell wall, with an additional layer beyond the peptodiglycan layer, which is rich in unusual lipids, glycolipids, and polysaccharides.
Ecology
It is thought that the more well-known infectious agents such as M. tuberculosis and M. leprae are evolved from a soil bacterium. More specifically, M. tuberculosis arose from a soil bacterium that evolved to infect cows, and then made the jump to humans about the time of animal domestication about 10,000 years ago. M. tuberculosis and M. leprae both grow remarkably slow for bacteria. M. tuberculosis doubles its population every 18-24 hours, while M. leprae doubles its population about every 14 days. This extremely long generation time probably contributes to the chronic nature of both diseases.
Pathology
Both leprosy and tuberculosis, caused by M. leprae and M. tuberculosis respectively, are considered chronic pathogens, causing diseases that takes months, sometimes years, to develop, and, without treatment, eventually result in a slow and excruciatingly painful death. Two of the oldest recognized pathogens, tuberculosis and leprosy have been plaguing mankind since the first stages of domestication some 10,000 years ago. Most mycobacteria do not cause disease, so M. tuberculosis and M. leprae are hardly typical of the genus, and are consequently called 'wayward sons of honorable parents.' In recent years, with the ushering in of the antibiotic age, when penicillin is used to treat everything, new, drug-resistant forms of these pathogens have begun to emerge allowing both diseases to become serious threats to humanity once again. In 1993 with rates of reported cases of tuberculosis on the rise, the World Health Organization declared it a global emergency and began to make efforts to heighten public awareness. In addition to an increase in people contracting tuberculosis, it has formed a deadly partnership with the AIDS virus. The two diseases feed off of each other. With the depleted immune system caused by AIDS comes increased susceptibility to tuberculosis, which in turn accelerates the progress of AIDS.
Tuberculosis sets up camp in the lungs of its host, where it, for the most part, coexists with its host while lazily following its daily division routine, yet causing no outward symptoms, but rather just accumulating numbers in order to launch its assault on its unsuspecting host. Macrophages that normally ingest pathogens in order to destroy them, are made into a cozy home by the tubercle bacillus. Tuberculosis is transmitted from person to person through the air, and requires a six to twelve month regimen of at least two drugs to rid its host of the infection. Drug-resistant strains of the pathogen are mainly the result of patients not following directions in the taking of their medication, and thus do not kill off the disease entirely.
Almost a third of the world's population is infected with tuberculosis without knowing it. Some of these people may develop symptoms, but most will not. But for those who do treatment is generally available, unless they live in a "resource poor" setting. Currently there is a strain of tuberculosis called mutlidrug-resistant tuberculosis, or MDR-TB, which doctors in those countries will not treat. This is causing a problem, not only because the lack of treatment is spreading the disease, but because doctors can not afford to help these people with different treatment methods.
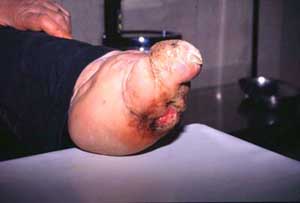
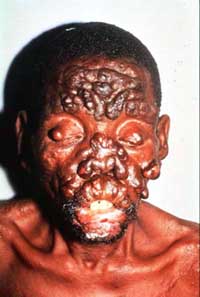
Leprosy, popularly thought to be a disease of the past, has over 690,000 new cases reported annually, but the mode of transmission still remains a mystery. The infection is very slow to develop, taking anywhere from six months to ten years. Leprosy is a neurological disease, that mainly accumulates in the extremities, and inhabits macrophages through which it infects the Schwann cells of the peripheral nervous system. The lack of myelin produced by the infected Schwann cells leads to nerve damage, and sensory loss. There are two forms of leprosy, tuberculin and lepromatous. Lepromatous leprosy is the more contagious form, in which the body is unable to mount a resistance, and the bacterium freely multiplies in the skin, causing nodules to appear all over the body and face. It also infects the mucous membranes of the nose and throat, creating a rather disturbing physique. Tuberculin leprosy causes an immune defense in which the body's cells crowd around the invading organisms in the deep skin layers, which causes hair follicles, sweat glands, and nerve endings at the site to be destroyed. The skin then becomes dry and discolored and loses feeling. This most often affects the fingers and toes which are now fragile and injury prone, and often become mutilated and fall off. It is also the seventh most common cause of blindness. Over 250,000 people are blind today because of a leprosy related eye problem. The leprosy bacterium attacks facial nerves and destroys the ability to blink. This leaves the eyes susceptible to infection which ultimately leads to blindness.
Luckily for the people disfigured by leprosy, with treatment this disfigurement can be almost entirely reversed.. Obviouslly they will not be able to grow new fingers, but the nodules that disfigure the body will disapear entirely.
References
Cole, S. T. et al. 2001. Massive gene decay in the leprosy bacillus. Nature, 409: 1007-1011.
Nature: Honey I shrunk the Genome
New York State Department of Health: Disease Carriers - Bacteria: Mycobacterium tuberculosis
Storrs, Eleanor E. Pandoras Box: Leprosy through the ages
The Leprosy Mission. What Leprosy does to the face and eyes.
Disease University of Cape Town: The Mycobacteria
Washington State University: Leprosy
Young, Douglas B. 1998. Blueprint for the white plague. Nature, 393: 515-516.
Parish and Brown 2009. Mycobacterium: Genomics and Molecular Biology. ISBN: 978-1-904455-40-0
