Tetanus in sub-Saharan Africa: Difference between revisions
| Line 24: | Line 24: | ||
The severity of the effect of the toxin greatly depends on the incubation time, which may range from 3 to 21 days, where around 8 days is most common. Typically, the shorter the incubation time, the more severe the disease and there is a higher chance of death [11]. Incubation time and severity are also directly related to both the amount and the location of the site of the bacteria; a shorter incubation time means that the site is closer to the central nervous system, explaining the more severe response to the toxin [11, 12]. | The severity of the effect of the toxin greatly depends on the incubation time, which may range from 3 to 21 days, where around 8 days is most common. Typically, the shorter the incubation time, the more severe the disease and there is a higher chance of death [11]. Incubation time and severity are also directly related to both the amount and the location of the site of the bacteria; a shorter incubation time means that the site is closer to the central nervous system, explaining the more severe response to the toxin [11, 12]. | ||
===Symptoms=== | |||
===Transmission of disease=== | ===Transmission of disease=== | ||
Revision as of 02:03, 27 August 2009
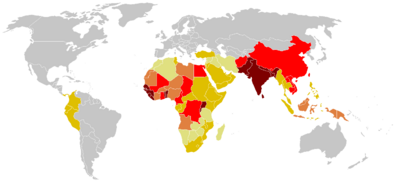
Introduction
Tetanus is a disease caused by the bacterium Clostridum tetani. The disease is caused by a neurotoxin released by the bacterium once inside the host, and causes deadly spastic paralysis. The neurotoxin is the second strongest toxin known to man, only second to the closely related Clostridum botulinum [4]. Records describing tetanus can be dated back to 5th century B.C. and are littered throughout medical military records from various periods of time [11,13]. The name is derived from the Greek word tetanos, from teinein, which means “to stretch,” [13]. The bacterium responsible for the disease, Clostridium tetani, was discovered in 1884 by Nicolaier, who injected animals with soil, and a pure culture was obtained in 1889 [11]. While tetanus used to be a rampant problem throughout the world in ages past, it has been controlled in recent decades through prevention in developed countries today. However, in developing regions of the world such as sub-Saharan Africa, it remains a critical issue in society: most maternal and neonatal deaths from this disease currently take place in this region [14]. With immunization from the tetanus toxoid, the disease is completely preventable. However, the WHO estimates up to 290,000 deaths each year, with 128,000 infant mortalities due to neonatal tetanus. In fact, the WHO reports it as the second leading cause of death from vaccine preventable disease [7].
Description of Microbe
Lineage( abbreviated ) Bacteria; Firmicutes; Clostridia; Clostridiales; Clostridiaceae; Clostridium [1]
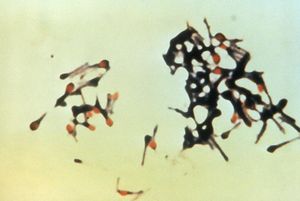
Structure and Function
Colstridum tetani are rod shaped bacilli, anaerobic fermenting, gram positive bacteria of the Clostridium genus. C. tetani are spore forming bacteria which form spores at their terminal ends, this gives them a tennis racquet like apprearance during sporulation [2]. C.tetani habituate low oxygen places such as soil, and animal instestine.[4] C. tetani are the cause of the disease Tetanus, which is caused by toxigenic species which carry the toxin producing gene on a plasmid. The two species have been found to be most susceptible to Tetanus neurotoxin are horses and humans. Tetanospamin is the toxin produced by these toxigenic species, but non toxic producing species have been found to exist. Most species of C. tetani are motile and form peritrichous flagella, in addition swarming is observed in some species. Other species are not immotile and do not form flagella [2]. C. tetani is not the only species in the Clostridium genus that produces endotoxins which are medically important neurotoxins, notably C. botulinum which produces botulism toxin. [3]
Genome
The genome of toxigenic C.tetani E88 a contains a chromosome with 2,799,250-bp and a 28.6% G+C content. However the plasmid (pE88) containing the toxin gene (tetX) contains 74,082-bp and a much lower 24.5% G+C content. The plasmid also contains the regulator for the toxin gene. Both the regulator and the toxin gene show homology to botulinum neurotoxins and regulator. Unlike many other enteropathogens the genome of C.Tetani, however has a very stable G+C content and not many transposable elements are found, evidence for lack of lateral transfer and genome stability. Some mobile elements are found on the plasmid however, including genes for transposase. The plasmid also contributes several other virulence factors, such a gene for collaginase, which may destroy host tissue integrity. The origin of the plasmid containing the toxin gene has yet to be revealed. It is not what enviormental signals turn on TeTx genes, or what regulates the activation of toxin transcription, however it is though that alternative sigma factors may be responsible. [4].
Bioenergetics
During their vegetate state C.tetani are anerobic and can not survive in the presence of oxygen, and use fermentation as their energy source. C.tetani are peptolytic, and prefer to use ammino acids and protein substances for fermations, however they have been shown to be able to grow on glucose, but not on polypeptides. C.Tetani excretes many exopeptidase to break down the proteins in the host tissue and then imports the peptides into the cytosol, using a sodium ion symporter.Unlike some bacteria which use a proton motive force, C.Tetani uses ATP as product of fermentation to establish an ion motive force by pumping out sodium ions via V-type ATPase. Sodium dependent systems are common among some thermophiles and other pathogenic bacteria. The influx of sodium is coupled to drive several transportation processes, some of which include multi-drug resistant exporters. [4]
Description of Disease
Pathophysiology
Two toxins are actually produced by Clostridium tetani, one responsible for the symptoms called tetanospasmin, and another with no known pathogenic properties called tetanolysin [12]. Tetanospasmin acts by cleaving proteins that are involved in vesicle fusion, thereby inhibiting neurotransmitter release. It acts at many sites located in the central nervous system, including the spinal cord and the brain, as well as sites in the autonomic nervous system, namely the sympathetic nervous system. Tetanospasmin is cleaved after translation into a light and heavy chain [12, 10]. It is the carboxyl terminal of the heavy chain that binds to gangliosides on peripheral nerves, allowing it to enter the system. Both binding and protein transport are attributed to the heavy chain. The toxin is passed to the central nervous system from the peripheral nervous system by way of trans-synaptic transmission and retrograde axonal transport, finally entering presynaptic cells [10]. In the presynaptic cells, the toxin’s light polypeptide chain cleaves an essential intergral membrane protein, called synaptobrevin, that is needed for the fusion of synaptic vesicles to the cell [10]. This action thus prevents the release of important inhibitory neurotransmitters such as GABA, to be released into the synaptic cleft. The final result of this inhibition is the unregulated release of excitatory signals, causing continual muscle contraction as well as painful muscle spasms that may ultimately lead to respiratory arrest and subsequently, death [12, 10].
The severity of the effect of the toxin greatly depends on the incubation time, which may range from 3 to 21 days, where around 8 days is most common. Typically, the shorter the incubation time, the more severe the disease and there is a higher chance of death [11]. Incubation time and severity are also directly related to both the amount and the location of the site of the bacteria; a shorter incubation time means that the site is closer to the central nervous system, explaining the more severe response to the toxin [11, 12].
Symptoms
Transmission of disease
Tetanus is a disease caused by the bacterium Clostridium tetani, which releases an exotoxin inside the host [12]. Exposure to the bacteria usually happens by way of a wound; contact with soil containing dirt, feces, and other similar components raises the risk. Once a wound has allowed the bacteria to enter, they live in the necrotic tissue and produce the toxin, which is then carried throughout the body by the bloodstream and lymphatic system. Due to the fact that the organism is an anaerobe, the damaged tissue is required for its survival inside the host. The disease cannot be transmitted person to person [11].
Clinical Treatment and Vaccinations
Tetanus treatment begins with cleaning the wound, surgically if necessary, and removing the source of the toxin. In addition, the use of antibiotics, such as penicillin, clindamycin, erythromycin and metronidazle is used to battle tetanus longevity. To relax the muscles, often times bedrest is encouraged coupled with muscle relaxers and sedatives.
Tetanus toxoid, a chemically modified toxin from tetanus that is no longer toxic but is still antigenic and is used as a vaccine, (TT) is a T cell dependent antigen that induces long-lasting immunity against tetanus. The immune response to TT vaccination shows that protection is dependent on the amount of IgG antibodies, the subclass distribution which is mainly dominated by IgG1, and the overall strength of binding between the antibody and the antigen of the produced antibodies. The binding strength between the antibody and the antigen is used to measure the efficiency of the antibodies to neutralize the antigen because it reflects the collective functional affinities of the antibodies that are formed during a humoral immune response. Tetanus toxoid and improved wound management, including the use of tetanus prophylaxis has shown to decline the rate of tetanus throughout the world. However, for areas like sub-Sahara Africa, the necessary resources may not be available.
Prevention
Tetanus is preventable by continued immunization. Immunization is expected to last ten years. In the United States, immunizations begin at birth with the DTaP series of shots that is a three-in-1 vaccine that targets diphtheria, pertussis, and tetanus. A Td vaccine is also a booster used to continue immunity from the ages of 11 to 65. If an individual suffers an injury such as a punctured-wound, a tetanus booster immunization should be administered immediately if more than ten years have passed since the last immunization. Although maintained immunization is the key way to prevent tetanus, developing areas such as the sub-Sahara may not have the adequate resources for continued prevention, which is why there is an increased infected rate in those areas.
Why is this disease prevalent in sub-Saharan Africa?

Since maternal and neonatal tetanus cases are prevalent in poor, developing communities, many newborns die due to poor access to good healthcare. Furthermore, people in major developing countries, such as people in Sub-Saharan Africa, may not receive the most promising vaccination coverage or immunization. Most women of childbearing age in the developing country are not even provided with immunization with tetanus toxoid, which immunizes women of childbearing age in order to enhance transfer of tetanus antibodies into their systems and protecting their newborns from catching neonatal tetanus. [5]
Tetanus is most common in hot, damp climates with soil rich in organic matter for spores to grow. This explains why Sub-Saharan Africa is such a prominent country for neonatal tetanus. Exposure to the spores of the bacterium, Clostridium tetani, is caused by the potent neurotoxin produced during the growth of bacteria in an anaerobic environment. Once the bacterium proliferates into the dead tissues, it releases toxins for spore germination as soon as the bacteria lyses. The toxin that was previously introduced to the body or synthesized as an inactive polypeptide chain during bacterial growth phage, is then transformed by bacterial or tissues proteases into its active form. [6] Tetanus spores, unfortunately, cannot be removed from the environment, causing tetanus to be spread through spores that were exposed to the intestines and feces of various animals. Spores can also be launched into the body through puncture wounds that have already been contaminated by the soil, animal waste, or any nature of debris.
Neonatal tetanus, the most common tetanus in the developing world, is the result of contamination of the umbilical stump by the usage of non-sterile instruments or animal dung to cut the cord after delivery. Many newborn deliveries are performed at homes by untrained birth attendants. Most people in Sub-Sahara African do not have a profound understanding of dangerous causes of neonatal tetanus on their children.[5] In fact, neonatal tetanus is a huge problem in Sub-Sahara Africa because of the lack of maternal and paternal education, the unavailability of effective contraception, improper hygienic deliveries and cord care. Large numbers of Sub-Saharan Africa physicians leave their homeland to practice medicine or upon completion of their medical school practices in search of expanding their work experience in higher-income countries. This leaves many Africans in distress of receiving proper healthcare systems. In Sub-Saharan Africa, life expectancy is only 50 years with about less than 32% of the deliveries are attended by trained personnel. People in Sub-Saharan Africa suffer from poor health systems, which greatly hinder the country from taking a huge step towards improving their infrastructures of healthcare and eliminating diseases.
What is being done to address this problem
Include anything being done by the local government or groups as well as efforts by non-local groups.
What else could be done to address this problem
Are there solutions that could be successful but haven't been implemented due to political or economic reasons? Are there successful efforts in other countries? Are there reasons why these efforts may or may not be successful in the country you've focused on? etc. etc.
References
1.) NCBI taxonomy
7.) World Health Organization. Vaccine-Preventable Diseases. "Tetanus". http://www.who.int. WHO 2009.
9.) Medline Plus
Images courtesy of Center for Control and Disease Prevention. Public Health Image Library (PHIL).
Edited by Freyr Petursson, Megan Glasheen, Meghan Wu, Chris Fascenda, David Cervantes, Lisa Sugimori, students of Rachel Larsen
This template is just a general guideline of how to design your site. You are not restricted to this format, so feel free to make changes to the headings and subheadings and to add or remove sections as appropriate.
