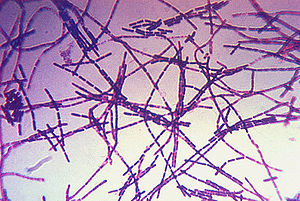
Bacillus Anthracis: Anthrax Lethal Toxin
Introduction
By Connor Gibbons
Anthrax is a disease that typically affects herbivores but can infect any mammal, including humans. It is caused by the bacterium Bacillus anthracis (B. anthracis). This disease has become a hot topic in today’s society, in which terrorism is becoming more prevalent, as it can be used in biological warfare. Recently, there has also been an increase in the number of cases of injection anthrax, a form of the disease that affects heroin users, in Europe (Grunow 2012). However, this disease is not new. In fact, there is evidence of it throughout history. The fifth and sixth plagues in Egypt (Exodus, Chapter 9) have been attributed to this pathogen (Baillie 2001).
The species derives its name from the Greek word anthrakis, meaning coal, because infection by the organism causes the formation of black, cutaneous eschars (Spencer 2003). There are are three types of B. anthracis infection that are typically described: cutaneous anthrax (the cause of the black sores), inhalation anthrax (the most deadly form), and gastrointestinal anthrax (Mock 2003)
Organism
Bacillus anthracis, a member of the genus Bacillus, is a Gram-positive, rod-shaped bacteria that typically forms short chains of cells. It is an aerobic organism that is also capable of functioning as a facultative anaerobe. Bacillus anthracis is the only obligate pathogen in its genus, and a large reason that it is such a dangerous bacteria is the fact that it can produce spores that are resistant to very adverse environmental conditions such as heat, radiation, pressure, and chemical agents (Mock 2001). These spores are able to live dormant in soil for decades (Spencer 2003). Virulent strains of B. anthracis contain two large plasmids, pXO1 and pXO2. The first plasmid, pXO1, is 184.5 kbp in length and it contains the genes that encode the three secretory toxins produced by the bacteria. These toxins are lethal factor (LF), edema factor (EF), and protective antigen (PA). The second plasmid, pXO2, contains the genes capA, capB, and capC. These genes code for protein products that are involved in the synthesis of the polyglutamyl capsule, which functions to prevents phagocytosis of the active, vegetative form of B. anthracis. The loss of either of these plasmids typically results in at least a partial loss of virulence (Spencer 2003). It has been observed, however, that high concentrations of the bacteria will still cause infection, even without the pXO2 plasmid. Further evidence shows that LF and EF work in tandem in the host organism to cause virulence, so EF- or LF-deficient mutants are not as effective at causing death or edema respectively (Mock 2001).
Genome
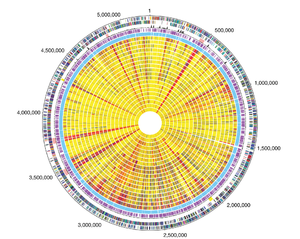
Though there are a large number of B. anthracis strains, perhaps the most well known is the Ames strain. The Ames strain got its name from the United States Army Medical Research Institute of Infectious Diseases who received the sample from the National Veterinary Services Laboratories in Ames, Iowa. This was a mistake as the original sample was taken from a diseased cow in Sarita, Texas in 1981. Due to its virulence the Ames strain, which was found to be the strain used in the 2001 bio-terror attacks in the United States, is the de facto strain used in the development and testing of vaccines (Read 2003).
In 2003, Read et al. sequenced the Ames strain in its entirety to learn more about the virulence activity as it relates to the bacterial chromosome. They found that the vast majority of the chromosomal gene products of B. anthracis have homologues to the gene sequence of B. cereus, a very closely related species. There were only 141 proteins that could not be assigned a function or that no homologue could be found, and nearly all of the proteins that could potentially have an effect on the virulence of the bacteria are also produced by B. cereus, indicating that they are not specifically associated with B. anthracis pathogenicity (Read 2003).
Some of these homologues that are known to be involved in the pathogenic pathways of other species (B. cereus and B. thuringiensis) include two type III hemolysins (BA5701 and BA2241) as well as three non-hemolytic enterotoxins (BA1887-1889). Other homologues known to be involved in the pathogenicity of the species Listeria monocytogenes were found on the chromosome, including two forms of a phospholipase, internalin-like genes, listoriolysin O, sigma factor B, and an extracellular protease p60. Other homologues have also been noted in the genome of B. anthracis, and the complete gene sequence can be seen in Figure 2 (Read 2003).
Life Cycle
The Spore
When B. anthracis, in the vegetative form, enters the environment, leaving a dying host organism, sporulation occurs. Dormant endospores are the infectious particle of B. anthracis; infection only takes place when an endospore enters the body from the environment, whether through an abrasion on the skin of an organism, through ingestion, or through inhalation. Spores are ideal infections particles because, as mentioned earlier, they are extremely resistant to adverse environmental conditions (Mock 2001). There have not been any observed cases of transmission of the disease between two living animals in the wild, because this would require the transfer of vegetative bacterial cells, not spores (Hanna 1999).
Germination
When B. anthracis spores enter a host organism, they are phagocytosed by regional macrophages and transported to the lymph nodes (Rao 2010). There, receptors on the inner membrane of the spore bind to molecules called germinants, which begins the germination process. The binding of the receptors causes rehydration of the spore and disintegration of the cortex and the coat (Driks 2009), leaving the vegetative form of B. anthracis. Infection of the host organism proceeds until it is treated or the host dies, releasing the cells into the environment and starting the process over.
Pathogenesis
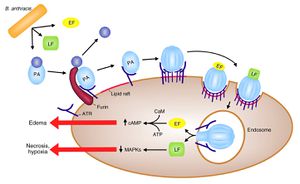
As noted above, infection by B. anthracis begins with the germination of a spore in the host organism. When germination occurs, the vegetative bacteria enter the blood stream and begin rapid extracellular multiplication. At this time, synthesis and extracellular secretion of capsule proteins and exotoxins also begins.
The exotoxins of B. anthracis act in binary combinations (LF + PA and EF + PA) to form lethal toxin (LeTx) and edema toxin (EdTx). Protective antigen molecules act by binding to a receptor on a target cell, inserting into the cell membrane, and translocating the bound toxin factor into the cytosol of the target cell (Langer 2012). This is accomplished by the binding of PA to anthrax toxin receptor (ATR), a membrane protein located in many cell types. PA is then cleaved by a furin-family protease to reveal the LF and EF binding sites. PA then oligomerizes into a hepatomer and binds LF or EF, a competitive process between the two toxin factors. The newly formed LeTx or EdTx complexes are activated by acidic conditions in an endosome when they enter the cell via endocytosis, and they are then transferred into the cytosol.
Inside the cell, EF is an adenylate cyclase, which converts intracellular ATP into cAMP, a process that is dependent on the protein calmodulin, which is produced by the host cell and acts as a ligand for EF. This process causes a dramatic increase in intracellular cAMP, disrupting cell signalling as well as membrane permeability regulation, which leads to edema at and around the infection site (Chung 2013). In the case of inhalation anthrax, this edema presents as pleural effusion. Lethal factor is a zinc metalloprotease that cleaves the N-terminus of mitogen-activated protein kinases (MAPKKs), which are involved in cell signaling pathways (Mock 2003). This process is illustrated in Figure 2. The exact physiological mechanisms by which LeTx and EdTx kill the organism are not yet known.
Clinical Symptoms and Diagnosis
Cutaneous Anthrax
Cutaneous anthrax infection occurs when B. anthracis spores enter the host via an opening in the skin, such as an abrasion, cut, or insect bite. In the two to three days post-infection, a small pimple-like papule forms. During the next 24 hours , vesicles form, making a raised ring around the papule, which ulcerates at this time. This ulcer dries out, forming a painless, black eschar, from which B. anthracis gets its name. Edema will be present around the site as well. In an uncomplicated case of cutaneous anthrax, the bacteria will not spread beyond the lesion, but if the infection is left untreated, ~20% of patients will become septic, which is very likely fatal (Spencer 2003).
Gastrointestinal Anthrax
Gastrointestinal anthrax occurs when a human or other animal ingests contaminated meat that contains B. anthracis spores. This type of infection is very rare, and outside of Asia and Africa, few if any cases have been reported. Clinicians divide cases of this type of infection into two categories: abdominal and oro-esophageal. Patients suffering from the abdominal form experience nausea, vomiting, anorexia, and fever. These symptoms quickly progress are followed by increasing acute abdominal pain, bloody diarrhea, septicemia, and death. The oro-esophageal form of gastrointestinal anthrax presents with patients symptoms including sore throat, dysphagia, fever, cervical lymphadenopathy (enlargement of the lymph nodes in the neck), and edema.
Gastrointestinal anthrax has a high rate of mortality even though it is curable if caught early. This can be attributed to the non-specific symptoms, which resemble those of a severe case of influenza (Spencer 2003).
Inhalation Anthrax
Resulting from the inhalation of B. anthracis spores, inhalation anthrax (also called respiratory anthrax) is mainly associated with industrial exposure in the textile or tanning industries. The onset of symptoms usually occurs two to five days post-exposure. These symptoms are usually non-specific and “flu-like” (mild fever, fatigue, mild cough, etc.). This stage of the infection lasts about two days abruptly ends with the onset of acute symptoms including trouble breathing, fever, rapid breathing, tachycardia, cyanosis, and pleural effusion. These symptoms continue to worsen until they eventually lead to coma and death. Meningitis, or swelling of the membranes surrounding the brain and spinal cord, also occurs in about 50% of patients who contract this form of the disease (Spencer 2003).
Diagnosis
Clinical diagnosis of anthrax is performed by first culturing the skin lesion, blood, or cerebrospinal fluid and Gram staining the culture. The disease is indicated by the visualization of large Gram-positive bacilli forming short chains (Spencer 2003).
Anthrax Toxin Neutralization with Antibody
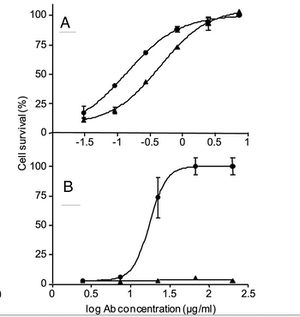
During infection by B. anthracis, protective antigen is integral in the intoxication of the host cells by anthrax toxins. This protein, therefore, is a logical target for scientists seeking to neutralize the anthrax toxins. Mechaly, et al. have recently found that the antibody cAb29, does just that: it targets PA molecules, interfering with the function of the molecule and thereby neutralizing the anthrax toxin (Mechaly 2012).
The Mechaly group, in attempting to determine the mechanism by which cAb29 functions to neutralize the toxins, found that cAb29 does not have any effect on the initial steps of the intoxication process: PA molecules are still able to bind to the target cell via receptors on the target cell membrane. These molecules are still cleaved by the furin-family protease and they still oligomerize into hepatomers which bind EF and LF molecules. Instead, they discovered that the antibody binds to the prepore, which is the complex of PA and either LF or EF before it is internalized by the cell, preventing the acid catalyzed transition to the transmembranal pore (Mechaly 2012).
Their tests showed 100% survival of mice injected intravenously with cAb29 12 hours after initial exposure to B. anthracis (Figure 3). This is a very important discovery as it could possibly lead to a cure for the disease even if it is not caught in the very early stages of infection (Mechaly 2012).
Target Cells in Humans in Inhalation Anthrax
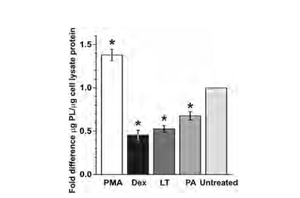
Until recently, scientists believed that alveolar macrophages were the target cells for inhaled B. anthracis spores in humans because the disease had been previously shown to inhibit mouse alveolar macrophages. However, more recent studies have determined that human alveolar macrophages do not express the anthrax toxin receptor protein and are therefore are unaffected by anthrax toxins because PA molecules are unable to bind to the cells. In their 2012 paper, Langer et al. explain how they determined what cells are actually the target of anthrax toxin is in humans. The results that they obtained show that human alveolar epithelial cells (AECs) express the anthrax toxin receptor, and they are, therefore, the target cell in the human respiratory system (Langer 2012).
The experiment which they conducted revealed that AECs in human lungs express the ATR protein, allowing PA molecules to bind to those cells and transport lethal toxin into the cytosol of the cells. Also, once infected, these cells exhibit reduced barrier function, junction formation, and surfactant production. This reduced surfactant production is illustrated in Figure 2. These symptoms are all signs of acute lung injury caused by the anthrax toxin. The team suspected that these changes in the AECs allow for greater dissemination of B. anthracis from the lungs into the blood in the early stages of infection, and in later stages of infection, they cause severe edema in the pulmonary tissue (Langer 2012).
References
Spencer, R. C. (2003). "Bacillus anthracis". "Journal of Clinical Pathology", 56(3), 182-187.
Edited by student of Joan Slonczewski for BIOL 238 Microbiology, 2013, Kenyon College.