Modern Treatments for Leprosy: Difference between revisions
No edit summary |
No edit summary |
||
| Line 7: | Line 7: | ||
[[image:Medievalleperimage.jpeg|thumb|300px|right|Figure 1. Image taken from a medieval text depicting a individual afflicted with leprosy. Source:http://www2.kenyon.edu/projects/margin/leper3.jpg]] | [[image:Medievalleperimage.jpeg|thumb|300px|right|Figure 1. Image taken from a medieval text depicting a individual afflicted with leprosy. Source:http://www2.kenyon.edu/projects/margin/leper3.jpg]] | ||
Dr. Gerhard H.A. Hansen, after whom the disease is named, identified the bacterium Mycobacterium leprae in 1873 and proved that the disease was of biological origin. The first breakthrough in medication to treat leprosy happened in the 1940’s with the introduction of the antibacterial drug dapsone. Since then more effective drugs have been introduced [2]. Until 2008 the bacterium Mycobacterium leprae was the only known causative agent of Hansen’s disease, when a new species of closely related bacterium, Mycobacterium lepromatosis, was discovered to cause DLL (diffuse lepromatous leprosy). This strain of Hansen’s disease is endemic to Mexico and while less studied than the other strain, it appears to have symptoms different from those caused by Mycobacterium leprae [3]. | Dr. Gerhard H.A. Hansen, after whom the disease is named, identified the bacterium <i> Mycobacterium leprae </i> in 1873 and proved that the disease was of biological origin. The first breakthrough in medication to treat leprosy happened in the 1940’s with the introduction of the antibacterial drug dapsone. Since then more effective drugs have been introduced [2]. Until 2008 the bacterium Mycobacterium leprae was the only known causative agent of Hansen’s disease, when a new species of closely related bacterium, Mycobacterium lepromatosis, was discovered to cause DLL (diffuse lepromatous leprosy). This strain of Hansen’s disease is endemic to Mexico and while less studied than the other strain, it appears to have symptoms different from those caused by Mycobacterium leprae [3]. | ||
Revision as of 02:50, 23 April 2015
History of Leprosy
The disease of leprosy, also known as Hansen’s disease, was believed to have originated in Asia. The earliest records of the disease in Europe appearing after Alexander the Great’s army returned from India and a second time with the return of Pompeii’s troops from Asia Minor. A document dating back to 600 B.C.E. from the Indian subcontinent describes a disease with symptoms consistent with those of leprosy. However, now the first believed reference to leprosy was recorded on Egyptian papyrus and can be dated back to 1550 B.C.E. Since then the disease has spread across the globe. Nowadays, leprosy is a treatable disease and with a much lower rate of incidence. Nonetheless, it is estimated that between one and two million people worldwide suffer from visible and irreversible disabilities left in the wake of the disease [1]. Leprosy can be cured and transmission prevented through antibacterial treatments. Be that as it may, in poorer and more remote parts of the world such as regions in Asia, Africa, and South America afflicted persons had less access to and fewer resources with which to obtain these drugs, thus increasing incidence of the disease and the number of individuals suffering from symptoms in the past.
Historically individuals infected with were cast out of society and poorly treated. Transmission of leprosy and the disease itself, were not well understood resulting in the ostracization and shunning of afflicted persons. Throughout varying parts of the world the disease was considered a curse or punishment from God [1].

Dr. Gerhard H.A. Hansen, after whom the disease is named, identified the bacterium Mycobacterium leprae in 1873 and proved that the disease was of biological origin. The first breakthrough in medication to treat leprosy happened in the 1940’s with the introduction of the antibacterial drug dapsone. Since then more effective drugs have been introduced [2]. Until 2008 the bacterium Mycobacterium leprae was the only known causative agent of Hansen’s disease, when a new species of closely related bacterium, Mycobacterium lepromatosis, was discovered to cause DLL (diffuse lepromatous leprosy). This strain of Hansen’s disease is endemic to Mexico and while less studied than the other strain, it appears to have symptoms different from those caused by Mycobacterium leprae [3].
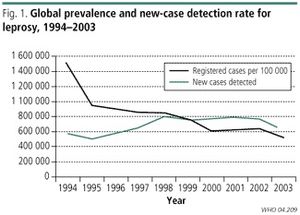
The World Health Assembly (WHA) initiated a program to eliminate Hansen’s disease as a public-health concern in 1991. They strived to accomplish this resolution by the end of the year 2000. The ultimate goal of this program was to reduce the prevalence rate of Hansen’s disease to less than one afflicted person per ten thousand people on a global scale. The goal of global elimination of the disease, by means of the prevalence rate of the disease, was accomplished by the set forth deadline. Since 1995, Multidrug Therapy has been distributed free to all persons afflicted by Hansen’s disease. This free distribution of medication is made possible with the assistance of the World Health Organisation (WHO). The decrease in the prevalence rate of the disease worldwide has been striking since the institution of the aforementioned public-health initiative, although Hansen’s disease is still endemic some developing countries, primarily in countries situated near the equator with tropical climates. As many as sixteen million symptomatic individuals are believed to have been cured of the disease over the past twenty years. Over the duration of that time the prevalence rate of Hansen’s disease is thought to have decreased by at least 90%. In 1985, before the public-health initiative against the disease was instigated, Hansen’s disease was considered a public-health concern in a total of 122 countries globally. Since then the disease has been eliminated in a total of 119 of those countries in which it was considered a public-health issue. However in more recent years there have been many reports of new cases. In 2012, official reports stated that over 230,000 new cases of Hansen’s disease were reported from 115 countries over the globe. Sixteen of these countries accounted for around 95% of the reported incidents of the disease. Some of the countries in which Hansen’s disease is more prevalent and a greater health concern than elsewhere in the world include India , China, Brazil and the Philippines. In 2009 it was recorded in the National Hansen's Disease Registry that there were 213 new cases of the disease reported in the United States. Between 150 and 250 newly diagnosed cases of Hansen’s are reported each year in the United States, most of these cases arising in individuals who had immigrated to the United States. The reason that the total elimination of leprosy is near impossible is due to the fact that Hansen’s is not an exclusively human pathogen. Several species of animals, such as armadillos and including some species of apes, such as chimpanzees, carry the bacterial agent that causes the disease, thus creating the opportunity for the pathogen to jump from one species to humans [2].
Signs and Symptoms
Symptoms of Hansen’s disease can take many years to materialize, often anywhere from two to ten years, due to the slow-growing nature of the bacteria. The majority of the symptoms affect the epidermis (skin), nerve cells and the mucus membranes lining bodily cavities, such as the lining of the throat and the nasal canals. Most symptoms are painful and can leave the afflicted person disabled if treatment is provided too late.
Skin lesions can appear that may in time become faded or discolored. Skin can become thick, stiff or dry and numbness in those affected areas of the skin may follow. Growths on the skin may appear, such as the characteristic boils seen in many patients which may then rupture. As a result of the fact that the infection affects the nerves, severe pain can occur as well as ocular nerve issues which can in turn lead to permanent damage that results in partial or total loss of eyesight in patients. Other problems with the nerves such as muscle weakness or paralysis, particularly in extremities, for instance the hands or feet, are common as well as enlarged nerves often around the knees or elbows. Ulcers on the soles of the afflicted persons feet can also be an issue. As the disease also affects mucous membranes, less serious symptoms such as nosebleeds, sinus infections and stuffy nasal canals can occur.
The effect of Hansen’s disease on the nerves is by far the most concerning aspect of the disease. Loss of feeling and sensation is particularly concerning because nerve damage can become a perpetual issue and leave an afflicted individual permanently disabled. Due to the loss of sensation and feeling, injuries may be disregarded. Untreated wounds can lead to infection and decrease the immune system’s ability to fight against the pathogen [4].
Multi Drug therapy
As there are multiple strains of Hansen’s disease there are three major combinations of drugs used to treat varying strains. Rifampicin is used solely in combination with dapsone in order to treat tuberculoid cases of Paucibacillary (PB) leprosy. Dapsone and rifampicin are also used in combination with clofazimine in order to treat lepromatous cases of Multibacillary (MB) leprosy. Recently a single dose treatment combining the drugs ofloxacin, rifampicin, and minocycline has been used as a treatment for single lesion paucibacillary leprosy. Dapsone was used as a monotherapy drug for a time until resistant strains of the disease evolved. Now, use of any one drug as a monotherapy treated is prohibited in order to attempt to prevent the mutation multi-drug resistant strains.
-Dapsone-
