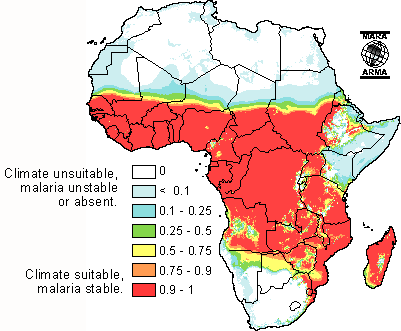
Malaria (Plasmodium falciparum) in sub-Saharan Africa
Introduction
Malaria is an infectious disease caused by the parasitic protozoan 'Plasmodium', which can only be transferred by the female Anopheles mosquito. Malaria is spread when the mosquito bites into a person who is already infected. The parasites from the blood uptake reproduce in the mosquito and mix with the saliva so that the next time the mosquito bites another person, parasites are transferred.[1]
There are four parasitic protozoans which cause malaria: Plasmodium falciparum, Plasmodium malariae, Plasmodium ovale, and Plasmodium vivax. Of these parasites, Plasmodium falciparum is the most dangerous and can cause coma or death.[2] Symptoms include high fever, chills, vomiting, and nausea and they don’t appear until 10-15 days after the initial mosquito bite.[3]
Malaria, which is Italian for “bad air,” has been infecting humans since the last Ice Age, more than 20,000 years ago in sub-Saharan Africa and the Mediterranean region.[4] It was first documented in Chinese medical scripts in 2700 BCE and later in Greece in the 4th century BCE. It was then that Roman writers attributed malaria to swampy areas. The discovery of a tree bark that remedies malaria was discovered in the early 17th century – Spanish missionaries in South America were introduced to the bark by local Indian tribes to cure fevers. The medicine in the bark, now called quinine, is currently being used as anti-malarial drug.[5]
The World Health Organization estimates that 300-500 million cases of malaria occur annually worldwide and more than one million victims are killed every year. About 90% of these deaths are from sub-Saharan Africa, occurring mostly in children under the age of 5.[6] 50,000 deaths occur in Zambia alone. 1 in every 5 children in Africa die from malaria, and costs Africa’s gross domestic product approximately $12 billion per year in lost wages due to debilitating effects of the disease.[7][8] Although malaria is preventable and curable, misuse of antimalarial drugs over the past century led to parasitic resistance to these malaria medications.[9]
Description of Malaria
Description of the microbe
Include a link if there is an existing microbewiki page. Ex. Salmonella typhi
Transmission of disease
How is it transmitted? Is there a vector (animal/insect)?
Prevention
Why is this disease a problem in sub-Saharan Africa
Do lifestyle/environment/economics/political issues play a role?
What is being done to address this problem
Include anything being done by the local government or groups as well as efforts by non-local groups.
What else could be done to address this problem
Are there solutions that could be successful but haven't been implemented due to political or economic reasons? Are there successful efforts in other countries? Are there reasons why these efforts may or may not be successful in the country you've focused on? etc. etc.
Because anti-malaria drugs and vaccines are so expensive and limited, it’s important to invest money into diagnostic products that are effective and accurate. Misdiagnosis of malaria leads to too many prescriptions of limited drugs and vaccines. In the past couple of months, 30.8% of the patients were misdiagnose and 29.3% were given drugs they didn’t need [7]. With microscopy and the rapid diagnostic test (RDT), patients can be diagnose accurately. Diagnosis of malaria is 93.5% accurate with microscopy and 97.5% accurate with RDT [8]. RDT detects the parasitic antigens that are present in malaria quicker and more accurate than microscopy[9]. Although RDT is more expensive than microscopy, it needs to be implemented in areas that have severe cases of malaria. Since the diagnosis are quick and accurate, treating patients with malaria will be more cost efficient and there will be more vaccines and anti-malaria drugs to be used efficiently. Overtime the money saved on misdiagnosed patients will cover the costs of RDT [10]. In the absence of microscopy and RDT, pregnant women and children five and younger with high fevers are automatically given anti-malaria drugs because they are more prone to malaria.
References
[1] "WHO | Q&A: malaria." WHO | World Health Organization. Web. 18 Aug. 2009. <http://who.int/topics/malaria/qa/en/index.html>.
[2] "WHO | Malaria." WHO | World Health Organization. Jan. 2009. Web. 18 Aug. 2009. <http://www.who.int/mediacentre/factsheets/fs094/en/index.html>.
[3] "WHO | Malaria." WHO | World Health Organization. Web. 18 Aug. 2009. <http://www.who.int/topics/malaria/en/>.
[4] Carter, Richard. "Speculations on the origins of Plasmodium vivax malaria." Trends in Parasitology 19.5 (2003): 214-19. ScienceDirect. Cell Press, 3 Apr. 2003. Web. 27 Aug. 2009. <http://www.sciencedirect.com/science?_ob=ArticleURL&_udi=B6W7G-488VVXW-2&_user=4429&_rdoc=1&_fmt=&_orig=search&_sort=d&_docanchor=&view=c&_acct=C000059602&_version=1&_urlVersion=0&_userid=4429&md5=0f976cb9b27708cfc41234aae0663f93>.
[5] "History | CDC Malaria." Centers for Disease Control and Prevention. 23 Apr. 2004. Web. 27 Aug. 2009. <http://www.cdc.gov/Malaria/history/index.htm>.
[6] "Frequently Asked Questions | CDC Malaria." Centers for Disease Control and Prevention. 17 Dec. 2008. Web. 18 Aug. 2009. <http://www.cdc.gov/malaria/faq.htm>.
[7] "Africa - Striking Back at Malaria in Sub-Saharan Africa." The World Bank. Web. 18 Aug. 2009. <http://go.worldbank.org/HKLWTF8890>.
[8] "UNICEF - Press centre - Africa Malaria Day 2007." UNICEF - UNICEF Home. United Nations Children's Fund. Web. 18 Aug. 2009. <http://www.unicef.org/media/media_39453.html>.
[9] "WHO | 10 facts on malaria." WHO | World Health Organization. Web. 18 Aug. 2009. <http://www.who.int/features/factfiles/malaria/en/index.html>.
Edited by Andy Chen, Alice Nguyen, Kris Vasant, Chirag Yadav, Matthew Hsia, Renu Gaur, and Amreeta Panesar, students of Rachel Larsen
This template is just a general guideline of how to design your site. You are not restricted to this format, so feel free to make changes to the headings and subheadings and to add or remove sections as appropriate.
