Bacteroides Influence on Host Behavior
Introduction
Bacteria often live in a special mutualism with large multicellular organisms: in such relationships, both the host and its bacterial inhabitant perform some process that benefits the other. One such relationship of particular interest is that of the human digestive system and its "gut flora", or the microbial life that colonizes it. We provide an environment rich in nutrients and relatively stable environmental conditions (at least in terms of temperature and pH level), and our gut flora reciprocate by metabolizing substrates that our own digestive system has not evolved to break down. Humans do not have the ability to catabolize a significant amount of the substrates we consume, we simply lack the enzymes and other tools necessary to execute certain metabolic pathways. The reason we are still able to derive energy from these substrates is that the extensive community of microbes living in the human digestive tract metabolizes these molecules for us. An ancient mutualism between host organisms and the bacteria that colonize them has relieved humans of the need to develop such pathways. The microbia is composed of approximately 1013 organisms that fall into somewhere between 500 and 1,000 distinct species of bacteria [1]. This is not an insignificant statistic: there are more microbial organisms present in the human gut than the sum total of all of our somatic and gametic cells [2]; they are often considered to compose a functional organ of the human body. The species that compose this "organ" represent every branch of life—eukaryotes, bacteria, and even some archaea—but by far the most populous inhabitants are the bacteria.
This community of microorganisms reaches the highest population density of any form of life in any ecosystem anywhere on the planet [4]. Interestingly enough, this high population density is not reflected by a high species diversity: the digestive system is home to relatively few species, which are dominated by the genera Bacteroides and Firmicutes—when combined, these two compose over 90% of all the phylogenetic types present [2]. In ecosystems with high species diversity equilibrium is maintained because a broad range of species with a broad range of functions will be able to fill a diverse set of niches. As the boom-bust pattern of bacterial growth cycles due to availability of substrate, predation, and a variety of other factors, new species are able to fill the voids left by species that have "busted". The ecosystem of the human gut, however, does not have a range of species with a range of functions. Rather, equilibrium is maintained because each individual species can fill a broad spectrum of functions [2]. A major factor that contributes to the stability of the digestive tract ecosystem is that the microbes of the intestine are able to induce changes in the host to bring their environment into equilibrium. The most extensively studied species in this area is a keystone member of the gut flora: Bacteroides thetaiotaomicron.
It is fairly intuitive that in such a relationship the host will dictate temperature, pH level, substrate availability, and a variety of other environmental factors that will determine what types of bacteria are able to colonize it, how these bacteria will behave, and how successful any given species will be in that environment. That is to say, the host has a substantial influence over its microbia. What is not always such an intuitive aspect of the host/bacteria relationship is the influence that bacteria may have over the behavior and characteristics of the host. Research on the effect of bacteria on a host has traditionally been focused on combating pathogenic bacteria, only recently turning to the manipulation of tissues by indigenous bacteria. Two important topics in this field are: the role of gut flora as a cause of obesity, and as anti-pathogen agents.
The rise in obesity in the western world over the past several decades has prompted researchers to explore possible explanations for such a drastic shift in human physiology. An important determinant of the physiology of an individual is the unique genome of that individual; and while this may account for a natural tendency towards weight gain for certain genotypes, the human genome has certainly not undergone a radical transformation since the "obesity epidemic" hit the western world. If we look at what has changed in the past few decades, we see people consuming larger-portioned, higer-calorie diets. But how and why does this shift in diet translate to a shift in body composition? Scientists are now looking at the role of the microbia as a factor in the rise in obesity.
A closer look at Bacteroides thetaiotaomicron
B. thetaiotaomicron (B. thet) is a bacteria in the class Bacteroides, which is a gram-negative, rod-shaped bacteria. It resides in the human/mammalian cecum where it ferments polysaccharides from plant fibers using anaerobic respiration. The substrates catalyzed by bacteroides cannot be broken down by host enzymes, but once fermented by bacteriodes can be used and/or stored as energy by the host. It is estimated that up to 15% of the caloric value humans obtain from food is made available to us by bacteriodes [2], making organisms in this class key players to consider when examining the pathway from diet to fat storage. Bacteroides' vital role in energy processes has prompted researchers to explore the role that it and other bacteria may be playing in the rise in obesity.
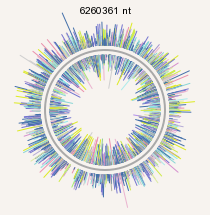
In the human microbiota B. thetaiotaomicron is the most abundant species, it is a 'keystone' member of the gut ecosystem. B. thetaiotaomicron is the first abundant member of the human gut flora to have its entire genome sequenced (figure 1). Analysis of the genome revealed a massive proteome, with some 4,779 predicted proteins of which 24% have no homology to other known sequences, and 18% have homology to proteins with no known functions [6]. The large portion of proteins with no known homologs indicates a deep-branch in its lineage. The remaining 58% of proteins of known function offer insight into how this organism maintains its dominance in the ecosystem of the human gut. Dr. Xu posits that the success of B. thetaiotaomicron can largely be attributed to three factors: "(i) sensing its luminal environment, (ii) acquiring dietary polysaccharides, and (iii) manipulating host gene expression in ways that establish and maintain a mutually advantageous environment"[6]. B. thetaiotaomicron has the ability to derive energy from a broad range of sources, preferring food particles followed by shed elements of the mucus layer, and lastly exfoliated epithelial cells [2]. If a preferred food is not available to it , B. thetaiotaomicron will use host polysaccharides. It does this by manipulating the host genome; for example, it can promote host epithelial cell production of fucosylated glycans on which to feed.
To manipulate the host genome, B. thet uses a process involving quorum sensing and a variety of signaling factors to modify host biochemical pathways (figure 2). Miguel Freitas has outlined the steps of this process in his paper on indigenous bacteria and probiotics. The process begins with bacteria-bacteria communication. In the gut, bacteria fill very specific niches, the ecosystem is organized both laterally and radially, with different species thriving at different levels [9]. In addition, there are both innate organisms and organisms that are not native to the region of the gut that they may be found in at any given time. By using quorum sensing, organisms are able to detect where they are in the gut and what other bacteria are surrounding them. Based on this signaling, bacteria will release compounds that are directly active on the epithelial cell surface of the host gut lumen. Some of these interactions require direct contact, either through enzymes or lippopolysaccharides. The factors that mediate changes in the host cells are referred to as 'modulins'; they are able to modify some host cell biochemical processes such as glycosilation patterns of the host cell surface. These modifications can have an effect both on the bacteria and on the host cell [10].
A Regulatory Pathway of B. thetaiotaomicron Pertaining to the Immune System
The pathway of bacterial host modification has been observed in experiments on mice: one such pathway involves the presence of surface proteins on the host gut. The cells lining the gut have various surface proteins that serve a wide range of processes, from cell-cell communication to food absorption. The host is not born with all of these proteins present, some of them appear as the gut matures, and some appear only under certain environmental conditions. A good example of this is the dependence of the presence of leptin protein Ulex europaeas agglutinin (UEA-1) on B. thetaiotaomicron. UEA-1 is a protein that recognizes carbohydrates found on pathogens; specifically, it is a substance capable of causing the clumping of a particular antigen, thus it is a player in the host immune system. Mice generally begin to develop UEA-1 between 17 and 21 days after birth, and by 28 days, it is generally fully present (hooper). The development of this protein turns out to be regulated by B. thetaiotaomicron.
An experiment presented by Lora Hooper and colleagues examined epithelial differentiation of the gut in both the presence and absence of B. thetaiotaomicron. In this experiment, two groups of mice were raised one group in a gnotobiotic environment (GF), and the other under normal circumstances. When the mice were between 17 and 21 days old, each group began to show patterns of expression of the UEA-1 leptin; however, by 28 days the protein had disappeared in the GF mice while in the conventionally raised mice it proliferated to the entire ilium. This indicated that the presence of a normal microbiota was required to sustain and increase the expression of UEA-1. The next step in the experiment was to inoculate GF mice with B. thetaiotaomicron. Inoculation reinitiated the natural pattern of gut maturation. Basically, whenever and for however long B. thetaiotaomicron was present in the gut, normal expression of UEA-1 occurred.
Hooper suggests that the B. thetaiotaomicron manipulates the host either by secreting a soluble microbial factor, or by density depended metabolism/signal generation. The results indicate that in order to have a complete and functional immune system, a healthy microbiota must be present. Hooper believes that "By introducing one or two genetically manipulatable members of the normal gut flora into developing or adult germfree mice, it should be possible to identify signaling molecules that are exchanged between symbiont and host, as well as the bacteria themselves, during establishment of their functional associations". This research would give us a more specific and more clear picture of the pathways used by bacteria to influence their hosts. This particular pathway is a good example of human/bacteria mutualism: protection against pathogens will benefit both the host and its bacteria.
Bacterial Involvement in Obesity
As we learn more about host/bacteria mutualism, we are becoming more aware that there are factors dictated by the bacterial community living in a host that have a profound impact on the host. The rise in obesity in the western world has prompted researchers to look for connections between gut flora and host phenotype.
To explore the hypothesis that microbiota play a significant role in body composition—particularly fat content—a team of scientists led by Fredrik Bäckhed and Hao Ding designed and executed several experiments on mice. The overall hypothesis of their experiment was that "microbiota act through an integrated host signaling pathway to regulate energy storage in the host" [1]. To test their hypothesis, the researchers raised two groups of mice: one group was normal (CONV-R), and the other consisted of genetically engineered gnotobiotic mice (GF). A group of the GF mice were exposed to microbiota isolated from the CONV-R group. The exposed group was renamed CONV-D and were allowed to grow for 10-28 days after exposure. When the CONV-D mice were compared with the CONV-R and GF groups, they showed a substantial increase in total body fat content (the CONV-D had 57% more than the GF), and epididymal fat weight (up 61% in CONV-D), but had a 7% decrease in lean body mass. In addition to comparing the CONV-D and GF mice, the researchers also looked at the CONV-R and GF mice. In this case as well they found that the mice with a healthy microbiota had a higher body fat content (though not as high as the CONV-D group) than the germ-free mice. These results showed a direct and meaningful correlation between the presence of intestinal bacteria and body composition: when bacteria are present in the digestive tract, it is more efficient in converting and storing energy in the host.
The results from this experiment show us that bacteria are an important factor in the process of converting and storing food as energy, but they do not indicate the mechanism by which they operate. To investigate this pathway, several experiments were set up using mice with knock-out mutations to trace the signal pathways that dictate an increase in body fat when bacteria are present. There is a hormone in mice (and humans) called leptin that is expressed in correlation with the lipid content of adipocytes (tissue cells that store fat). It has been shown that when a mouse experiences an increase in leptin, it will be inclined to eat less and exercise more [8]. As the body fat of the CONV-D mice rose, levels of leptin in their bodies rose accordingly; however, so did fasting glucose and insulin levels.
In the liver, glucose and insulin trigger an increase in lipogenic enzymes. In the study, PCR assays confirmed an increase in mRNA's coding for acetyl-CoA carboxylase (Acc1), and fatty acid synthase (Fas); both enzymes are important in forming new fatty acid biosynthetic pathways. Mice with a microbiota showed increase levels of a protein called xylulose-5-phosphate (Xu5P), which essentially begins a cascade of protein activation resulting in increased levels of Acc1 and Fas. Monosaccharide uptake by epithelial cells was also found to increase in the presence of microbiota. The increase of lipogenesis proteins and monosaccharide transfer to the liver are both directly correlated to the presence of microbiota. The both put stress on the liver, which must find something to do with the extra energy it is receiving. It has essentially two options: it can reduce the efficiency of the host's metabolism by inducing futile cycles, or it can export extra calories to be stored in the peripheral tissue.
Another signaling pathway that these experiments showed the gut flora to play a part in is the promotion of storage of triglycerides. In this pathway, a protein called Fasting-induced adipocyte factor (Fiaf) inhibits lipoprotein lipase (LPL). LPL normally releases fatty acids from certain tissues, thus signaling the body to increase uptake of fatty acids. The presence of gut microbiota suppress Fiaf in the gut epithelium, resulting in an increase in LPL, and accordingly, an increase in fatty acid uptake (figure 4).
Conclusion
The recent shift in research to examining the interactions of host and their microbial colonizers has opened up a new and exciting field with important medical implications. This research is changing the way we understand the human body and its processes. The human gut and its microbiota work in an important partnership, each benefiting the other; we are only begining to understand the extent to which we are connected to our gut flora.
References
1. Backhed, F., Ding, H., Wang, T., Hooper, L., Koh, G.Y., Nagy, A., Semenkovich, C.F., Gordon, J.I. "The gut microbiota as an environmental factor that regulates fat storage". Science. 2004. Volume 101(44). p. 15718-15723.
2. Backhed, F., Ley, R.E., Sonnenburg, J.L., Peterson, D.A., Gordon, J.I. "Host-Bacterial Mutualism in the Human Intestine". Science. 2005. Volume 307. p. 1915-1920.
3. Ley, R.E., Turnbaugh, P.J., Klein, S., Gordon, J.I. "Microbial ecology: Human gut microbes associated with obesity". Nature. 2006. Volume 444. p. 1022-1023.
4. McCann, K.S. “The diversity-stability debate”. Nature. 2000. Vol. 405. p. 228]
5. Turnbaugh, P.J., Ley, R.E., Mahowald, M.A., Magrini, V., Mardis, E.R., Gordon, J.I. "An obesity-associated gut microbiome with increased capacity for energy harvest". Nature. 2006. Volume 444. p. 1027-131.]
6. Xu, J., Bjursell, M.K., Himrod, J., Deng, S., Carmichael, L.K., Chiang, H.C., Hooper, L.V., Gordon, J.I. "A Genomic View of the Human-Bacteroides thetaiotaomicron Symbiosis". Science 2003. Vol.299. p.2074-2076.
7. Ferretti, J.J., Gilmore, M.S. "The Thin Line Between Gut Commensal and Pathogen". Science. 2003. Volume 299. p. 1999-2002.
8. Pelleymounter, M.A., Cullen, M.J., Baker, M.B., Hecht, R., Winters, D., Boone, T., Collins, F. "Effects of the obese gene product on body weight regulation in ob/ob mice". Science. 1995. Volume 269. p. 475-6.
9. Hooper, L.V., Bry, L., Falk, P.G., Gordon, J.I. "Host-microbial symbiosis in the mammalian intestine: exploring an internal ecosystem". BioEssays. 1998. Vol. 20, p. 336-343.
10. Freitas, M., Tavan, E., Cayuela, C., Diop, L., Sapin, C., Trugnan, G. "Host-pathogens cross-talk. Indigenous bacteria and probiotics also play the game". Biology of the Cell. 2003. Vol. 95, p. 503-506.
Edited by student of Joan Slonczewski for BIOL 238 Microbiology, 2009, Kenyon College.