Talk:MicrobeWiki
Brevibacillus laterosporus, a bacterial biological control agent of Western Corn Rootworm.
Background
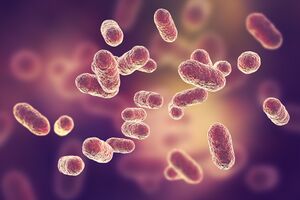
By Katya Naphtali
Underneath the umbrella of “pesticides”, there are biologically synthesized alternatives to chemicals called microbial pesticides. This alternative uses different microorganisms to target specific pests that threaten production. The actual material used as a pesticide is naturally formed, biodegradable, highly specialized to specific pests rather than having widespread impact meaning they can be used in small quantities with large effects (EPA). Microbial pesticides are commonly used to address pest control in corn crops. Stats on the importance of corn in USA agriculture, and the threat corn poses to it (monoculture). It is under threat by the Western Corn Rootworm (CRW), which specialized just to parasitize corn monocropping productions (Cornell). A common management process to address CRW is the incorporation of microbial pesticides into corn GMO strains (background on melding process?) Bacillus thergo (Bt) is the most commonly used bacteria as a source of microbial pest control. There are multiple strains of GMO corn that contain toxins from Bt. Unfortunately, in some regions where these GMOs are overused, CRW has adapted resistance to this toxin (Cornell). This drives researchers to search for similarly effective bacteria to replace their current technology.
Western Corn Rootworm
The Western Corn Rootworm (latin WCRW) is a species of Coleoptera (beetle) that specializes only in eating species of corn (latin). These beetles are ¼” long and yellow with black stripes along the sides of their elytra. They only have a single generation a year, because their life cycle is dependent on corn developmental stages (cornell source). Adult beetles lay their egg clusters below the soil surface for generation the following year, before dying themselves in the first winter frost (cornell). These eggs hatch during late May and early June into larva that are long small and white but sport brown heads with mandibles. They spend most of their larval stage feeding on the root zone of soil. They tunnel through dirt until finding corn roots to feed on. This tunneling can kill an entire root or break the tips of them, this prevents the plant from recieving enough nutrients causing it to either fall over, or greatly damage growth. The plant can be weakened in terms of stunting growth, reducing the yield amount, or even reducing the size of each ear of corn (cornell source). These larva undergo three instars of molting over a 4-6 week period (Iowa extension source). Before they pupate within the soil to undergo a compleme metamorphosis of their bodies into their adult forms. 5-10 days after pupation, CRW emerge as adults coinciding with when the corn plants flower (Iowa extension source). CRW beetles still consume during their adult stages, mainly corn pollen and corn silk, sometimes their leaves as well. Corn silk and pollen are both are needed for corn to pollinate eachother, so adults reduce their ability to reproduce (cornell source). Despite these negative impact, it is still less than the damage caused during their larval stage feeding on roots (Godfrey et al. 1993). In laying their eggs for the next generation, adult CRW are relatively stagnant species and do not tend to move fields for laying their eggs. As a result a common pest management technique for CRW is crop rotation with soy beans. Each year switching corn out for soybean plants prevents CRW from parasitizing their roots, causing CRW larva populations to drop due to the lack of their niche corn food source. Unfortunately, in some cases CRW have adapted to crop rotation schedules and have begun laying their eggs in soybean fields in anticipation of crop rotation to corn the following Spring when their offspring hatch (cornell source). This species adapts quickly due to its dependence on corn as its sole food source (Rausher et al.) As a result, other forms of pesticides are needed to be used alongside crop rotation (cornell source). One of these techniques include GMO corn strains that can be more resistant to these pests than non-GMO crops. A common GMO strain used to address CRW pest threats is Bt resistant corn.
NEED TO PUT INTO CITATION & FIGURE
Brevibacillus laterosporus
A number of Bacillus species have been investigated for pesticidal properties due to their formation of specialized biotoxins. Different species currently in use for biopesticides include: _____. While Bt is commonly regarded as the “most effective??” biopesticide, it has become less effective as CRW adapt to overcome its toxins (SOURCE). In recent years BL has become a bacterial species of more interest due to the speed in which it produces biotoxins, even if less powerful of a toxin than Bt produced (Ghazanchyan et al. & Oliviera et al.).
Brevibacillus laterosporus is rod-shaped with a gram-negative cell wall and relies on access to oxygen for metabolism. This bacteria produces a number of products including enzymes and prebiotic materials that function as an insecticides (Orlova et al.) B. lat can be sources from environmental soil, plants, and even the insects themselves (Ghazanchyan et al.). This bacteria produces endospores. On one end of each spore, this species of bacteria can be identified by its production of canoe-shaped paraposal bodies (a crystallized shell that contains endotoxins that can be used as pesticides (Ghazanchyan et al.). This bacteria has had almost an 100% effectiveness rate in the elimination of Coleopteran (beetles) pests depending on the strain, this was most effective in targeting these species during their larval stage, especially during their second instar (Favret et al.).
This species is of interest by biopesticide scientists due to the high rate in which it produces these paraposal bodies (pesticide containing structures) (Ghazanchyan et al.). Specialization??? These paraposal bodies can be HOW ARE THEY USED Bt resistant corn which uses toxins produced by Bacillus thergoneous to prevent parasitation. These Bt toxin BACKGROUND?? but if they are used to often CRW can become resistant to these strains. Bt is the most commonly used strain of resistant corn, and due to its over use, there are now multiple resistant strains of CRW both in Northwest Iowa and Southeast Minnesota. While these resistant strains mostly cannot move from field to field without accidental human transportation, they fortell the immunity that may be seen in other regions over-using this same resistant strain technique. As a result, new bacterial strains are being investigated to create new resistant corn GMO archetypes. Similar to crop rotation, a rotation of toxins may introduce more variety in pest control techniques that they will be less able to adapt to (cornell source).
Pathology & Experimental Use
Include some current research, with at least one figure showing data.
Real World Impacts
Conclusion
Root Worms
References
Authored for BIOL 238 Microbiology, taught by Joan Slonczewski, 2023, Kenyon College
