Vancomycin-resistant Enterococcus
Introduction
By Evan Baum
Enterococci are a group of bacteria that are coccoid or ovoid, gram positive bacteria that can live within the digestive tract of humans. There, the aid in the digestion of food, but cause infections in other places of the body. Enterococci are very resilient organisms, the can be found not only in intestinal tract but in soil, water, and food. They are able to live in temperatures ranging from 10-45 C and pH ranges from 4.8 to 9.6.
Vancomycin-resistant Entercoccus (VRE) (figure 1) is a bacterial strain of Enterococcus that has acquired resistance to the antibiotic vancomycin through the uptake of a plasmid that has the resistance. VRE can be resistant to not just vancomycin, it can be resistant to other antibiotics commonly used for Enterococcus infections such as aminoglycosides, and ampicillin . VRE is a major concern to hospitals. Healthcare workers can carry the bacteria and pass it along to patients. VRE is most associated with nosocomial infections, making up about 30% of all enterococcus infections in hospitals. Healthy people can bring VRE into the hospital where it can then infect patients. This bacteria is very dangerous towards immunocompromised individuals. With VRE's aptitude for passing on it's genes to other bacteria, this strain is very capable of transferring it's resistance to lethal infections such as MRSA.
Vancomycin Resistance
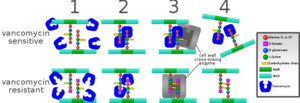
Vancomycin resistant Enterococcus was isolated in Europe in the late 1980s. However the use of Vancomycin began clinical use in the 1950s but was not wide spread until 1970s. Vancomycin works by inhibiting cell wall formation in gram positive bacteria and by this mechanism. Between each cell wall is a chain of amino acids that a cross linking enzyme recognizes and connects the carbohydrate chains. Vancomycin recognizes the two D alanine at the top of each chain and binds to them. The cross-linking enzyme can then not work properly and the cell wall would not from. For resistant bacteria, instead of have two D-alanine the last D-alanine has been replaced with D-lactate. This does not allow for vancomycin to bind properly and lets the cross-linking enzyme to properly form the cross links (figure 2).
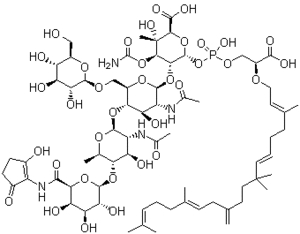
There are three types of clinically studied vancomycin resistant genes, vanA, vanB, and vanC. The highest resistance to vancomycin is vanA and continues decreasing with vanB then vanC. While vanB is still highly resistant to vancoymcin it is highly susceptible to teicoplanin. The last operon, vanC, has very low resistance to vancomycin and teicoplanin but this property is not transferable to other species. Teicoplanin like vancomycin, is a glycopeptide antibiotic. It attacks the glycopeptides and binds to them to inhibit the formation of cell membranes in gram-positive bacteria. It has a similar structure to vancomycin but does have some changes such as a long hydrocarbon chain that varies in length. This tail is said to be what gives this antibiotic strength. Vancomycin resistance is transferred through a plasmid from an already resistant bacteria to a sensitive bacteria (figure 3). Due to enterococcus capability of easily transferring DNA to other bacteria, this can prove troublesome for hospitals and health care centers. A major concern is MRSA acquiring vancomycin resistance. MRSA is a very tough infection to begin with. Patients with this infection may need hospitalization and kidney dialysis if the infection overwhelms the patients immune system. The best way yet, is to give intravenously, two antibiotics. If MRSA becomes vancomycin resistant, it will become that much harder to eliminate from patients. There have been studies to find out if there could be a way to hinder the genetic transfer of these operons. Flavophospholipol (FPL) (figure 4) is an antibiotic obtained from streptomyces, normally used in feed for cattle and pigs to promote growth. This antibiotic has been shown to reduce the transferring frequency by 70 fold (Riedl 2000). The mechanism of how this antibiotic does this is not know but there are some theories. One common explanation could be that there is some interaction of the peptidoglycan that is used in the bridging between two bacterial cells when there is transference of a gene (Riedl 2000). FPL is normally used against gram-positive bacteria and does work like vancomycin in disrupting membrane formation of the cell. However, vancomycin does not also have the effect of significantly decreasing gene transference. If there is use of FPL then there may be a way to hopefully reduce the occurrence of vancomycin resistance in MRSA.
Infection and Contamination in Hospitals
Hospitals are a breeding place for VRE. Nosocomial infections are very common in surgeries and is surprisingly is one of the top three pathogens isolated from patient's blood. VRE can cause peritonitis, urinary tract infections and endocarditis, bacteremia, meningitis, and can infect a number of medical devices. VRE is easily passed on from person to person or from contaminated services and medical equipment. VRE can exist in the human body without causing an infection however, this is called colonization. Colonized patients are not generally treated. Due to the massive flora in the digestive tract, the antibiotics used to kill the colonized VRE, will inadvertently kill off the beneficial bacteria. If the bacteria does enter the blood stream from the digestive tract or some how is introduced through a wound, then a person is considered infected with VRE. Symptoms of infection in the blood include fever, fast heart rate and the feeling of sickness. Urinary tract infections from VRE, symptoms include burning sensation while urinating, back pain, and fever. If there is suspect for a VRE infection then there may be blood or spinal fluid samples and cultured to determine infection. Urine and sputum can also be taken and cultured if the patient is experiencing UTI symptoms or pneumonia, these samples however, do not indicate specifically if the patient is colonized with VRE or is infected. A doctor will ask questions about the symptoms and also a physical exam to determine if signs are present for the infection.
There are improvements as to what visitors and nurses wear when they are in the presence of ICU patients. There have always been masks but there has been research to bring cap and gown when visitors come to the ICU. This is to prevent the spread of germs such as VRE from coming in contact with patients whose immune systems are already compromised. In the event of a patient becoming infected with VRE there are steps that hospitals are beginning to take in order to minimize the exposure and mobility the virus has with other people and medical instruments. People who are constantly in contact with the patient like nurses and doctors have sets of gowns, masks, caps and equipment so they do not overlap with patients who are not infected with the bacteria. A stool sample should be taken to see if there is colonization of VRE in the patent. After there is contact with an infected patient, the clothes should be taken off before exiting and immediately wash hands with antiseptic soap. Hand washing with antiseptic soap is a major part of preventing the spread of VRE (figure 6). The most common way patients become infected with the bacteria is through touching a contaminated surface. This can be greatly diminished with hand washing. Before seeing patients, especially ones in ICU and ones with compromised immune systems, health care workers and visitors should wash hands before and after to greatly reduce the impact of bacteria. After a carrier or infected patients is removed form the hospital room, there could still be residual fecal particles that could carry VRE. Possibly, some surface has been contaminated and not cleaned properly. This would lead to another patient being infected and the cycle starting over again.
Prevention and Treatment
As stated above there is a great stance for hand washing to prevent the spread of VRE. This is especially useful and a simple thing to help prevent further infections. Indirectly, this also helps to lessen the resistance gene from becoming more evolved towards vancomycin. The use of clean gowns, caps, and medical equipment also reduces the likelihood of infection, with the presence of sterilization there has been a decrease in the medical equipment infections. A major part of what can prevent VRE is hand washing and cleanliness of the rooms where people are staying. Washing hands for at least 30 seconds and getting under the nails can greatly prevent people getting VRE and transferring VRE to others. Cleaning a room should take precautions because VRE can contaminate multiple types of surfaces. However, the bacteria does not have a different life span on different surfaces. In fact there is very little variation between surfaces. What does impact the life span is the traffic the surface gets. High traffic areas such as handrails and countertops, will have a greater contamination period than something will less traffic. This is why hand washing is very important before and after visitors and hospital staff see any kind of patient. The high traffic areas are something that everyone touches, hand washing is the easiest way to prevent trasmission of bacteria. There have been past methods to clean a room, such as standard cleaning products but that did not seem to get every surface. Because VRE is very adapt, only a little area of contaminated surface is all it takes to an infection to occur. To properly clean a room, an arriving method is to use hydrogen peroxide vapor(HPV) to clean the room in which there has been an uprising of VRE, this ensures that every surface of the room is exposed to the vapor. HPV is introduced through a ventilation system and interacts with all exposed surfaces. Monitors are present to ensure that there is no leakage and that levels are safe after the process. The vapor can then be broken down into water and oxygen by spontaneous reaction or could be moved to a specific area to break down by powerful aeration units or by the use of the buildings own air flow system. This process uses the same bio-applications to measure effectiveness and is held on the same level as an autoclave.
However, if a patient does become infected there are a few ways to deal with the infection. Linezolid is an antibiotic that is commonly used in place of vancomycin. There have been new antibiotics that are being used in the defense against VRE, but these are almost always used in combinations with older antibiotics. New research, does show that Lactobacillus was used to help treat an infection of VRE in the intestinal tract of patients (Manley 2000).
Conclusion
Prevention and treatment of VRE should be taken seriously due to it's ability to give up the resistance gene to other bacteria. MRSA is a highly infections bacteria that, if given a vancomycin resistance gene, would be immune to most antibiotics today. With prevention and understanding there is a chance that VRE could become better understood and treated to prevent spread and lessen the chance resistance genes being transferred. Preventing this bacterial infection would lessen hospital stays for patients and put everyone's mind at ease to know that there are precautions and methods for sterilizing a room to protect against infections. There will be less cases due to nosocomial infections and less of a chance for VRE to spread it's resistance.
References
[Centers for Disease Control and Prevention. Recommendations for preventing the spread of vancomycin resistance: recommendations of the Hospital Infection Control Practices Advisory Committee (HICPAC). MMWR 1995;44(No. RR-12)]
[Courvali, Patrice. "Vancomycin Resistance in Gram-Positive Cocci." Oxford Journals. 2006. Web. <http://cid.oxfordjournals.org/content/42/Supplement_1/S25.full.pdf+html>.]
[Heiken, Esther. "The Role of Enterococcal Surface Protein in the Pathogenesis of Enterococcus Faecium Infections." Dec. 2009. Web. <http://igitur-archive.library.uu.nldissertations/2009-1130-200122/heikens.pdf>. ]
[Launay A, Ballard SA, Johnson PD, Grayson ML, Lambert T (2006) Transfer of vancomycin resistance transposon Tn1549 from Clostridium symbiosum to Enterococcus spp. in the gut of gnotobiotic mice. Antimicrob Agents Chemother 50:1054–1062]
[Manley, KJ, MB Fraenkel, BC Mayall, and DA Power. "Probiotic Treatment of Vancomycin resistant Enterococci: a Randomised Controlled Trial." 2007. Web. <http://www.mja.com.au/public/issues/186_09_070507/man10966_fm.html>. ]
[Riedl, S., K. Ohlsen, G. Werner, W. Witte, and J. Hacker. 2000. Impact of flavophospholipol and vancomycin on conjugational transfer of vancomycin resistance plasmids. Antimicrob. Agents Chemother. 44:3189-3192.]
Edited by student of Joan Slonczewski for BIOL 238 Microbiology, 2011, Kenyon College.