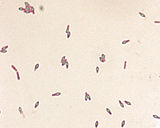
Foodborne Botulism
Introduction
Foodborne botulism is a rare but sometimes deadly disease that occurs all over the world. It can range from having mild symptoms, which may be misdiagnosed or disregarded, to a more serious condition that can be lethal within a day. Botulism occurs as a direct result from exposure to, or the ingesting of, a botulinum neurotoxin; the most toxic natural substance known. Produced from the bacteria Clostridium botulinum, the neurotoxin will only proliferate under ideal environmental conditions. Foodborne botulism is typically associated with exposure to improperly canned foods and/or contaminated food products, and is a condition that adversely affects the nervous system. Diagnostic tests and treatments for this disease continue to improve as advancements in technology are made. Although foodborne botulism has not been eradicated, public awareness in the United States continues to grow along with continued efforts made to minimize occurrences of the disease.
Clostridium botulinum
See also Clostridium botulinum
Clostridium botulinum is a gram-positive, anaerobic, rod-shaped bacterium that produces the botulinum neurotoxin, which is the cause of foodborne botulism. The bacteria lie dormant as spores in the stationary-phase until exposed to ideal environmental conditions that enable them to germinate, in which the neurotoxin is then produced. These spores are also very resistant to adverse environmental conditions so eradication of them is difficult. Proliferation of these spores occurs if conditions include for "group I" (discussed below) optimal temperatures between 35-40°C and a minimum pH of 4.6, while "group II" requires the temperature to be between 18-25°C and a minimum pH of 5.0, with both groups requiring anaerobic conditions [1].
Classification
There are four distinct groups (designated I-IV) in which C. botulinum is categorized, and is solely determined by the characteristic of botulinum neurotoxin production. Groups I and II are both directly responsible for the cause of disease in humans. The botulinum neurotoxins can also be divided into seven antigenically distinct types, A–G, and are some of the most potent toxins known [2]. Group I contains proteolytic strains (those that are able to break down proteins due to the enzymes they produce), while group II contains nonproteolytic strains. Foodborne botulism is almost always associated with groups I and II, and (depending on the group) produce the toxin types A, B, E and F. Toxin types A and B are the most common causes of foodborne botulism while type F is the least common. Type E is most commonly associated with the consumption of contaminated marine products. The most common cause of food poisoning in the United States is toxin type A, while for most of Europe the most common cause is toxin type B.
| Characteristics | Group I | Group II |
|---|---|---|
| Neurotoxin types | A, B, F | B, E, F |
| Cause of human disease | Yes | Yes |
| Proteolytic | Yes | No |
| Disribution in the environment | Type A in the Western U.S.; Type B in the Eastern U.S. and in most of Europe | Type E common in marine sites worldwide |
Genome
Many of the Clostridium botulinum strains have been sequenced and many others are in the process of being sequenced. Information has been gathered from sequenced strains and has been useful in understanding how Clostridium botulinum is able to synthesize one of the most lethal neurotoxins. The genome of C. botulinum strains varies from 3.6Kb to 4.0Kb. Strain A appears to have the larger genome than the other strains and is also involved with foodborne botulism disease. Some of these strains also contain small plasmids. A short summary of the sequenced strains is provided in Table 2.
| Strain | Chromosome Size | Plasmid Size | GC content |
|---|---|---|---|
| Clostridium botulinum A str. ATCC 19397 (Los Alamos National Laboratory) | 3.8 Kb | none | 28% for chromosome |
| Clostridium botulinum A str. ATCC 3502 (Sanger Institute) | 3.9Kb | pBOT3502 0.016Kb | 28 % for chromosome
26% for plasmid |
| Clostridium botulinum A str. Hall (Los Alamos National Laboratory) | 3.7Kb | none | 28% for chromosome |
| Clostridium botulinum A2 str. Kyoto (Los Alamos National Laboratory) | 4.15Kb | none | 28% for chromosome |
| Clostridium botulinum A3 str. Loch Maree (Los Alamos National Laboratory) | 4Kb | pCLK 0.27Kb | 28% for chromosome
25% for plasmid |
| Clostridium botulinum B str. Eklund 17B (Los Alamos National Laboratory) | 3.8Kb | pCLL 0.048 Kb | 27% for chromosome
24% for plasmid |
| Clostridium botulinum B1 str. Okra okra (Los Alamos National Laboratory) | 3.9Kb | pCLD 0.15Kb | 28% for chormosome
25% for plasmid |
| Clostridium botulinum Ba4 str. 657 (Los Alamos National Laboratory) | 3.9Kb | pCLJ- 0.27Kb, pCLJ2-0.01Kb | 28% for chromosome;
25% for pCLJ; 24% for pCLJ2 |
| Clostridium botulinum E3 str. Alaska E43 (Los Alamos National Laboratory) | 3.6Kb | None | 27% for chromosome |
| Clostridium botulinum F str. Langeland (Los Alamos National Laboratory) | 4.0Kb | pCLI 0.018Kb | 28% for chromosome
26% for plasmid |
Interaction with Food
The interaction between food and a microbial population creates a complex microenvironment, as the presence of a bacteria on food will directly affect the overall food ecosystem. Although C. botulinum is an obligate anaerobe, foods that are aerobic can still become contaminated by this bacteria and are often the source of food poisoning outbreaks. For example, C. botulinum growth in potatoes, cole slaw, and sautéed onions, has caused botulism outbreaks since the oxygen in these foods leaves during cooking and although it diffuses back, it does so so slowly that most of the food product remains anaerobic [5]. Heat resistance of spores can vary greatly among the different species and even among strains. Since group I C. botulinum type A and B strains produce extremely heat-resistant spores, they therefore are the most important subtype for the public health safety of canned foods to be cautious of [6]. The only way to ensure prevention of foodborne botulism is to prevent the neurotoxin production within those foods.
Pathology
Virulence genes and other factors
Clostridium botulinum encodes for the botulism neurotoxins using specific loci which contains the genes encoding for one and in some cases two of the neurotoxins (A-G) and other important factors such as nontoxic nonhemagglutinnin and hemagglutanin [7]. The genes encoding botulism neurotoxin A, B, E and F are found in the chromosome (about 4Kb in size) and those encoding C and D are found in bacteriophage [7]. Clostridium botulinum secrete the neurotoxin as an inactive protein, the protein is later cleaved, and the neurotoxin becomes active by modifying its structure (make disulfide bonds) [7]. The neurotoxin produced is composed of one heavy chain which contains C-terminal and a light chain which contains the N-terminal and an active site for zinc endopeptidase [7]. The N-terminal is known as the translocation domain since it aids in the translocation of the light chain from the vesicle to the cytosol of the presynatic motor neuron where it will be cleaved and use its metallo-protease activity in its target [7]. The ability of the light chain to cleave more than one target protein makes the neurotoxin a very efficient and lethal pathogen, 1ug is sufficient to kill one person and 1g would be sufficient to kill 1,000,000 people [8,9]. In short, Clostridium botulinum encodes a lethal neurotoxin that is engineered to travel to the neuromuscular junction where it performs the cleavage of the target protein.
Mechanism
Clostridium botulinum synthesizes deadly botulism neurotoxins which inhibit the motor neurons of the peripheral nervous system. These neurotoxins prevent the release of acetylcholine in the muscular junction by targeting synaptic proteins which form the SNARE complex involved in exocytosis of the neurotransmitter vesicles [7,8,9]. C. botulinum has specific features to accomplish the inhibition of the release of neurotransmitter. First, C. botulinum bacteria cells secrete the botulism neurotoxin as an inactive polypeptide (150 kD) chain which is able to travel to the intestines where it is cleaved into two molecules- a 100kDa heavy chain and a 50kDa light chain [7,9]. Second, these two molecules are capable of making disulfide bonds with each other and travel to the neuromuscular junction where they exert their metallo-protease activity in their specific targets SNAP-25, VAMP or synthaxin only if these targets are in the uncomplexed form [7,8,9]. Four key steps must take place in order completely inhibit the release of the neurotransmitter: (a) the neurotoxin must bind a membrane receptor in the presynaptic neuron (b) the neurotoxin must then be internalized by receptor- mediated endocytosis (c) the L chain of the neurotoxin must also be traslocated across the endosome and finally (d) the L chain of the neurotoxin must be able to bind specific binding sites (SNARE motifs) and cleave different bonds of the same peptide target found in SNAP-25, synthaxin or VAMP using its metallo-protaise activity [7,8]. Studies have been done to determine which specific strains affect SNAP-25, VAMP or synthaxin. These studies have shown neurotoxin A and E target SNAP-25 whereas neurotoxin B, D, F and G target the VAMP [7,8]. The neurotoxin from strain C, unlike rest of the strains, is able to act in two synaptic proteins SNAP-25 and synthaxin [7,8]. In short, the botulism neurotoxins affect proteins that form the SNARE complex making them incapable releasing neurotransmitter and preventing the peripheral nervous system from performing important functions.
Signs & Symptoms
Botulism is a multi-faceted disease. Different botulism disease types have the same symptoms as foodborne botulism with varying incubation periods and varying risks of acquiring disease symptoms [10].
The symptoms of food botulism can appear as early as 18-36 hours after consuming contaminated food or may be acquired as a later onset of disease as late as 10 days. Botulism is a neurotoxin with many symptoms [11]. Foodborne botulism in adults more often affects the gastrointestinal tract and swollen abdomen may be a subsequent result. This is perhaps why the toxin is more commonly associated with food poisoning. There are other symptoms that are present with the disease. Double vision, droopy eyelids, slurred speech, difficulty swallowing are other signs of the disease. There may also be respiratory complications leading to death. Paralysis and weakness may also be a result [10].
Some patients have mild neurological signs and complain of autonomic symptoms as well as abnormal sudomotor function and high cardiovascular failure [12].
Infant botulism is defined for babies under 6 months of age since children who are older than 6 months begin to develop immune defenses against Clostridium botulinum germination [10]. Symptoms include constipation, weakness, loss of muscle tone, poor feeding, respiratory distress, and alertness although weakness is apparent. Lethargic infants are also common. Prompt diagnosis and immediate treatment must be administered to reduce morbidity and mortality of the disease in infant botulism [13].
Diagnosis and Complications
In diagnosing the botulism disease from the bacteria Clostridium botulinum, the presence of an absent or decreased gag reflex, paralyzed bowel, absent or decreased deep tendon flexes, and urine retention will be observed. Diagnosis may be difficult since the signs of botulism are similar to those of Guilliain-Barre Syndrome, stroke, and myasthenia. To confirm botulism, special test are performed. These tests include a brain scan, spinal fluid examination, or nerve conductive test, and inoculation of mice is performed [11]. The mouse bioassay takes 4 days to complete and is therefore not primary in determining in comparison to clinical diagnosis [16]. ELISA testing can be used in addition to mouse inoculation for further confirmation of the pathogenic organism [16].
An earlier diagnosis will result in better prognosis of foodborne botulism [10].
An infected person, in some cases, will not be able to breathe, which is the most common cause of death in botulism [14]. A higher chance of acquiring aspiration pneumonia, respiratory distress, long-lasting weakness, and nervous system problems for up to a year following the illness is common to the disease [15].
Treatment

Treatment of foodborne botulism varies as it depends on the method in which the microorganism got into the body system as well as the amount of time it has been in the system. The following are methods that physicians may use in order to treat a patient. In cases where the doctor needs an antitoxin, they are able to contact the state health officials or CDC to obtain them. [17]
- If diagnosed early, the foodborne botulism can be treated with equine antitoxin in order to the block the toxin from circulating in the blood.
- If diagnosed late, the patient may experience respiratory failure and paralysis and will need to be placed on a breathing ventilator and in intensive care for several weeks.
- If the botulism was foodborne, it is possible that the doctor will induce vomiting or perform an enema in order to remove the contaminated food.
- If the botulism is by a wound, the doctor may treat it by removing the toxin producing bacteria by antibiotics.
Foodborne Botulism in the United States
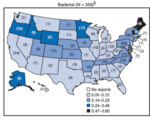
Although there is ongoing research on Clostridium botulinum, it is still not as well-known as other disease-causing microbes, such as Salmonella or E. coli. Foodborne botulism occurs year after year within the United States due to poor home canning methods, and in part due to the limited exposure of information about proper canning methods. Organizations such as the CDC and the FDA, however, have information about Clostridium botulinum on their websites to better inform the public. The limited awareness of some individuals may be due to relative infrequency of botulismm incidinces and media reports compared to Salmonella and E. coli.
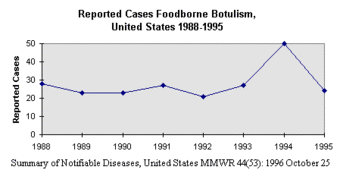
Information from the FDA has shown that from 1988 to 1995, there have been occurrences of botulism yearly. [18] Depending on the region within the United States, different Clostridium botulinum strains are more prevalent:
- Type A botulinum are found mostly in the western regions
- Type B spores are found mostly in the northeast and central states
- Type E spores are found in the marine life in the Pacific Northwest and Great Lakes
Prevention
The occurrence of foodborne botulism in the United States has been ongoing for many years, even during a time when people did not know of the existence of microorganisms and their interaction with food products. Current organizations such as the US Department of Agriculture (USDA), U.S. Food and Drug Administration (FDA), and the Centers for Disease Control and Prevention (CDC) provide detailed information about this topic that is available to the general public. In August of 2001, the USDA implemented a fact sheet to inform the public of the food-dwelling microbes, including Clostridium botulinum, that are potentially harmful to the public given the right conditions. [19] The CDC provides yearly reports of foodborne disease occurrences that are available to the public, including the state in which the incidence occurred and the vehicle of the disease. The increase of public awareness of the ill-effects of microbes, as well as how to prevent them, can lead to the minimization of diseases. For example, the USDA states that any frozen food purchased should be inspected carefully for broken seals or refrozen products. A mishandled food product with these conditions increases the potential for microbial contamination.
Another way in which foodborne botulism can be prevented is through the implementation of statewide standardization measures of proper food canning methods. For example, over 200 licensed canning companies in California must abide by strict rules outlined by the Cannery Inspection Program, concerning standards of hygiene and canning methods. If the facility fails to meet minimum standards, the state of California will force a recall of that product and prevent further manufacturing until standards are met. [20]
If a health care provider is aware of an individual that has been negatively affected by a microbe from a food source, the health care provider should notify the state public health authorities, which then, in turn, notify the CDC, USDA and the FDA. Diagnostic tests are then performed to explicitly identify the microbe responsible.
Although the United States attempts to minimize the amount of cases of Clostridium botulinum per year, it cannot be completely eradicated. Advancements in food technology was not enough to prevent an outbreak of the botulinum toxin in chili sauce in 2007. Although all of the products were recalled after eight incidents, there was still another individual whom became ill after consuming the contaminated food product. [21]
A Guide to Home-Canning
In an effort to prevent the prevalence of foodborne botulism from increasing in the United States, the USDA implemented a guide to home-canning. This guide suggests methods of “selecting, preparing and canning” fruits, vegetables, meats, jams and jellies.
In general, home-canned foods should be performed with the following conditions:
- Be sure that the jars used are washed in hot water and detergent.
- Store the jars at around 50-70 degrees Fahrenheit
- If possible, try the method of “hot packing” which removes most of the oxygen from the food
- Acidity: the acidity of the canned food can determine whether the botulinum spores live or not. At high acidic levels, or at low pH levels, the botulinum toxin would not be able to grow.
- Low-acid level (pH>4.6) allows for botulinum toxin growth
- High-acid level (pH<4.6) prevents botulinum growth
- The product should be sterilized at temperatures of 240-250 degrees Fahrenheit in order to ensure that the microorganism is destroyed.
For more detailed information on canning foods at home, please follow this link to the USDA canning website. USDA Complete Guide to Home Canning [22]
Summary
Foodborne botulism, caused by a neurotoxin-producing bacteria Clostridium botulinum , is a quick-acting, aggressive disease that negatively affects the nervous system. It is important to avoid the microorganism by taking preventative measures against all levels of exposure. Such precautions include ensuring food products are packaged, cooked, and maintained at proper environmental levels to minimize the possibility of C. botulinum contamination. If there is by chance, consumption of C. botulinum, an early diagnosis will decrease the chance of a secondary disease and death. The United States has implemented many ways to prevent food contamination with the botulism toxin, but even with these preventative suggestions there are still cases of botulism in the United States. Although a better understanding of how the botulinum neurotoxin functions pathogenically continues to increase, Clostridium botulinum still poses a great threat to the public's health. Since botulism is such a compromising disease, worldwide public awareness and education of this disease should continue to be encouraged.
References
1. Montville, T. J., & Mathews, K. (2005). Food Microbiology: an introduction (p. 192-193). Washington, DC: ASM Press
2. Hatheway, C. L. (1990, January). Toxigenic Clostridia (Electronic version). Clinical Microbiology Reviews, 3, 71-74.
3. McLauchlin, J., Grant, K.A., & Little, C.L. (2006, August). Food-borne botulsim in the United Kingdom (Electronic version). Journal of Public Health, 28, 339 (Table 2).
4. Data obtained from http://www.ncbi.nlm.nih.gov/sites/entrez?db=genomeprj&cmd=DetailsSearch&term=txid1491%5Borgn%5D+AND+pt_default%5Bprop%5D&log$=activityDownload this as a file
5. Montville, T. J., & Mathews, K. (2005). Food Microbiology: an introduction, (pp. 12). Washington, DC: ASM Press
6. Montville, T. J., & Mathews, K. (2005). Food Microbiology: an introduction, (pp. 33). Washington, DC: ASM Press
7. Simjee, Shabbir, ed. Foodborne diseases. Totowa, N.J.: Humana Press, 2007. p. 41-70.
8. Giampietro Schiavo, Michela Matteoli, and Cesare Montecucco.Neurotoxins Affecting Neuroexocytosis. Physiol. Rev. 2000; 80: 717-766.
9. Koussoulakos S: Botulinum Neurotoxin: The Ugly Duckling. Eur Neurol 2009; 61:331-342.
10. World Health Organization.“Botulism” 2002. WHO Media Center. 20 August 2009. < http://www.who.int/mediacentre/factsheets/fs270/en/>.
11. Centers for Disease Control and Prevention. “Botulism”. 21 May 2008. Department of Health and Human Services. 19 August 2009. < http://www.cdc.gov/nczved/dfbmd/disease_listing/bo tulism_gi.html#4>.
12. Topakian R, Heibl C, Stieglbauer K, Dreer B, Nagl M, Knoflach P, Aichner FT. “Quantitative Autonomic Testing in the Management of Botulism”. May 2009. Department of Neurology, Academic Teaching Hospital Wagner-Jauregg, Wagner-Jauregg-Weg 15, Linz 4020, Austria. 20 August 2009.< http://www.ncbi.nlm.nih.gov/pubmed/19240955?ordinalpos=4&itool=Ent rezSystem2.PEntrez.Pubmed.Pub med_ResultsPanel. Pubmed_DefaultReportPanel.Pubmed_RVDocSum>
13. Lavoie D, Pawar G, Khan A. “Infantile Botulism a Case Report”. Sept-Oct 2006. Dept. of Neurology, West Virginia University School of Medicine, Morgantown, USA. 20 August 2009. <http://www.ncbi.nlm.nih.gov/pubmed/17285950?ordinalpos=1&itool=EntrezSystem2.PEntrez.Pubmed.Pubmed_R esultsPanel.Pubmed_DiscoveryPanel.Pubmed_Discovery_RA&linkpos=1&log$=relatedarticles&logdbfrom=pubmed>.
14. Mayo Clinic Staff. “Botulism-Complications”. 28 March 2008. Mayo Foundation for Medical Education and Research. 20 August 2009. <http://www.mayoclinic.com/health/botulism/DS00657/DSECTION=complications>.
15. Arnold L. Lentnek. “Botulism”. 16 August 2007. VeriMed Healthcare Network. 20 August 2009. < http://www.nlm.nih.gov/medlineplus/ency/article/000598.htm>.
16. Cai S, Singh BR, Sharma S. “Botulism Diagnostics: From Clinical Symptoms to In Vitro Assays”. Apr-Jun 2007. Botulinum Research Center, and Department of Chemistry and Biochemistry, University of Massachusetts Dartmouth, North Dartmouth, Massachusetts 02747, USA. 20 August 2009.<http://www.ncbi.nlm.nih.gov/pubmed/17558660?ordinalpos=1&itool=EntrezSystem2.PEnt rez.Pubmed.Pubmed_Resu ltsPanel.Pubmed_DiscoveryPanel.Pubmed_Discovery_RA&linkpos=5&log$=relatedreviews&logdbfrom=pubmed>.
17. Center for Disease Control and Prevention. Department of Health and Human Services. Disease Listing: Botulism General Information. Web. <http://www.cdc.gov/nczved/dfbmd/disease_listing/botulism_gi.html>.
18. U.S. Department of Health and Human Services. U.S. Food and Drug Administration. BBB - Clostridium botulinum. 4 May 2009. Web. <http://www.fda.gov/Food/FoodSafety/FoodborneIllness/FoodborneIllnessFoodbornePathogensNaturalToxins/BadBugBook/ucm070000.htm>.
19. United States Department of Agriculture. Food Safety and Inspection Service. Frozen, Fully-Cooked Products & Botulism - Food Safety Advisory. Sept. 2001. Web. <http://www.fsis.usda.gov/Fact_Sheets/Frozen_Fully_Cooked_Products_&_Botulism/>.
20. California Department of Health Care Services. Food and Drug Branch. Cannery Inspection Program. Web. <http://www.dhs.ca.gov/fdb/HTML/Food/indexcan.htm>.
21. Centers for Disease Control and Prevention. Department of Health and Human Services. Botulism Associated with Canned Chili Sauce, July-August 2007. Center for Disease Control and Prevention, 21 Aug. 2007. Web. <http://www.cdc.gov/botulism/botulism.htm>.
22. United States Department of Agriculture. USDA Complete Guide to Home Canning. 1994. USDA Complete Guide to Home Canning, 2006 revision. Web. <http://www.uga.edu/nchfp/publications/publications_usda.html>.
Images
1. Centers for Disease Control and Prevention's Public Health Image Library, Courtesy of Larry Stauffer, Oregon State Public Health Laboratory, with identification number #1932. (2002). Clostridium botulinum spores stained with Malachite Green Stain. http://phil.cdc.gov/phil/details.asp
2. Centers for Disease Control and Prevention. Trivalent antitoxin (not Type A monovalent). http://www2a.cdc.gov/phtn/botulism/treatment/treatment.asp
3. Centers for Disease Control and Prevention's Morbidity and Mortality Weekly Report. (2006). Rate of reported foodborne disease outbreaks per 100,000 standard population and number of outbreaks. http://www.cdc.gov/mmwr/PDF/wk/mm5822.pdf
4. . U.S. Food and Drug Administration. Reported Cases Foodbotulism, U.S. 1988-1995. http://www.fda.gov/Food/FoodSafety/FoodborneIllness/FoodborneIllnessFoodbornePathogensNaturalToxins/BadBugBook/ucm070000.htm
5. Centers for Disease Control and Prevention's Public Health Image Library, Courtesy of Dr. Chas Hatheway, with identification number #3355. (1977). These were jars of contaminated Jalapeño peppers involved in an outbreak of botulism in Pontiac, Michigan, April, 1977. http://phil.cdc.gov/phil/details.asp
Edited by Carolina Ceballos, Cristina Flores, Nancy Gomez, Malisa Tov, students of Rachel Larsen