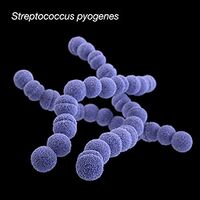
Change in the Pharyngeal Microbial Environment after a Tonsillectomy
Introduction
By Lindsey Abramson
The palatine tonsils are spheres of lymphoid tissue that sit in the back of the pharynx, or throat area, and play a huge role in the immune system due to their proximity to ingested or inhaled pathogens [2]. The immune cells on the tonsils (B and T cells) help to filter and destroy bacteria and viruses by producing antibodies [2]. Tonsillectomies, the surgical removal of the tonsils, are performed on individuals with recurrent tonsillitis infections, recurrent strep throat, enlarged tonsils, Sleep-Disordered Breathing, and other issues such as cancerous cells [3]. The goal of this radical procedure is the eradication of bacteria assuming antibiotics have been frequently used and failed or if antibiotic resistance was developed [4]. Streptococcus pyogenes (also called group A streptococci, or GAS) is the causative agent bacterium of strep throat, one of the leading causes that push individuals towards an elective tonsillectomy [5]. This procedure is cautioned against due to the high risks associated, including hemorrhage[6]. GAS is spread through aerosol droplets and can lead to more severe infections such as rheumatic fever [5][7]. Other problematic bacteria include: Staphylococcus aureus, Haemophilus influenzae, Streptococcus pneumoniae, Escherichia coli, and Pseudomonas aeruginosa, although viruses are also common [4]. Bacteria such as Staphylococcus aureus and GAS can produce biofilms on the tonsils and can cause antibiotic resistance in the pharynx and make recurrent strep throat tonsillitis possible [4]. Research on the differences between the pre and post tonsillectomy microbial environments has scarcely been a focus, however, the limited current literature finds that the removal of infected tonsils has a positive effect on the microbial environment of the throat, decreasing levels of pathogenic bacteria such as GAS and increasing the normal flora found in the throat [3]. This wiki page will dive into GAS, the tonsillectomy procedure, as well as the pharyngeal microbial environment before and after tonsil removal.
Streptococcus pyogenes

Streptococcus pyogenes (group A streptococci, or GAS), a gram-positive bacteria, is the causative agent of strep throat and tonsillitis [5][7]. GAS falls under the classification of Firmicutes (Bacillota, “tough skin”) and contains a very thick cell wall containing 10-20 layers of peptidoglycan [5]. GAS is a worldwide public health concern due to its virulence and ability to lead to more severe infections [5][7]. Such infections like rheumatic fever can occur due to repeated GAS infections [7]. Rheumatic fever occurs after a throat infection when the M surface protein on GAS binds to a B-cell receptor on the heart and is taken up by mistake due to its resemblance to heart antigens (“cardiac-like epitope” on the M protein) [5]. GAS spreads by aerosol droplets through close or direct human to human contact [7]. The effective adhesion and attachment of GAS allow the bacteria to form micro colonies and biofilms [7]. It is hypothesized the GAS attaches through a two step process where there is first a longer range hydrophobic interaction that mediates pili attachment followed by a more specific high affinity binding [7]. Biofilms are colonies of adjacent bacteria that stick to one another and attach to a surface. The biofilm formation abilities of GAS have not been extensively studied, however, it has become apparent that the pathogenesis of the biofilm may lead to recurrent infection [7]. GAS biofilm formation is regulated by a complex process including transcriptional regulation in response to environmental conditions such as temperature, PH, and oxygen presence [7]. Recent research has looked into the possibility of creating a vaccine that would inhibit either the adhesion of GAS or the biofilm formation in order to reduce the rates of tonsillitis, strep throat, and other more severe infections caused by GAS [7].
GAS is the most common bacterial cause of a sore throat (15-30% of cases in children and 5-10% of cases in adults) even though it is a common commensal bacterial in the pharyngeal flora [8]. This bacteria can be found in the palatine tonsils, adenoids, uvula, soft palate, and other lymphoid tissue [8]. This area in the throat is referred to as “Waldeyer’s ring” which includes the adenoid, lingual, and palatine tonsils [8]. Waldeyer’s ring includes the “nasal-associated lymphoid tissue”[9]. The tonsils are the first site of encounter for pathogens after inhalation or ingestion and therefore the first line of defense [9]. The B cells in the tonsils are what allows the organ to fight infection [9]. Although they might put up a good fight, the tonsils are susceptible to infection due to the crypts (folds that form in response to infection) as compared to the pharynx which has a smoother surface that is filled with saliva [8]. A sore throat will present with soreness or pain when swallowing and inflammation due to the response to pathogens in the throat [8]. The glossopharyngeal nerves are the direct cause of pain [8].
What is a Tonsillectomy?
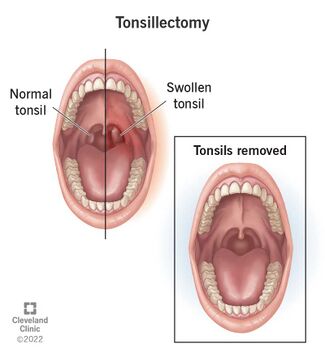
A tonsillectomy is the surgical removal of the palatine tonsils which is performed as a last resort invasive effort to fight recurrent tonsillitis infection, cancer, and other issues that cannot be solved via antibiotics or the normal functions of the immune system [3]. Healthy tonsils normally play an important role in the immune system by filtering and destroying bacteria and viruses by the production of antibodies[2]. The tonsils grow to a peak size around ages four to eight as this is the peak immune activity of this tissue due to the high exposure rate to new pathogens from children [8]. Tonsillectomies previously were the most popular procedure used to combat respiratory disease, however, now the prevalence of such procedures has decreased to less than one half of the number from 40 years ago [11]. The history of tonsillectomies dates back to the first century when Cornelius Celsus in Rome was described as removing infected tonsils with his fingers [12]. Between 1500-1600, the practice of removal included using string, strangulation, and force [12]. The early stages of this procedure did not use anesthesia and therefore the goal of the procedure was to complete the removal as quickly as possible [12]. Since that time period, the procedure has drastically evolved, but the basic idea of the surgery has not changed [12]. Currently, the 20-30 minute procedure includes the use of general anesthesia, and the severing of the mucous membrane by electrocautery, cold-knife cutting, or snare pulling, and then more electrocautery or sutures to stop the bleeding [12]. Due to the extremely high risk factors and complications that are associated with this procedure, it is only recommended if certain requirements are met.
The Mayo Clinic defines its criteria for surgery as the following:
-seven episodes of tonsillitis in a single year, or
-five episodes of tonsillitis in each of two consecutive years, or
-three episodes of tonsillitis in each of three consecutive years [11].
After the procedure, painful swallowing and a sore incision site is to be expected. Dehydration, weight loss, and nausea are big concerns due to the pain that accompanies swallowing [11]. The greatest concern comes from the risk of hemorrhage, which can arise at any moment after surgery when the scabs covering the incision site start to flake off [11]. Post tonsillectomy hemorrhage, which varies in risk from 0.28%-20%, is always considered an emergency and requires immediate attention and likely surgical intervention [6]. Individuals over the age of twelve are at greater risk for complications and higher levels of pain, due to the buildup of scar tissue on the tonsils themselves and an overall larger surface area [6]. Therefore, some doctors do not recommend this procedure for adults unless absolutely necessary. Furthermore, there are mixed opinions from pediatricians and ENT’s in regard to the role of tonsils in the body and long-term effects on the immune system after a tonsillectomy [13]. For these reasons, careful consideration needs to be given when deciding whether a tonsillectomy is necessary.
Pre-Tonsillectomy Microbial Environment

A normal or "healthy" pharyngeal environment, or more specifically, a oropharyngeal environment, consists of both “aerobic and anaerobic bacteria such as α-hemolytic and nonhemolytic streptococci, coagulase negative staphylococci, Neisseria, Flavescens, Corynebacterium, Actinomyces, Leptotrichiae, and Fusobacterium species” [16]. The epithelium (thin outer tissue that covers all organs and blood vessels) of the paired palatine tonsils contains both “T cells and immunoglobulin-expressing B cells” in all regions due to their random distribution [17]. These lymphocytes, especially B cells, play an important role in healthy tonsils by producing antibodies that filter and destroy bacteria [17].
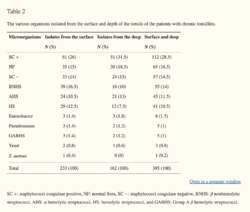
It should be first noted that the bacteria that causes tonsillitis can inhibit both the surface of the tonsil as well as deeper tissue[16]. This can cause issues when the prescribed antibiotics only target surface bacteria[16]. Therefore both the surface and deep tissue bacteria cultures need to be considered when analyzing the difference in microbial environments. Although tonsillectomies treat recurrent tonsillitis due to bacterial infection, it is also important to recognize that they treat Sleep-Disordered Breathing (SDB) as well, which stems from many causes, including large tonsils[14].One specific studyanalyzed the tonsils of patients who were receiving a tonsillectomy due to recurrent tonsillitis. Both surface level and deep level samples were collected to quantify the various types of bacteria found during the time of the procedure on the infected tonsils. The majority of bacteria found on the surface were the same as what was found within the tissue [14]. The most common isolated bacterial pathogens include: staphylococci coagulase positive and by β non-hemolytic streptococci [14]. As stated above, group A streptococci is the most common pathogenic bacterial cause of strep throat and is found in 15-36% of children who present with a sore throat [7][18]. The recommended antibiotics to treat GAS include “penicillin, amoxicillin, erythromycin, and first-generation cephalosporins” [18]. The CDC recommends penicillin as the number one treatment option for those who have the minimum amount of GAS bacteria present to require antibiotics [18]. They also urge physicians to make sure they are completing a GAS throat culture prior to prescribing antibiotics in order to limit the amount of antibiotic resistance present among younger individuals [18].
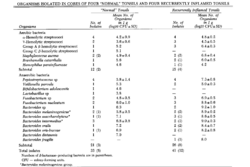
Many studies have found the presence of β-lactamase producing bacteria in the core of GAS infected tonsils that were surgically removed due to recurrent strep throat [15]. An older study investigated the quality and microbial environment of “healthy” tonsils that were removed for various other reasons and infected tonsils. They found that the number of bacteria on the infected tonsils were anywhere between 100-1000 times greater [15]. Significant differences in bacteria levels were noted between “β-hemolytic streptococci, all Bacteroides spp, and all Peptostreptococcus spp” [15]. Furthermore, β-lactamase production was found in five isolates from the healthy tonsils and twelve isolates from the infected tonsils [15]. The second figure on the right is taken from Brook and Foote (1990), and summarizes all of the organisms found in “normal” tonsils versus recurrently inflamed tonsils. The “normal” and infected tonsils did contain the same or similar organisms, however, the concentrations of the streptococci and staphylococci and most of the anaerobic bacteria were much higher in the recently inflamed tonsils [15]. Recovering the same species of bacteria from both tonsil groups provides support for the theory that allows for non encapsulated organisms to transform into encapsulated organisms during the inflammatory process [15]. Encapsulation has been recognized as an important virulence factor that impacts the inflammation of the tonsils [15].
Post-Tonsillectomy Microbial Environment
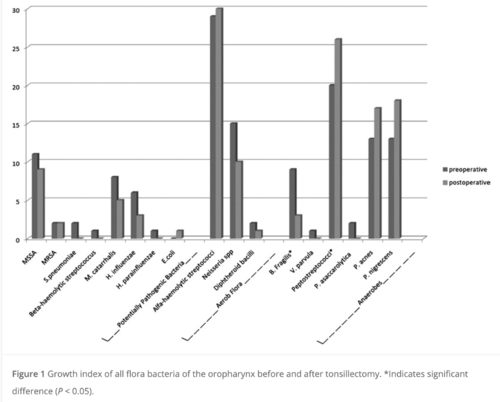
Karaman et al., investigated the effect of tonsillectomy on the oropharyngeal flora in children. Throat swabs were collected from 31 individuals prone to recurrent tonsillitis prior to the operation as well as one month post-tonsillectomy [19]. There was surprisingly no significant difference in the pre and post operative prevalence of aerobic pathogenic oropharyngeal bacteria [19]. The Neisseria species (part of the normal bacterial flora) did decline but not significantly, whereas the anaerobic bacteria, B fragilis did significantly decrease [19]. This could suggest that the bacteria flora may revert back to what is expected from a “healthy” individual, as increased anaerobic bacteria can be a potential risk for upper respiratory infection [19]. A meta-analysis and systematic review paper investigated the current scientific literature results surrounding pathogenic bacteria changes after a tonsillectomy. They reported decreases in multiple pathogenic bacteria post tonsillectomy including GAS and reported increases in non-pathogenic respiratory flora, once again suggesting that the flora may revert to a more healthy state [3]. Besides GAS, other statistically significant decreases in bacteria post operation include Haemophilus influenzae and Streptococcus pneumoniae[3]. This meta-analysis implied that the removal of infected tonsils has a positive effect on the microbial environment of the throat [3]. As stated in this paper, results and data on the outcomes in reference to the change in microbial environment is scarce and require future studies[3].
Alho et al., conducted a randomized experiment on adults to determine the effectiveness of tonsillectomy while determining the amount of GAS present. There is still some skepticism surrounding the removal of the palatine tonsils because infection by GAS also occurs in “other pharyngeal lymphoid and soft tissues”, therefore Alho et al., proposed a study to gather more conclusive evidence [20]. 70 individuals who met the criteria for a tonsillectomy were assigned to two groups, an experimental group undergoing a tonsillectomy and a control group placed on a waiting list for a tonsillectomy [20]. Throat cultures were taken 90 days post tonsillectomy or non-tonsillectomy to determine the presence of GAS as well as the proportion of individuals that presented positive for GAS pharyngitis (inflammation of the throat caused by bacteria or virus that leads to pain) [20]. After 90 days, the study found that a significant proportion of the control group had experienced acute episodes of pharyngitis compared to the group that underwent tonsillectomy [20]. Rates of infection along with throat pain and fever were significantly reduced in the experimental group compared to the control group [20]. At the 90 day mark, “streptococcal pharyngitis had recurred in 24% (8/34) in the control group and 3% (1/36) in the tonsillectomy group (difference 21%) [20]. Therefore, this study concluded that adults who experience recurrent GAS pharyngitis were less likely to experience future GAS related infection and pain if they had their tonsils removed [20].
Another study analyzed the immune systems of 34 children after a range of 4-6 years following a tonsillectomy. Levels of the antibodies IgG, IgM, and IgA were quantified from blood samples and found to be significantly lower in individuals who underwent a tonsillectomy as compared to those who did not [13]. Having reduced levels of these antibodies could make an individual more susceptible to infection which then calls into question the risks associated with a tonsillectomy [13].
Success Rates
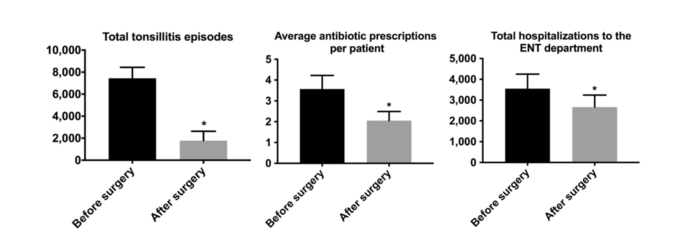
Taking a more broad approach to determine the effectiveness of tonsillectomies, long-term outcomes can be analyzed by looking at the number and severity of tonsillitis episodes, antibiotic use, and hospitalizations after the procedure. Tzelnick et al., analyzed 3,701 adult patients (mean age = 37.4) who underwent a tonsillectomy and their lives following the procedure for up to three years after via a retrospective chart review. Following the removal of tonsils, there was a significant decrease in the number of tonsillectomy episodes, consumption of antibiotics, visits to the ear, nose, and throat doctor, hospital visits and respiratory infection diagnosis [21]. “Patients with recurrent tonsillitis who underwent tonsillectomy had a 75% decrease in the total number of tonsillitis episodes and a 57% decrease in the consumption of pertinent antibiotics due to tonsillitis events” [21]. These statistics show significant success rates in health following the removal of the tonsils for adults in this study.
Another study looking at pre and post operation statistics with a smaller sample size found similar results. This study differed in the time frame that was analyzed post-operatively, as patients were consulted seven years following the operation. Prior to getting the tonsils surgically removed, the mean number of sore throats / tonsillitis episodes was ten per year (median = 6) for this study [22]. After surgery, the mean number dropped to just two (median = 1), which was a significant difference [22]. Furthermore, the yearly use of antibiotics for a sore throat decreased from four times a year to two and a half times a year [22]. This demonstrates the improved quality of life that a tonsillectomy can provide for individuals who suffer from recurrent tonsillitis, including overall health as well as economic value (decrease in the number of medications used, trips to the doctor, and days out of work due to illness) [22].
A UK based study also analyzed a smaller sample size of individuals with varying age ranges. They found that the number of days off from work or school due to a sore throat was reduced by 95.3% after a tonsillectomy [23]. Furthermore, visits to their general practitioner due to a sore throat was reduced by 95.6% and more than 93% of patients reported a significant increase in their well being, general health and energy level [23]. Among patients who suffer from recurrent, chronic, or acute tonsillitis, a tonsillectomy is a cost-effective treatment that may provide a more positive and healthy lifestyle [23].
Conclusion
The surgical removal of the palatine tonsils will likely continue to be a standard elective procedure for improving the quality of life and health of individuals with recurrent tonsillitis [3][20][21][22][23]. The drastic decreases in tonsillitis / strep throat episodes, hospital visits, and prescribed antibiotics following a tonsillectomy are incentive enough to remove the tonsils, not to mention the economic benefit that follows due to these reasons [21][22][23]. Further, the limited published data finds that there is a reduction in pathogenic bacteria such as GAS, and a push towards a healthier microbial environment in the throat following the removal of the tonsils [3][19][20]. This procedure seems to be a very effective solution in boosting the immune system when the tonsils are not doing their designated job as the first line of defense against ingested or inhaled pathogens [9]. However, due to the complications and long, painful recovery process that follows this procedure, physicians should continue to proceed with caution in performing this surgery, especially in adult patients who are at higher risk [11]. With the evolution of the medical field, hopefully the techniques, tools, and machines used will only aid in providing the best outcome for patients. More scientific literature needs to be published on the topic of the effects of tonsillectomies on microbial environments and the impact it has on the body's ability to fight off infection. Although this is a limitation of human medicine, as it is of course difficult to compare bacterial environments on human subjects. Future research should also focus on understanding the adhesion and biofilm formation of GAS in the hopes of creating a vaccine protecting individuals against strep throat and pharyngeal infection [7].
References
- ↑ Streptococcus laboratory: Streptococcus pyogenes | CDC. (2021, July 23). Centers for Disease Control and Prevention.
- ↑ 2.0 2.1 2.2 Masters KG, Zezoff D, Lasrado S. Anatomy, Head and Neck, Tonsils. 2023. StatPearls Publishing.
- ↑ 3.0 3.1 3.2 3.3 3.4 3.5 3.6 3.7 3.8 Brietzke, S.E. and Andreoli, S.M., 2021. Systematic review and meta-analysis of the change in pharyngeal bacterial cultures after pediatric tonsillectomy. Otolaryngology–Head and Neck Surgery, 164(2), pp.264-270.
- ↑ 4.0 4.1 4.2 Yildizoglu, U., Polat, B., Gumral, R., Kilic, A., Tosun, F. and Gerek, M., 2015. Effect of antibiotic use on bacterial flora of tonsil core in patients with recurrent tonsillitis. European Archives of Oto-Rhino-Laryngology, 272, pp.1525-1528.
- ↑ 5.0 5.1 5.2 5.3 5.4 5.5 Slonczewski, S.L, Foster, J.W, and Zinser, E, 2024. Microbiology an evolving science, sixth edition. W.W. Norton and Company.
- ↑ 6.0 6.1 6.2 Liu, J.H., Anderson, K.E., Willging, J.P., Myer III, C.M., Shott, S.R., Bratcher, G.O. and Cotton, R.T., 2001. Posttonsillectomy hemorrhage: what is it and what should be recorded?. Archives of Otolaryngology–Head & Neck Surgery, 127(10), pp.1271-1275.
- ↑ 7.00 7.01 7.02 7.03 7.04 7.05 7.06 7.07 7.08 7.09 7.10 7.11 7.12 Brouwer, S., Barnett, T.C., Rivera‐Hernandez, T., Rohde, M. and Walker, M.J., 2016. Streptococcus pyogenes adhesion and colonization. FEBS letters, 590(21), pp.3739-3757.
- ↑ 8.0 8.1 8.2 8.3 8.4 8.5 8.6 Bathala, S. and Eccles, R., 2013. A review on the mechanism of sore throat in tonsillitis. The Journal of Laryngology & Otology, 127(3), pp.227-232.
- ↑ 9.0 9.1 9.2 9.3 Hellings, P., Jorissen, M. and Ceuppens, J.L., 2000. The Waldeyer's ring. Acta oto-rhino-laryngologica belgica, 54(3), pp.237-241.
- ↑ Tonsillectomy: Procedure details and recovery. (2022, October 17). Cleveland Clinic.
- ↑ 11.0 11.1 11.2 11.3 11.4 Stuck, B.A., Windfuhr, J.P., Genzwürker, H., Schroten, H., Tenenbaum, T. and Götte, K., 2008. Tonsillectomy in children. Deutsches Ärzteblatt International, 105(49), p.852.
- ↑ 12.0 12.1 12.2 12.3 12.4 Younis, R.T. and Lazar, R.H., 2002. History and current practice of tonsillectomy. The Laryngoscope, 112(S100), pp.3-5.
- ↑ 13.0 13.1 13.2 Radman, M., Ferdousi, A., Khorramdelazad, H. and Jalali, P., 2020. Long-term impacts of tonsillectomy on children's immune functions. Journal of Family Medicine and Primary Care, 9(3), pp.1483-1487
- ↑ 14.0 14.1 14.2 14.3 Shishegar, M. and Ashraf, M.J., 2014. Posttonsillectomy bacteremia and comparison of tonsillar surface and deep culture. Advances in preventive medicine, 2014.
- ↑ 15.0 15.1 15.2 15.3 15.4 15.5 15.6 15.7 Brook, I. and Foote Jr, P.A., 1990. Microbiology of “normal” tonsils. Annals of Otology, Rhinology & Laryngology, 99(12), pp.980-983.
- ↑ 16.0 16.1 16.2 Gul, M., Okur, E., Ciragil, P., Yildirim, I., Aral, M. and Kilic, M.A., 2007. The comparison of tonsillar surface and core cultures in recurrent tonsillitis. American journal of otolaryngology, 28(3), pp.173-176.
- ↑ 17.0 17.1 Nave, H., Gebert, A. and Pabst, R., 2001. Morphology and immunology of the human palatine tonsil. Anatomy and embryology, 204(5), pp.367-373.
- ↑ 18.0 18.1 18.2 18.3 Linder, J.A., Bates, D.W., Lee, G.M. and Finkelstein, J.A., 2005. Antibiotic treatment of children with sore throat. Jama, 294(18), pp.2315-2322.
- ↑ 19.0 19.1 19.2 19.3 19.4 19.5 Karaman, E., Enver, O., Alimoglu, Y., Gonullu, N., Bahar, H., Torun, M.M. and Isildak, H., 2009. Oropharyngeal flora changes after tonsillectomy. Otolaryngology--Head and Neck Surgery, 141(5), pp.609-613.
- ↑ 20.0 20.1 20.2 20.3 20.4 20.5 20.6 20.7 20.8 Alho, O.P., Koivunen, P., Penna, T., Teppo, H., Koskela, M. and Luotonen, J., 2007. Tonsillectomy versus watchful waiting in recurrent streptococcal pharyngitis in adults: randomised controlled trial. BMJ, 334(7600), p.939.
- ↑ 21.0 21.1 21.2 21.3 21.4 Tzelnick, S., Hilly, O., Vinker, S., Bachar, G. and Mizrachi, A., 2020. Long‐term outcomes of tonsillectomy for recurrent tonsillitis in adults. The Laryngoscope, 130(2), pp.328-331.
- ↑ 22.0 22.1 22.2 22.3 22.4 22.5 Senska, G., Atay, H., Pütter, C. and Dost, P., 2015. Long-term results from tonsillectomy in adults. Deutsches Ärzteblatt International, 112(50), p.849.
- ↑ 23.0 23.1 23.2 23.3 23.4 Akgun, D., Seymour, F.K., Qayyum, A., Crystal, R. and Frosh, A., 2009. Assessment of clinical improvement and quality of life before and after tonsillectomy. The Journal of Laryngology & Otology, 123(2), pp.199-202.
Authored for BIOL 238 Microbiology, taught by Joan Slonczewski,at Kenyon College,2024