Ebola virus (EBOV)
Introduction
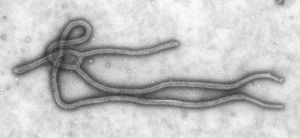
Ebola virus (EBOV) is a member of the Filoviridae virus family along with Marburg virus (MARV). Together they are commonly known as filoviruses. EBOV is a virulent pathogen that causes fatal hemorraghic fever in humans and nonhuman primates (Hartlieb et al.2005). A large majority of patients infected with EBOV, and who are not properly treated, fall ill within 2-20 days after exposure, with 50-90% death rate (WHO media centre). There has been greater than 2,300 reported cases of hemmorraghic fever caused by filoviruses, EBOV and MARV (Yermolina et al.2010). The actual number of cases is expected to be even higher as it is suspected that many cases go unreported in rural African villages. The EBOV virus has infected many parts of the world, but the majority of the infectious outbreaks occur in central Africa (Geisbert et al.2010). Not only has this viral pathogen affected human populations, but it has also aided in the decline of western gorilla populations near central Africa (Yermolina et al.2010).
The genome of this fatal pathogen possesses a linear non segmented, single negative-stranded RNA (Figure 1). The genome codes for seven structural proteins, which include: nucleoprotein (NP), VP35, VP40, glycoprotein (GP), VP30, VP24, and L protein, which provides RNA-dependent RNA activity enclosed in an envelope (Leroy et al.2000). These structural proteins are the primary target sites of vaccines in many current studies as they are vital sites for silencing EBOV outbreaks. There are currently five species of the infectious virus that differ from each other by 37-41% based on their amino acid and nucleotide sequencing (Jones et al.2005). This fluctuation in amino acid and nucleotide sequencing leads to a large problem in finding a cure as vaccinations, for one species does not guarantee vaccination for any other species. The five species of EBOV include: Zaire ebolavirus (ZEBOV), Sudan ebolavirus (SEBOV), Reston ebolavirus (REBOV), Ivory Coast ebolavirus (CIEBOV), and the newly observed Bundibugyo ebolavirus species, which was discovered in the most recent outbreak in 2007 (Jones et al.2005). Of the five species ZEBOV is cited to be the most lethal strain with up to 90% mortality rate during outbreaks (Geisbert et al.2010). EBOV outbreaks are commonly found throughout central Africa, although they are not constrained to this area as they easily and rapidly spread.
There are many symptoms involved with the onset of EBOV. The first mild symptoms include: fever, fatigue, anorexia, malaise, myalgia, severe frontal headache, and pharyngitis. These preliminary symptoms are able to last two to sevens days. As the virus continues to spread throughout the patient the symptoms continue to worsen as melena, epistaxis, confusion, hearing loss, and maculopopular rash begins to form, which is then followed by vomiting and bloody diarrhea. The final characteristic of EBOV is uncontrollable haemorrhage, which leads to death as victims fall into shock related to the immense amount of blood lost (Cohen 2004 and Ledgerwood et al.2011). The first recorded outbreaks of EBOV were in 1976, as two outbreaks of different strains occurred. The outbreaks arose in northern Zaire (ZEBOV) and caused a 90% mortality rate (Figure 2), and the other outbreak occurred in southern Sudan (SEBOV) and resulted in a 50% mortality rate (http://microbewiki.kenyon.edu/index.php/Filoviridae). Since these initial outbreaks there have been 25 more EBOV outbreaks, of which four were epidemic (http://www.cdc.gov/ncidod/dvrd/spb/mnpages/dispages/ebola/ebolatable.htm). The first EBOV vaccine used on nonhuman primates consisted of a DNA prime-adenovirus boost approach (Jones et al.2005).Vaccination techniques have greatly altered from this first attempt and have displayed more efficient apothegenic results.
Transmission and Reproduction
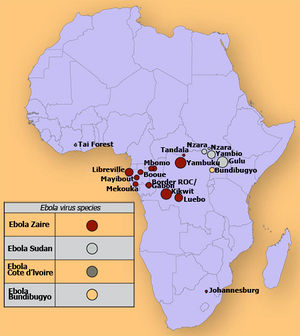
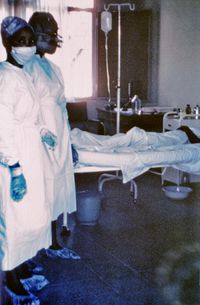
Ebola virus (EBOV) is fatal to Africa as the majority of major outbreaks have emerged from central Africa (Figure 3). EBOV is not only a dangerous virus because it is a virulent pathogen, but also because it spreads rapidly as this virus is easily transmitted between individuals. It is still unclear how the virus first began to spread, but it is believed that humans incidentally obtained the virus from direct contact with contaminated animals, which are usually in the form of dead carcasses (Ledgerwod et al.2011). There is an increased belief that cave dwelling fruit bats are a reservoir for EBOV as evidence of asymptomatic infection has been confirmed in three species of these fruit bats (Ledgerwood et al.2011). The most common way the virus is spread is through direct contact with an infected individual, whether human or nonhuman primate (Hartlieb et al.2005). The virus is transmitted through contact with bodily fluids, blood or tissue. It is also commonly transmitted in third world hospital environments where contact with infected bodily fluid is common. This commonly occurs through reuse of unsterilized, contaminated needles, and syringes, which increases the spread of the viral pathogen (Jaax et al.1995). EBOV most frequently enters individuals through openings in the skin, such as cuts or scrapes, as well as through the gastrointestinal tract, and conjunctiva (Johnson et al.1994).
Along with these natural forms of transmission, other studies have found an unnatural transmission of the virus through the air. Aerosol transmission was first discovered in 1992 during an EBOV outbreak. Monkeys located in a quarantine facility quickly all became infected with EBOV even though they were separated from each other in individual cages (Johnson et al.1994). Shortly after it was determined that EBOV is capable of unnaturally being transmitted by aerosol, which has displayed high rates of infection when it is inhaled as particles in the air (Leffel et al.2004). Based on these terrifying results EBOV, along with MARV, have been categorized as category A biological weapons, and as a possible threat of bioterrorism (Leffel et al 2004, Yermolina et al.2010). This has lead to a large scare as there is currently no vaccine for EBOV.
EBOV has an encapsulated negative-stranded RNA genome that is 19 kb long and codes for seven structural proteins. These seven proteins include: nucleoprotein (NP), VP35, VP40, glycoprotein (GP), VP30, VP24, and L protein, which provides RNA-dependent RNA activity (Leroy et al.2001). A large breakthrough in recent studies was the discovery that EBOV, like other viruses, uses host cellular protein machinery to assemble viral replicants, and to bud new copies of the virus from the host cell membrane as EBOV reproduces asexually inside of the host cell (Hartlieb et al.2005). Of the seven structural proteins, VP40 is the major structural protein as it is composed of vital information for the replication process, including assembly and budding of new viral copies (Hartlieb et al.2005). An imperative process for viral replication is RNA binding, and therefore octamer formation (Hoenen et al.2005). The envelope of EBOV is covered in many GP, which is a transmembrane protein, and binds to the host cell membrane. Binding to the host cell membrane allows the virus to freely enter into the cytoplasm of the host cell (Hartlieb et al.2005). Once the GP binds to the host cell the viral membrane fuses with the host cell membrane allowing the viral particles to be released into the host cytoplasm (http://microbewiki.kenyon.edu/index.php/Filoviridae). After the viral parts enter the host cell, EBOV VP40 is transported from the endosome to the plasma membrane via the retrograde late endosomal pathway by means of multi-vesicular bodies (MVBs) (Hartlieb et al.2005). Once located in the plasma membrane, VP40 is able to localize viral assembly and budding machinery, from the host, with the help of Tsg101 and HECT domain (Hartlieb et al.2005). GP then re-localizes to MVBs and is transported to the site of assembly and budding on the plasma membrane (Kolesnikova et al.2004). NP becomes expressed and forms intracellular inclusion bodies (Hartlieb et al.2005). NP determines the structure of the nucleocapsid, and recruits VP30, VP35, and L protein into the inclusion bodies in the nucleocapsid (Becker et al.1998). Once all the protein structures are in place, budding of new viral copies begins (Hartlieb et al.2005). This is a very rapid process as many untreated patients die within 5-7 days after exposure to this lethal pathogen (Hartlieb et al.2005).
Immune Response to EBOV
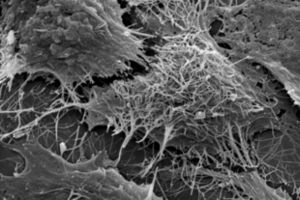
The first line of defense against viral pathogens is the innate immune system. The immune system exploits multiple defense mechanisms to minimize replication and spread against incoming viruses (Kaletsky et al.2008). The EBOV protein, VP40, is capable of producing virus-like particles (VLP) that resemble EBOV and bud from host cell membranes (Kaletsky et al.2008). The presence of tetherin (Bst-2), which is a recently discovered IFN-induced cellular response factor, has shown to inhibit the release of HIV-1 and HIV-2, along with other related retroviruses (Keletsky et al.2008 and Lopez et al.2010). Recent studies have shown that tetherin is not limited to the inhibition of retroviruses as it prevents the release of a much broader range of enveloped viruses, including filovruses, such as EBOV. The viral pathogen remains attached to the surface of mammalian cells when tetherin is present as they physically interact with each other, and remain connected. This physical linking of the membranes prevents the budding of new viral pathogens from the host membrane, and therefore decreases the spreading of EBOV throughout the host (Neil et al.2007). Tetherin anchors EBOV VLPs to the surface of the cell by proteinaceous interactions (Figure 4) (Kaletsky et al.2008). It may seem that this is sufficient to prevent such a deadly virus, and there is no need for a vaccine as the human immune system is adequate to prevent the spread of this deadly virus by securing EBOV to mammalian cell surfaces. Unfortunately this is not the case as EBOV, like many other viruses, has evolved a strategy to overcome the inhibition by tetherin (Kaletsky et al.2008).
One of the seven structural proteins produced by the EBOV genome, glycoprotein (GP), is used as an antagonist to tetherin suppression activity. This mechanism displayed by EBOV is not fully understood, but was originally thought to be fairly similar to the mechanism used by HIV-1 and HIV-2 viruses, which represses tetherin function as well. The HIV-1 virus is able to limit the effects of tetherin by the use of an accessory protein, Vpu. Vpu inhibits tetherin-induced particle retention (Neil et al.2008). In a similar fashion HIV-2 also reduced the effects of tetherin through the use of Env (Lopez et al.2010). Both HIV-1 and HIV-2 are capable of suppressing the tethering effects by removing tetherin from the cell surface, which is a difference in the mechanistic approach to limit tetherin activity in EBOV.
In EBOV, the GP acts in a similar manner to Vpu, as GP advocates EBOV replication and budding of new viral replicates even in the presence of tetherin. However, there is a large difference in the tetherin avoidance mechanism displayed by EBOV in which GP does not significantly remove tetherin from cell surfaces as a means of reducing its effects on viral budding (Lopez et al. 2010). This evidence suggests that EBOV, unlike HIV-1or HIV-2 is able to bypass tetherin as a means of suppressing its effects (Lopez et al.2010). The presence of GP allows viral budding to occur to a level similar to that when tetherin is not present. It is still not fully understood, mechanistically, how GP allows for viral budding to continue, but current research is continuing to reveal new ideas of its exact mechanism, and is currently hypothesized that GP is able to suppress tetherin restriction by using an avoidance mechanism (Lopez et al.2010).
Upon transmission of EBOV, the immune system begins to use defense mechanisms to inhibit the replication and spread of the deadly illness. The human body’s immune response to EBOV is very complex and involves many timely steps in an attempt to inhibit the spread of this deadly pathogen. Around 5-7 days after initial exposure to EBOV a strong inflammatory response is triggered and results in high levels of proinflammatory cytokines. The inflammatory response minimizes viral replication and spread of the virus (Leroy et al.2001). These inflammatory responses are temporally associated with an anti-inflammatory response in which detectable levels of anti-inflammatory mediators are present (Leroy et al.2001). Following this step, T-cell up-regulation of T-cell cytokines and T-cell activation markers occurs, and is associated with cytotoxic cell activation. The decline of cytotoxic activity is temporally associated with the emergence of the apoptotic marker and EBOV-specific IgG antibodies, IgG1 and IgG3. This coincides with the removal of viral RNA (Leroy et al.2001). These results provide hope to many who become infected with the deadly virus as the patients in this study were able to overcome the pathogenic effects of EBOV solely with defense mechanisms provided by the immune system. However, these individuals were only infected with a minor concentration of the EBOV virus, and during most epidemic outbreaks much higher concentrations of the fatal virus are observed in infected individuals (Leroy et al.2001). At these high concentrations the immune system may not be able to react as efficiently to the infection.
Ebola virus Vaccines and Cures
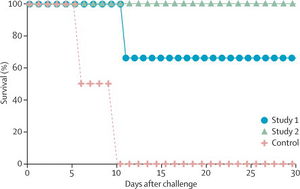
When the human immune system is not able to defend against viral pathogens, like Ebola virus (EBOV), then we have to rely on vaccines to protect patients from the virus. Many recent studies have focused on the treatment of the deadly EBOV virus, since there is no current cure or vaccine for this virus that has plagued parts of the world for more than 30 years (Geisbert et al.2010). All current studies are still performed on non-human primates, and other test animals, such as rats and guinea pigs. A present study is attempting to find a post-exposure cure for the most lethal Ebola virus strain, Zaire Ebola (ZEBOV), which has approximately a 90% mortality rate during outbreaks. This current study is using RNA interference techniques in an attempt to protect patients against ZEBOV. A vital protein associated with the viral RNA genome is the L protein, which serves as an ideal antiviral target because it provides the RNA-dependent RNA polymerase activity of ZEBOV. Along with polymerase activity L proteins are also dissimilar to mammalian proteins making it a much easier target for a vaccine (Geisbert et al.2010). Three small interfering RNAs (siRNA) that target the L protein, VP24, and VP35 genes were used in an attempt to silence three separate stages of the ZEBOV virus (Geisbert et al.2010). This cocktail of siRNAs was encapsulated in stable nucleic acid-lipid particles (SNALPs) and injected into non-human primates intravenously (Hensley et al.2006). All non-human primates were completely cured of ZEBOV following seven treatments of the siRNA cocktail (Geisbert et al.2010). This technique is not flawless as siRNAs have the potential to cause immune activation, which may cause further problems as immunostimulation is highly toxic, especially in humans. However, the effective results obtained were a milestone in the search for a cure as 100% of the non-human primate test subjects were completely cured of the highly lethal ZEBOV virus (Figure 5). Based on the results this technique provides hope toward finding an efficient cure for humans that have fallen victim to this deadly virus.
Another current approach in an attempt to find a vaccine for EBOV is based on live attenuated recombinant vesicular stomatitis viruses (rVSV). This approach is appealing as the vaccine is capable to be administered mucosally through the nasal passage (Jones et al.2005). Another reason this technique is attractive as a vaccine is because this same rVSV technique has been highly effective in previous animal studies associated with vaccines for other deadly viruses, such as AIDS (Rose et al.2001). The non-human test animals were injected intraperitoneally (IP) with the live attenuated rVSV (Garbutt et al.2004). The test animals were infected with Zaire Ebola virus (ZEBOV), which is the deadliest known strain of EBOV as past outbreaks have resulted in the highest death rates of any EBOV epidemics with mortality rates as high as 90% (Geisbert et al.2010). After the rVSV vaccination was administered to the newly virally infected test animals they found no signs or symptoms of ZEBOV as all test animals were protected from the virus. It was found that those infected with the EBOV displayed low to moderate levels of IgG antibody titers which are resistant against ZEBOV glycoprotein (Jones et al.2005). These results indicate that the live attenuated rVSV is apathogenic for the test animals (Jones et al.2005). A large breakthrough was that infected individuals were protected from the deadly ZEBOV virus with one dose of the rVSV vaccine (Jones et al.2005). The results of this study provide hope that these apathogenic results will carry over in future studies on humans infected with EBOV.
Developing a vaccine that is effective and safe is challenging (Figure 6). A candidate vaccine must inhibit the viral pathogen and protect the host in non-human primates. The vaccine can not just be effective, as it must be proven to be safe to the non-human primate patient as well. Lastly and most importantly, candidate vaccines must be immunogenic in human patients before they can be administered as a vaccine (Ledgerwood et al.2011). A new preliminary vaccine for EBOV, known as rAd5, has been proven to be safe and effective. This vaccine is a glycoprotein (GP) antigen as it induces a single amino acid point mutation by replacing an aspartate with a glutamate at position 71 in the N-terminus of the amino acid sequence (Ledgerwood et al.2011). Not only is this new candidate vaccine proven to be safe for human use, but it has also proven to be effective with a single dose. When a rAd5 dose concentration of 2x10^10 VP was administered, all of the patients displayed GP binding antibodies with a single dose. Not only did the candidate vaccine work as a GP binding antibody, but it also induced T-cell response to the site of the point mutation (Ledgerwood et al.2011). T-cell activation is an immune system response that acts as a natural viral defense mechanism (Leroy et al.2001). The immunogenic response, and safe consumption of the potential vaccine displays another positive step toward finding a cure for the lethal viral pathogen, EBOV (Ledgerwood et al.2011).
Conclusion
Ebola virus, a member of the Filoviridae virus family, is still an untamed, highly lethal viral pathogen that represents a nightmare for much of central Africa, which is the site of the majority of EBOV outbreaks (Geisbert et al.2010). Unfortunately there has not been a large push in the search for a vaccine as this virus, as deadly as it is, has not impacted a large portion of the world’s population with only 2,300 reported cases of hemmorraghic fever caused by filoviruses. However, the recent potential of threat of using EBOV as a bioterrorist weapon has placed a slight push toward discovery of a virus as the virus is extremely lethal as an aerosol (Leffel et al. 2004). Surprisingly this virus has stumped researchers for years as there is still not an effective vaccine that is able to be administered to those who are infected with the virus. On a more positive note there are many candidate vaccines that have displayed very effective results on non-human primates, as they have protected these patients from the viral effects of EBOV. Many of these potential cures may become a future vaccine to help save the lives of those who have fallen victim to the deadly illness. Leading the way in the race for a cure is the recent work done by Geisbert et al.(2010), who has obtained nearly flawless results through the use of siRNAs to target and inhibit the lethal effects of EBOV. With the persistence and drive of the researchers that continue to be hard at work in search for a vaccine, we may someday soon be able to eliminate the fear of future epidemic EBOV outbreaks, and save many innocent lives from being taken by the deadly virus.
References
Cohen, J. 2004. Containing the threat-don’t forget Ebola. PLOS Medicine 1(3): 188-189.
Hartlieb, B., W. Weissenhorn. 2005. Filovirus assembly and budding. Virology 344(2006): 64-70
http://www.cdc.gov/ncidod/dvrd/spb/mnpages/dispages/ebola/ebolatable.htm
http://microbewiki.kenyon.edu/index.php/Filoviridae
Edited by student of Joan Slonczewski for BIOL 238 Microbiology, 2011, Kenyon College.
