Mycobacterium avium subspecies paratuberculosis
A Microbial Biorealm page on the genus Mycobacterium avium subspecies paratuberculosis
.
Classification
Higher order taxa
Bacteria (Domain); Actinobacteria (Phylum); Actinobacteria (Class); Actinobacteridae (Subclass); Actinomycetales (Order); Corynebacterineae (Suborder); Mycobacteriaceae (Family); Mycobacterium (Genus); Mycobacterium avium complex (MAC) (Species group) [11]
Species
Mycobacterium avium
Subspecies
Mycobacterium avium subspecies paratuberculosis
Commonly referred to as MAP or Map
Also known as: Mycobacterium paratuberculosis, Mycobacterium johnei, Bacillus paratuberculosis, Bacterium paratuberculosis, Mycobacterium enteritidis, Darmtuberculose, and Mycobacterium avium paratuberculosis [11]
The classification of this organism has been subject to debate. Isolated over 100 years ago, it was originally termed Mycobacterium enteritidis chronicae pseudotuberculosae bovis johne [13]. Current classifications depend on genetic composition and phenotypic characteristics. With a genome almost identical to that of Mycobacterium avium (M. avium) and its subspecies, the International Association for Paratuberculosis has recognized the subspecies term (Map) as fitting. On the other hand, some researchers and organizations still use the name M. paratuberculosis, not only for simplicity, but as a result of its significant phenotypic variances from M. avium [3, 8].
Description and significance
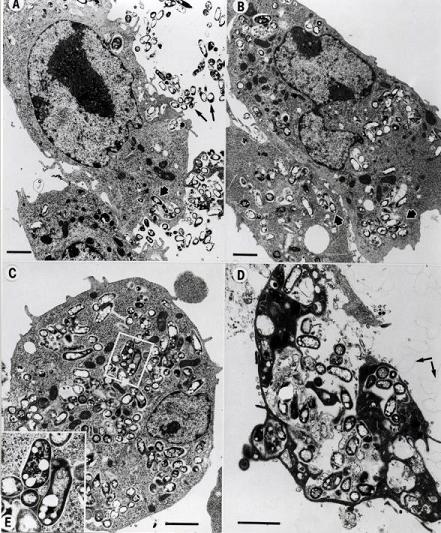
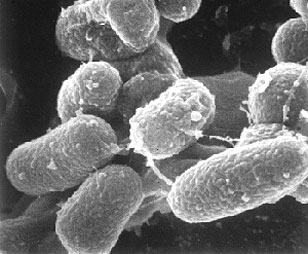
Mycobacterium avium subspecies paratuberculosis (Map) is the etiologic agent of Johne’s disease (pronounced “YO-nees” [8]) also known as paratuberculosis. It was first isolated by German scientists H.A. Johne and L. Frothingham over a century ago from diseased animals displaying inflammation of the ileum [13]. Johne’s disease, named for one of its finders, is a mammalian disease that resembles some clinical and pathological aspects of Crohn’s disease in humans [2], and which has become an increasingly relevant problem for cattle farmers and the economy worldwide. Map is found primarily in ruminants (cattle, sheep, goats, deer, antelope, bison, etc) and their three-chambered stomach relatives [3]. Johne’s disease has been studied extensively in dairy cattle, where it has been called one of the most serious diseases affecting these animals to date [4]. It is estimated that 20% of dairy herds and 8% of beef herds in the United States are infected [6], leading to a $1.5 to 2 billion loss for the cattle industry each year. Adding to this problem, Map has also been found to infect a variety of other wild animals, such as badger, fox, primates, rabbits, and swine [1]. Different strains of Map have been found equally distributed throughout the affected species (the same strain of bacteria is able to infect multiple types of animals), contributing to this wide host range and ease of transfer between species [8], all of which make the bacteria and disease very hard to keep track of. Also making Map hard to track is its long incubation period in host organisms. Though animals are infected at a young age, they don’t begin to show visible symptoms until adulthood, at which point they have reached the critical stages of disease and rarely survive [3, 5].
Map, an obligate intracellular pathogen, is a small (0.5 x 1.5 micron [3]), rod shaped bacteria which grows in circular colonies reaching about 1-2 mm in diameter [13]. It is usually found to be off-white or yellow depending on the medium [3], and has the ability to adapt easily to many environments. Map not only can evade host defenses and survive within phagosomal compartments for more than two weeks, but it has also been found to reprogram the pattern of gene expression of bovine macrophages to increase its chance of survival and pathogenesis within the host [1, 13]. Though it requires a suitable cell medium for growth, Map can survive in the environment well beyond its presence in an animal host, creating drastic problems for farmers trying to eradicate Johne’s disease from their herds.
Due to the steady increase of Map infection prevalence throughout cattle farms of the world and the economic impacts which result, methods of detecting Map from environmental cultures are currently being studied and may provide insight into the infection mechanisms of this pathogen and thus provide a basis for the development of drugs which may eradicate Johne’s disease altogether. Also, the close relation between characteristics of Johne’s disease in ruminants and Crohn’s disease in humans (a chronic inflammatory bowel disease) has created an ongoing debate of whether or not Map is a possible causative agent of this human disease as well. Though it has been fully sequenced, further functional characterization of the Map genome may solve this mystery between Map and Crohn’s by increasing our understanding of the molecular biology as well as the physiology, pathogenesis and host specificity of this bacterium [9].
Genome structure
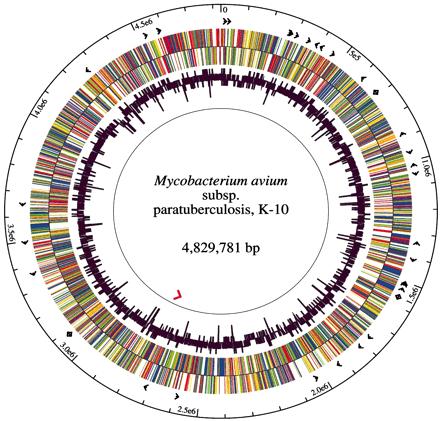
The Map strain used for sequencing, K-10, was originally isolated from a dairy herd in Wisconsin by investigators of the USDA National Animal Disease Center [10]. This strain is a typical bovine type II clinical isolate which was chosen because of its high efficiency of transformation with plasmid DNA [1], its virulence and its amenability to transposition mutagenesis. By random shotgun sequencing, 1.8- to 3.0-kb fragments were cloned into pUC18 and 66,129 sequences were used to create the final genome assembly. As represented in the figure, the K-10 Map genome has a single circular chromosome of 4,829,781 base pairs, 91.3% of which are protein coding. Map has a GC (guanine cytosine) content of 69.3%, an average gene density of 1,112 base pairs per gene and an average gene length of 1,015 base pairs. This genome encodes 4,350 ORFs, 45 tRNAs and 1 rRNA operon. 39 protein sequences were found within the Map genome which have no identifiable homolog recorded as of yet. About 1.5% of the Map genome consists of repetitive DNA [7].
Of the 19 insertion sequences identified in the K-10 genome, most represent homologs of other Mycobacterium IS elements. IS_MAP02 and IS_MAP04 are of interest because they have no homologs in other mycobacteria and thus could possibly be used as specific diagnostic targets for Map. The Map genome encodes for all proteins involved in the following metabolic pathways: glycolysis, the pentose phosphate pathway, the tricarboxylic acid cycle, and the glyoxalate cycle. Also, the large number of genes for regulatory function found within the genome is consistent with Map’s ability to survive in a wide range of environmental conditions. One major difference between Map and other mycobacteria is its inability to produce mycobactin in vitro, which is a siderophore responsible for the binding and transport of iron into the cell. A sequence comparison of the mycobactin gene cluster between Map K-10, M. avium strain 104 and M. tuberculosis strain H37Rv reveals a possible reason for this deficiency. Within this cluster, the mbtA gene is much shorter in Map than the other two, lacking more than 200 residues important for protein function. Though this needs to be tested more thoroughly, this truncated domain may be the limiting factor in mycobactin production for Map since MbtA has been found to initiate siderophore synthesis. One additional Map genome feature to note is the extentsive functional redundancy; a result of gene duplication, this redundancy is based on amino acid content and is usually high among genes involved in lipid metabolism and oxidoreduction [7]. A greater concentration of proteins for lipid metabolism in Map compared to other species may reflect its requirement of a robust cell wall which allows it to survive and colonize in the ruminant intestine [9].
Cell structure and metabolism
Map is a small, slow-growing, gram-positive, acid-fast positive, rod-shaped, multispecies pathogenic bacteria. It is aerobic, has no mechanisms of motility and has a cell wall made up of a waxy mixture of lipids and polysaccharides [3, 10]. The cell wall of a pathogen must act as an interface between the cell and its host, and thus will structurally display that parasite’s virulence. In the case of Map, a thick waxy cell wall made up of 60% complex lipids not only gives it the properties of an acid fast bacteria (the ability to resist decolorization by acidified alcohol), but it also creates hydrophobicity and an increased resistance to low pH, high temperature, and a variety of chemicals, increasing its longevity and pathogenic potential in harsh and varied environments [8, 13]. Studies have shown that virulence may be increased in Map by the presence of two copies of the five genes (fabG2, accD4, kasB, fabG3 and fabG5) involved in the fatty acid biosynthetic pathway through the combined action of these fatty acid synthases and polyketide synthases to create the complex lipid components of the membrane [9].
A thick cell wall also contributes to the slow growth rate of Map by decreasing the flow of nutrients into and out of the cell. Map is actually the slowest growing of all cultivated mycobacteria; under optimal conditions, it takes over 20 hours to generate. A Map isolate can produce small colonies within 3-6 weeks when grown in the optimal temperature of 37 degrees C under aerobic conditions [13]. As an aerobic organism, Map requires oxygen in its environment for metabolism; in order to survive in low-oxygen environments, it produces isocitrate lyase, an essential anapleurotic enzyme which assists in survival within microaerophilic conditions inside the host. In terms of metabolism, Map has a functional glycolytic pathway and tricarboxylic acid (TCA) cycle. The presence of an additional FAD binding domain in the fdhF gene, and the intact iron-sulfur domain within the fdxB gene possibly indicate an alternate survival strategy for Map which would be similar to that of the anaerobic survival of M. Tuberculosis under starvation [9].
Mycobactin is a siderophore unique to the mycobacterial family. This chemical is secreted from the membrane in order to break down and transport iron (an essential nutrient for growth) into the cell. Map is unique in that it does not produce mycobactin on its own like the rest of its genus, and thus requires a host cell to provide iron, which normally comes from cell macrophages. Because of this, in order to grow Map cells in in vitro culture, they must be provided with mycobactin in the medium or they will not grow or reproduce [3]. This mycobactin deficiency can also be seen as a contributor to the bacteria’s slow growth rate [13].
Ecology
Map and protozoa. Many studies have been done to test the intracellular growth patterns of M. avium within environmental protozoan hosts. By interfering with the fusion of lysosomal and parasitophoric vacuoles within the protozoa, many bacteria are able to survive, if not thrive, within these organisms. It has been found that the uptake of M. avium by certain amoeba (for example Acanthamoeba castellanii) creates a protective barrier for the bacteria, keeping it safe from antibiotics and harsh environmental factors. Some pathogenic amoebae have the ability to traverse the intestinal epithelium; and thus can carry encapsulated mycobacteria along for the ride (for this reason, some have called this a Trojan horse relationship). The bacteria can be released and transported by the amoeba through cysts which are created on the outside of the protozoa and are carried by the wind. Further studies have found M. avium replication and virulence to be enhanced after growth inside amoebae. Though limited research has been done to test these relationships in Map, its similarities to M. avium create a good starting point. Studies have shown similar results for Map in lab cultures (protozoan engulfment leading to protection and enhanced survival), but have yet to test the interactions between protozoa and Map in the natural environment, where temperatures are lower and there may be other outside factors to take into account [13]. If, in further studies, this turns out to be a significant relationship, it will open the door for a new niche outside of the infected animal wherein Map can successfully replicate and be distributed [3].
Map, nematodes and insects. Studies have been done to test the interactions between Map and nematodes, earthworms, cockroaches, as well as Diptera (flies). All of these organisms live near and within possibly contaminated soil and faeces. Earthworms were found to have the smallest contribution to Map transfer because the bacteria could only survive within their systems for about two days. Map was found to be closely associated with nematode larval bodies, which are able to penetrate the gastrointestinal mucosa, creating a good means of transfer of environmental Map into host animals that eat the third stage larvae from the grass. Because of the hardy structure of the mycobacterial cell walls, Map is resistant to the digestive enzymes of insects which consume them, thus creating an additional pathway of infection. Diptera, which injest fluids from cut intestines in slaughterhouses which may be contaminated with Map, similarly were found important in the spread of Johne’s disease within infected herds [13].
Map and the environment. Though Map is an intracellular parasite which requires a host for replication and growth, it does not require a host for survival, and thus has been found in many areas of the environment and is highly resistant to many environmental conditions. It has been found to be prevalent in soil, pond water and pastures to which infected cattle may have access (for contamination by feces). A study in 1944 showed Map survival in outdoor manure to last 246 days. In water of pH 7.0 it lasted up to 17 months. Map is tolerant to high temperatures, which decreases the effectiveness of pasteurization to kill the organism in infected milk. Studies concerning Map resistance to ultraviolet (UV) light have resulted in uncertain and inconclusive results [3, 8]. So far, Map has not been isolated from any biofilm formations, but other mycobacteria have. Biofilms create a resistance to environmental stresses for all those organisms within the watery congregation, thus it is a good area for future research of Map ecology [13].
Pathology
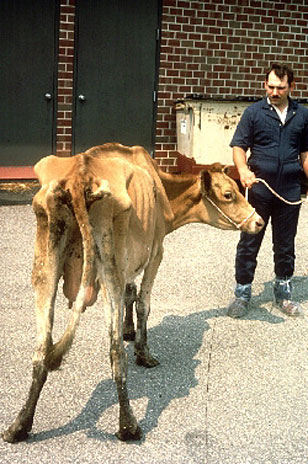
Mycobacterium avium subspecies paratuberculosis is pathogenic in mammals; it is the causative agent of Johne’s disease or paratuberculosis. Map primarily infects ruminants and pseduoruminants including but not limited to cattle, sheep, goats, dear, antelope, bison and llama [3]. Though it is most common found in these animals, it is definitely not restricted to these species, seeing that is has been found in many wild badger, fox, primates, rabbits, swine, and weasels [1, 8]. Infection has been found to readily spread between and across species with no restrictions, making the disease hard to control. Wild animals are proposed to be one method by which transfer of the Map bacterium occurs between farms or herds. Young animals are most susceptible to infection by Map because adults require a higher level of exposure to the bacteria in order to progress toward the disease [8]. Neonates are also at high risk of infection by their mother’s milk or contact with the bacteria during birth. Animals are most likely to be infected through the fecal-oral route due to contamination of water and food supplies by infected feces.
Johne’s disease progression has four stages: silent infection, subclinical, clinical, and advanced clinical disease. Once ingested, Map established itself in the lymphoid tissue of the upper gastrointestinal tract [1]. Clinical and visible manifestations of the disease will not be apparent for 1 to 10 years following infection, again making the disease hard to detect [2]. During that time, some of the Map is engulfed by epithelioid macrophages which elicit lymphocyte activation and clonal expansion. The immune system first responds with a Th1 response; a production of gamma interferon, interleukin 2, and tumor necrosis factor-alpha cytokines. This is followed by the Th2 response, wherein the animal begins to show nonspecific signs of disease, including weight loss and diarrhea despite a normal diet. These symptoms are due to pathogenic changes which occur throughout the disease progression. Proteins released from Map into the ileum lead to thickened and corrugated tissue as well as edematous lymph nodes. The inflammatory cells which respond to such an infection cause the intestinal wall to thicken until it can no longer function, thus leading to malabsorption and protein-losing enteropathy. Once animals have reached the advanced clinical phase, they usually die within weeks [8].
Because of non-specific clinical signs and long periods disease incubation withing the host animal, testing and management for control pose the greatest problem of this rapidly spreading disease. Diagnosis has been determined most effective when reviewing an entire herd rather than an individual by the pooling of clinical samples. All forms of testing unfortunately require a great amount of time and expense [2]. Vaccination has been deemed ineffective and economically impracticable [10]; though it can decrease the rate of disease, it cannot prevent infection and it has also been found to alter the results of tuberculosis testing, another major problem for cattle herds [2]. Though there is currently no cure for Johne’s disease, surveillance and control programs are being established throughout the globe that are committed to determining the location, species, familial links, and exposure history of any animals with confirmed disease in hopes to one day take control of this devastating disease and its etiologic agent Map [8].
Application to Biotechnology
Mycobacterium avium subspecies paratuberculosis has not been found to have any significance in biotechnology. Future research may prove otherwise.
Current Research
Map and Crohn's Disease
It is a debate which started in 1984, when a Mycobacterium similar to the agent of Johne’s disease was isolated and cultivated from the intestinal tissue of three patients with Crohn’s disease. Crohn’s disease is a chronic inflammatory bowel disease which currently is of unknown cause. The most widely accepted hypothesis is that Crohn’s disease occurs as a result of an abnormal immune response within the gastrointestinal mucosa. Ongoing studies have gone back and forth as to whether or not Map is a possible causative agent of Crohn’s. Theories include the presence of Map in Crohn’s patients, epidemiological similarities between the two diseases, as well as the response of Crohn’s patients to anti-microbial agents. So far, no conclusive evidence has proven either hypothesis (whether for or against Map in relation to Crohn’s) [12]. Current research in this area has been devoted to the possible transmission of the bacteria into humans through various means, including infected milk and meat. Seeing that dairy cows are the most commonly affected animals by Johne’s disease, the most likely method of transmission from animals to humans is through infected milk. Because of its high heat tolerance, though estimates of Map survival of HTST (high temperature short time) pasteurization is low, studies have shown occasional survivors [5]. A recent survey at the Dairy Food Safety Laboratory of the School of Veterinary Medicine at the University of California, Davis was done on ground beef to detect the presence of Map for human consumption. Map strains ATCC 43454 and ATCC 43544 were used along with a wild strain in a diluted broth to infect 200 ground beef samples. After analysis by PCR, all samples tested negative for the presence of Map [6]. Unfortunately, even if it can be proven that humans receive the pathogen from ruminant products, further research will be needed to substantially prove a bacterial cause for Crohn’s disease.
Methods of Detection
In order to get some sort of control over Johne’s disease throughout infected farms and to keep from spreading the disease further, efficient methods for environmental detection of Map must be determined and used consistently. There is currently a lack of reliable detection methods available for this purpose. A recent comparison of methods by the Department of Agriculture at Western Kentucky University suggests that the method of DNA extraction, sampling protocol and conditions of PCR all must be taken into account to confirm validity of the analysis in environmental samples. Within this testing, they compared DNA extraction by direct lysis of cells in situ to the cell extraction method in which cells are removed from the matrix prior to lysis and found the latter to result in higher DNA yields, shorter preparation times and higher concentrations of Map detected overall. They agreed with the commonly used sequence for targeting Map, IS900, since it turns out to be more sensitive than other targeted sequences as a result of having 14 to 20 copies throughout the genome. They also concluded that PCR conditions should include bead-beating to homogenize the sample and make all cells more readily available to lysis. With more efficient and consistent methods of real time PCR, environmental sources of Map can be investigated more effectively [4].
Molecular Basis of Pathogenesis
Despite the impact of Johne’s disease on the cattle industry in the United States, and its possible affiliations with Crohn’s disease, very little is known about the methods of pathogenesis of Map in its host animals. Investigators at the Laboratory of Bacterial Genomics of the Department of Pathobiological Sciences at the University of Wisconsin-Madison recently made the first effort to profile gene transcripts of Map following exposure to stressors (variances in acidity, temperature, and other such environmental alterations). A variety of clinical isolates and standard strains were used to find which genes were activated or deactivated as a result of each applied stressor. From this testing, they found, along with some unique activated gene sets, a set of genes that displayed consistent levels of transcription throughout each stressor, suggesting involvement in a universal mycobacterial response to certain conditions. Such ‘transcriptional profiling’ as it is named, can be used to detect the mechanisms used by Map to survive in certain conditions or to adapt to host cell medium in order to procure a solid establishment for pathogenicity, thus creating possibilities for infection control. Their testing resulted in the identification of a set of virulence genes which can become possible targets for disease treatment and a method which can be further utilized for other intracellular pathogens [14].
References
[ 1 ] Chacon, Ofelia; Bermudez, Luiz E.; and Barletta, Raul G. “Johne’s Disease, Inflammatory Bowel Disease, and Mycobacterium paratuberculosis.” Annual Reviews of Microbiology. 2004. 58: 329-63.
[ 2 ] Collins, Michael T. “Paratuberculosis: Review of present knowledge.” Acta veterinaria Scandinavica. 2003. 44: 217-221.
[ 3 ] Collins, Michael T. “Update on paratuberculosis: 1. Epidemiology of Johne’s disease and the biology of Mycobacterium paratuberculosis.” Irish Veterinary Journal. 2003. 56(11): 565-574.
[ 4 ] Cook, Kimberly L. and Britt, Jenks S. “Optimization of methods for detecting Mycobacterium avium subsp. paratuberculosis in environmental samples using quantitative, real-time PCR.” Journal of Microbiological Methods. 2007. 69: 154-160.
[ 5 ] Grant, Irene R. “Mycobacterium avium ssp. paratuberculosis in foods: current evidence and potential consequences.” International Journal of Dairy Technology. 2006. 59(2): 112-117.
[ 6 ] Jaravata, Carmela V.; Smith, Wayne L.; Rensen, Gabriel J.; Ruzante, Juliana; and Cullor, James S. “Survey of Ground Beef for the Detection of Mycobacterium avium paratuberculosis.” Foodborne Pathogens and Disease. 2007. 4(1): 103-106.
[ 7 ] Li, Lingling; Bannantine, John P.; Zhang, Qing; Amonsin, Alongkorn; May, Barbara J.; Alt, David; Banerji, Nilanjana; Kanjilal, Sagarika; and Kapur, Vivek. “The complete genome sequence of Mycobacterium avium subspecies paratubersulosis.” PNAS. 2005. 102(35): 12344-12349.
[ 8 ] Manning, Elizabeth J.B. “Mycobacterium avium subspecies paratuberculosis: a review of current knowledge.” Journal of Zoo and Wildlife Medicine. 2001. 32(3): 293-304.
[ 9 ] Marri, Pradeep Reddy; Bannantine, John P.; and Golding, Geoffrey B. “Comparative genomics of metabolic pathways in Mycobacterium species: gene duplication, gene decay and lateral gene transfer.” FEMS Microbiology Reviews. 2006. 30(6): 906-925.
[ 10 ] NCBI. “Mycobacterium avium subsp. paratuberculosis K-10 k10 project at Univ. Minnesota.” Entrez Genome Project.
[ 11 ] NCBI. “Mycobacterium avium subsp. paratuberculosis.” Taxonomy Browser.
[ 12 ] Prantera, C. “Mycobacterium and Crohn’s disease: The endless story.” Digestive and Liver Disease. 2007. 39: 452-454.
[ 13 ] Rowe, M.T. and Grant, I.R. “Mycobacterium avium ssp. paratuberculosis and its potential survival tactics.” Letters in Applied Microbiology. 2006. 42: 305-311.
[ 14 ] Wu, Chia-wei; Schmoller, Shelly K.; Shin, Sung Jae; and Talaat, Adel M. "Defining the Stressome of Mycobacterium avium subspecies paratuberculosis in Vitro and in Naturally Infected Cows." Journal of Bacteriology. 2007. Aug 10; [Epub ahead of print].
Edited by Kyla Holmes, student of Rachel Larsen
Edited by KLB
