Enterobacter aerogenes
A Microbial Biorealm page on the genus Enterobacter aerogenes
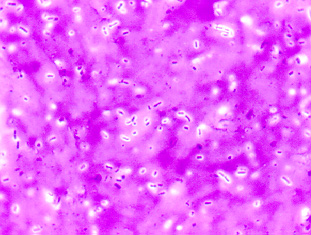
Classification
Higher order taxa
Bacteria; Proteobacteria; Gammaproteobacteria; Enterobacteriales; Enterobacteriaceae; Enterobacter
Species
Enterobacter aerogenes
Discussions on the true taxonomy of E. aerogenes presently exist due to the genomic distance between E. cloacae and Klebsiella. Research shows that E. aerogenes is more closely related to Klebsiella (47-64%) than E. cloacae (44%).
Description and significance
The Enterobacteriaceae family includes genera of Escherichia, Shilgella, Salmonella, Enterobacter, Klebsiella, Serratia, Proteus, amongst others. The gram-negative bacteria resides in soil, water, dairy products and inhabits a natural flora in the gastrointestinal tract of animals as well as humans. The rod shaped Enterobacteriaceae exists in a variety of sizes; are not spore forming; are both motile (with peritrichous flagella) or nonmotile; grow both aerobically and anaerobically; are active biochemically; ferment (versus oxidize) D-glucose as well as other sugars, often with gas production; reduce nitrate to nitrite; contain the enterobacter common antigen; and have a 39-59% guanine-plus-cytosine (G + C) content of DNA (2).
The genus Enterobacter is more specifically a nosocomial opportunistic pathogen and is sought out to be one of the many key causes for extraintestinal infections next to E. coli. Infections commonly attributed to E. aerogenes are respiratory, gastrointesntinal, and urinary tract infections, specifically cystits, in addition to wound, bloodstream, and central nervous system infections (1,2,3). Furthermore, E. cloacea and E. aerogenes are the species most commonly associated with aduilt cases of meningitis. Colonies of Enterobacter strains may be slightly mucoid.
In the clinical setting, Enterobacter aerogenes and Enterobacter cloacae are the most frequently isolated in samples of infected hospitalized patients. The majority of the infections are etiologically due to inadvertent transfer of bacteria during surgery or prolonged treatment in hospitals in patients who use venous or urethral catheters. Enterobacteriaceae may account for 80% of clinically significant isolates of gram-negative bacilli and for 50% of clinically significant bacteria in clinical microbiology laboratories. Additionally, they account for nearly 50% of septicemia cases and more than 70% of urinary and intestinal tract infections. The severity of these infections thus create an importance to target, isolate, identify and test for susceptibility for the causes of these nosocomial infections (2).
Genome structure
E. aerogenes are smaller, rod-shaped cells that are motile and encapsulated compared to others in the same family of Enterobacteriaceae. The complete genomic information (88% is coded) has not been entirely sequenced as of yet, however, there is some research that shows studies on mutations as well as show evidence of replication through plasmids. E. cloacae and E. aerogenes stain samples had no extrachromosomal elements (9). Plasmid analysis remains as one of the most utilized laboratory techniques used, but PFGE, RAPD, ribotyping, enterobacterial repetitive intergenic consensus (ERIC), PCR, and amplified fragment length polymorphism is also used. The replicon name is R751. The bacteria consists of DNA and is circular. Its length is recorded as 53,435 basepairs long and contains no structural RNAs. The G + C content is 64% and no psuedo genes are recorded for E. aerogenes (9).
Cell structure and metabolism
Enterbacter aerogenes is a gram-negative, rod shaped bacterium that contains flagella surrounding it's outer surface. E. aerogenes as well as others in its genus are known to be resistant to antibiotics, especially E. aerogenes and E. cloacae. Research shows that two clinical strains of E. aerogenes exhibited phenotypes of multiresistance to β-lactam antibiotics, fluoroquinolones, chloramphenicol, tetracycline, and kanamycin. Both strains showed a porin pattern different from that of a susceptible strain. They had a drastic reduction in the amount of the major porin but with an apparently conserved normal structure (size and immunogenicity), together with overproduction of two known outer membrane proteins, OmpX and LamB (8).
Ecology
Enterobacter are found in the soil, water, dairy products, and in the intestines of animals as well as humans. They are most frequently found in the gastrointestinal tract and are studied in clinical sites in stool samples. The minimum, optimum and maximum pH for E. aerogenes replication is 4.4, 6.0-7.0, and 9.0 (6).
Enterobacter aerogenes has been plated on several different medias and have been observed under several types of testing. The results are as follows- E. aerogenes tested negative when treated with/for: Indol, Methyl red, Hydrogen sulfide (by way of TSI), Urease, Arginine dihydrolase, Phenylalanine deaminase, and Dulcitol. E. aerogenes tested positive when treated with/for: Voges-Proskauer, Simmons' citrate, KCN, Motility, Lysine decarboxylase, Ornithine decarboxylase, Gas from glucose, Lactose, Sucrose, Manntiol, Salicin, Adonitol, Inositol, Sorbitol, Arabinose, Raffinose, and Rhamnose. Delayed positive results were obtained from: Gelatin (22°C) and Malonate (11). In other words, E. aerogenes resembles E. cloacae but the leusine decarboxylase test is positive and gelatin liquification is late. E. aerogenes is also, often times confused with Klebsiella aerogenes. However, E. aerogenes is motile and urease negative while K. aerogenes is nonmotile and urease positive (5). In actuality, research shows that "E. aerogenes is more related to Klebsiella aerogenes (47-64%) than it is to E. cloacae (44%) (9).
Different species of Enterobacter like E. cloacae are known to be found on a number of seeds and plants while E. sakazakii is commonly seen in infants who were given infant milk-based powder formulas (9).
Pathology
Enterobacter aerogenes causes disease in humans through inadvertent bacteria transfer in hospital settings. A selection of enteric bacteria like E. aerogenes are opportunistic and only infect those who already have suppressed host immunity defenses. Infants, the elderly, and those who are in the terminal stages of other disease or are immunosuppressed are prime candidates for such infections (9).
Additionally, E. aerogenes as well as other enteric bacteria, is known to have drug-resistant characteristics. There has been some success in dealing with infections through antibiotics, however, the fast development of multidrug resistence has become an increasingly growing problem (3). These multiresistant strains have caused outbreaks in intensive care units (ICUs) in Belgium, France, Austria, and the United States and has further become more emergent than its sister species E. cloacaw (12). Research has shown that E. aerogenes is resistant to ampicillin and it has been more recently discovered that it is resistant to imipenem (11).
In general, the pathogenic mechanisms expressed by strains of Enterobacter are unknown. Like other strains such as Klebsiella, they express type 1 and type 3 fimbraie. Most strains also express an aerobactin-mediated iron uptake systems, commonly associated with extra-intestinal human bacterial pathogens. Some strains may produce a haemolysin resembling the α-haemolysin produced by strains of E. coli. Additionally, an outer membrane protein, OmpX, may be a pathogenic factor for strains E. cloacae. This particular protein appears to reduce the production of porins on the gram-negative bacteria, leading to decreased sensitivity to β-lactam antibiotics and therefore might play a role in cell invasion of the host (7).
Enterobacter species produce type 1 or type 3 mannose sensitive hemagglutinins (MSHA) and rarely produce mannnose-resistant hemagglutinins. The only exception being E. gergoviae. Additionally, production of a variety of siderophores by enterobacters is also commonly seen. E. cloacae generate the hydroxyamate siderophore aerobactin, which is commonly used with microbial species that cause invasion disease. Additionally, several toxins have been found to be produced by Enterobacter species. Usually these toxins are described to having single strains or are limited in the number of isolates (9).
Preventative measures can be taken to reduce infection of E. aerogenes by monitoring careful, aseptic surgical techniques (3). Catheters should be removed and venous needles and tubing should be taken out and put in new locations. Treatment for E. aerogenes is difficult due to the highly resistant nature of the species. Enterobacter strains are resistant to penicillins and other cephalosporins because of the production of chromosomal beta-lactamase with cepholosprinase activity. Additionally, many are resistant to tetracycline, chloramphenicol and to streptomycin, as well as other aminoglycosides (such as gentamicin and fluoroquinolones). Most strains may appear to be susceptible to cefotaxime on primary testing, however, they often possess an inducible chromosomal cephalosporinase, allowing for the rapid development of resistance during treatment or therapy (7).
Risk factors for nosocomial Enterobacter species like E. aerogenes infections include hospitalization of greater than 2 weeks, invasive procedures in the past 72 hours, treatment with antibiotics in the past 30 days, and the presence of a central venous catheter. Specific risk factors for infection with nosocomial multidrug-resistant strains of Enterobacter species should be taken into account and include the recent use of broad-spectrum cephalosporins or aminoglycosides and ICU care (13).
Application to Biotechnology
Studies show that E. aerogenes has an increasing drug resistance rate. High levels of drug resistance in enterobacteria were found in accordance to aminoglycosides and broad-spectrum and fourth generation ceftazidime (>40%) and cefepime (15%). E. aerogenes stains showed production of extended-spectrum β-lactamases (ESBLs). A resistance such as this one often arises de novo in patients receiving empiric therapy for systemic infections. These drug resistant enterobacters can later emerge to produce severe or fulminant illnesses in immunosuppressed patients (9). Drug resistance such as these are common products of Enterobacter. Several drug therapies appear to be effective, however, after prolonged treatment, resistance arises and new drugs must be administered.
The involved resistance mechanisms exhibited by strains of E. aerogenes are associated with alterations of the outer membrane that cause a porin decrease and lipopolysaccharide modifications. As a result of its antibiotic resistance, many researchers have reverted back to "old drugs" such as colistin in addition to imipenem to treat severe E. aerogenes infections.
Current Research
In a case study used to determine the cause of infections in the aorta, isolation of two strains: S. pneumoniae and E. aerogenes were discovered and extracted from a 72 year old male suffering from epigastric pain, fevers, and chills. The orgin of E. aerogenes is unknown but is thought to be a result from and undiagnosed urinary tract infection or pneumonia. Research prior to this indicate that this case study is only the second report in the literature noting multiple organisms in infectious aortitis concerning E. aerogenes and S. pneumoniae. In addition to this, Enterobacter has only been reported as a cause of infectious aortitis in the setting of aortic grafts. This is the first time that Enterobacter has been reported in cryptogenic infectious aortitis. The study concluded that infections of the aorta are rare, are caused by various pathogens, and are difficult to diagnose. Symptoms that the patients may experience include fever and abdominal pain (and a palpable, pulsatile abdominal mass if the aorta is aneurysmal). Blood cultures, if positive, can be helpful, as are CTA, and leukocyte scintigraphic imaging. A high index of suspicion is necessary as the mortality, if only treated medically, approaches 100%. Combined surgical and medical therapy is superior, reducing the mortality rate to between 20% and 60% (14).
The Enterobacter aerogenes eefABC locus, which encodes a tripartite efflux pump, was cloned by complementation of an Escherichia coli tolC mutant. E. aerogenes became less susceptible to a wide range of antibiotics. Data from eef::lacZ fusions showed that eefABC was not transcribed in the various laboratory conditions tested, but instead increased transcription from Peef (from an E. coli hns mutant). Additionally, EefA was detected in E. aerogenes expressing a dominant negative E. coli hns allele. Research concluded that many H-NS target genes are involved in bacterial adaptation to stressful environmental conditions and virulence. The biological relevance of the eef operon silencing is still not known. However, like other commensal or pathogenic bacteria, E. aerogenes has to undergo drastic changes in its gene expression profile in order to adapt to the host-associated conditions (15).
Other Enterobacter are being observed especially those concerning the species Enterobacter sakazakii which is an infant formula-borne pathogen that causes severe meningitis, meningoencephalitis, sepsis, and necrotizing enterocolitis in neonates and infants, creating a high fatality rate. The outer membrane protein A gene (ompA) and sequences from E. sakazakii (ATCC 51329), were cloned in the pGEM-T Easy vector and sequenced. A high degree of homology with ompA genes of other gram-negative bacteria belonging to the Enterobacteriaceae was discovered when the nucleotide and deduced amino acid sequences were compared to those in GenBank. The proteins were found to have an identity of 89% and a sequence conservation of 94% at the amino acid level. Similarly, the ompA gene of E. sakazakii had sequence identities of 86% and 88% at the nucleic acid and amino acid levels. Additionally, with Enterobacter aerogenes, 87% and 90% with serovar Typhimurium, and 85% and 88% with Shigella flexneri. A signal peptide cleavage site prediction analysis thus revealed a 21-amino-acid N-terminal signal sequence similar to those found in E. coli, E. aerogenes, S. flexneri, and S. enterica serovar Typhi (16).
References
1. Brooks, Geo F., MD; Karen C. Carrol, MD; Janet S. Butel, PhD; Stephen A. Morse, PhD. Jawetz, melnick, & Adelberg’s Medical Microbiology. 24th ed. New York: McGraw Hill, 2007.
2. Lederberg, Joshua; Martin Alexander [et al.]. Encyclopedia of Microbiology. 2nd ed. San Diego, Ca.: Academic Press, 2000
3. Sankaran, Neeraja. Microbes and People an A-Z of Microorganisms in Our Lives. Phoenix, Az.: Oryx Press, 2000
4. National Center for Biotechnology Information site: http://www.ncbi.nlm.nih.gov/sites/entrez?Db=genome&Cmd=ShowDetailView&TermToSearch=11232
5. Collins, C.G.; P.M. Lune, J.M. Grange, J.O Falkinham III. Microbiological Methods. 8th ed. London: Arnold, 2004
6. Atlas, Ronald M.; Richard Bartha. Microbial Ecology Fundamentals and Applications. 4th ed. Menlo Park, Ca.: Bemjammin/Cummings Publishing Company, Inc., 1998
7. Greenwood, David; Richard C.B. Slack; John F. Peuthere. Medical Microbiology, a Guide to Microbial Infections: Pathogens, Immunity, Laboratory Diagnosis and Control. Edinburgh: Churchill Livingstone, 2002
8. National Center for Biotechnology Information site: http://www.pubmedcentral.nih.gov/articlerender.fcgi?tool=pmcentrez&artid=153306
9. Janda, J. Michael; Sharon L. Abbott. The Enterobacteria 2nd ed. Washington D.C.: ASM press, 2006
10. National Center for Biotechnology Information site: http://www.ncbi.nlm.nih.gov/sites/entrez?Db=genome&Cmd=ShowDetailView&TermToSearch=11232
11. Bailey, W.R. and E.G. Scott. Diagnostic Microbiology, 4th ed. St. Louis, Mo.: The C.V. Mosby Co., 1974
12. De Gheldre, Y. [et al.]. National Epidemiologic Surveys of Enterobacter aerogenes in Belgian Hospitals from 1996 to 1998. J Clin Microbiol. 2001 March 39(3): 889–896
13. Fraser, Susan L. MD, [et al.]. Enterobacter Infections. eMedicine. 2007 Jan.
14. Rhondina, Matthew T. [et al.]. Abdominal Aortitis due to Streptococcus pneumoniae and Enterobacter aerogenes A Case Report and Review. J Gen Intern Med. 2006 July; 21(7): C1–C3.
15. Masi, Muriel, [et al.]. The eefABC Multidrug Efflux Pump Operon Is Repressed by H-NS in Enterobacter aerogenes. J Bacteriol. 2005 June; 187(11): 3894–3897.
16. Kumar Mohan Nair, Monoj [et al.]. Cloning and Sequencing of the ompA Gene of Enterobacter sakazakii and Development of an ompA-Targeted PCR for Rapid Detection of Enterobacter sakazakii in Infant Formula. Appl Environ Microbiol. 2006 April; 72(4): 2539–2546.
Thiolas, Aurélie, Claude Bollet,[et al.] Successive Emergence of Enterobacter aerogenes Strains Resistant to Imipenem and Colistin in a Patient. Antimicrobial Agents and Chemotherapy, 2005 April; 49 (4): 1354-1358.
Parts of this page were created by Tiffany M. Liu, a student of Professor Rachel Larsen at the University of California, San Diego.
Parts of this page were created by students of M Glogowski
