Paramyxoviridae-Mumps Virus

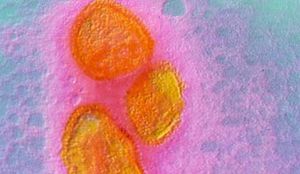
Etiology/Bacteriology
Taxonomy
| Order = Mononegavirales
| Family = Paramyxoviridae
| Subfamily = Paramyxovirina
| Genus = Rubalavirus
| species = Mumps Virus
|
ICTVdb: [3] |
Description
The mumps virus is a single-stranded, negative-sense RNA virus covered by a glycoprotein envelope. There are two glycoproteins on the RNA envelope: one regulates hemagglutinin-neuraminidase activity, the other is responsible for attachment to the lipid membrane of a host cell. This species of Rubalavirus can be found in host culture of saliva, urine, and cerebrospinal fluid. The mumps virus shares some epidemiological characteristics with other RNA viruses: measles and rubella. Humans are the only known hosts of this virus. It is an infectious disease that can be spread through direct contact of fluids, or via respiratory droplets from inhalation. Adults are usually affected more severely than children, but infection normally leads to lifelong immunity.
During a classic infection of mumps, 20-30% of cases are symptomatic and 30-40% of symptomatic cases experience pressure and pain from parotid gland inflammation. Gland inflammation can lead to parotitis. Mumps virus is the only known cause of epidemic parotitis. Possible additional symptoms of the mumps virus are fever, headache, weakness and fatigue, and loss of appetite [3]. Other complications from the mumps virus include encephalitis, aseptic meningitis, pancreatitis, orchitis, and deafness. Encephalitis, swelling of the brain, can become life-threatening. A vaccine for the mumps virus was produced in 1967, but outbreaks have continued to occur because of vaccination failure based on a single-dose regimen. Also, in the early 1970's most families with children and young adults did not consider the mumps vaccine a high priority [4]. In addition, people became unsure about the safety of the vaccine when it was thought to be linked to cases of autism.
Pathogenesis
Transmission
Mumps is extremely contagious and can spread rapidly among people living in close environments. Viral shedding occurs for a short time after initial infection through salivary droplets. The mumps virus is transmitted from person to person through infected saliva and sometimes through direct contact with surfaces, such as pillows and clothing that contain formites [5]. People without immunity can contract the virus by breathing in droplets of saliva from an infected person who sneezes or coughs. Mumps virus can linger on the surfaces of cups and utensils, leading to infection from the sharing of food and drink [3].
Infectious dose, incubation, and colonization
The TCID50 of mumps virus (50% tissue culture infectious dose) is 4.3 log 10 [6]. The incubation period of mumps ranges from 12-25 days, but the average is about 16-18 days. Fever can last for three to four days, and if parotitis occurs, usually lasts seven to ten days. A person is considered most infectious from one to two days before until five days after the symptoms of parotitis. Mumps mostly colonizes and replicates along the upper respiratory tract in the midst of a symptomatic infection [7]. After entering the respiratory system, the virus locally replicates. To target tissues of the salivary glands and central nervous system, viremic dissemination occurs. The virus replicates at target organs leading to a secondary phase of viremia before the immune response occurs. The virus also colonizes via blood transmission into the kidneys and other organs, possibly leading to renal impairment [4].
Epidemiology
Frequency
Since the introduction of the mumps vaccine in 1967, the number of mumps cases has dramatically decreased. In 1968 almost 155,000 cases were reported, but by 1998 there were only 666 reported cases of mumps. Currently, the number of recorded cases ranges from 200-250 in the United States. In 1990 there were 5,292 reported cases because children had only received one dose of vaccine, in contrast to the current recommendation of two doses. Only 57% of countries operating under the WHO have access to the mumps vaccine. Due to the variation in the number of people who receive the vaccine, it makes it difficult to estimate incidence and the number of cases in international regions. In 2005 there was an outbreak of mumps at a summer camp in New York that resulted in 32 cases. The people at camp were infected by an unvaccinated counselor that had traveled from the UK. In more recent years the amount of mumps cases has increased to several thousand due to outbreaks in highly populated environments for example, universities. These facts provide evidence that mumps outbreaks can occur among vaccinated people exposed to the mumps virus that is imported from a country with a continuous mumps epidemic. The risk of infection from a mumps virus from regions with mumps epidemics remains high [4].
Morbidity and Mortality
Although most patients with mumps fully recover, some fatal complications can arise. Without ready availability of the vaccination in some parts of the world, epidemics can still occur. The amount of deaths has decreased in association with mumps due to the great success of the vaccine, yet not all people choose to become vaccinated in countries where epidemics occur. There are approximately 1700 cases of mumps worldwide per year in people who are not vaccinated. The case fatality rate is 1 in 100,000 cases and the risk for encephalitis is 2 per 100,000 cases. The risk for deafness is 5 in 100,000 cases [8].
Virulence Factors
The double layered envelope surrounding the mumps virus is one of the highest contributing factors to its virulence, working through a series of proteins. The genome of the mumps virus contains 15,384 nucleotides that encodes seven genes: the nucleo-(N), the matrix (M), the fusion (F), the small hydrophobic (SH), the hemaglutinin-neuraminidase (HN), the V, and the large protein gene (L). Each of these genes codes for a single protein, except the V genes. The N protein covers the viral RNA as it is synthesized, creating the ribonucleoprotein (RNP). The RNA polymerase complex responsible for transcription, replication, and methylation capping consists of the N protein of RNP bound to the RNA-dependent RNA polymerase complex made of P and L proteins. A viral envelope encapsulate the mumps virus made up of the M protein on the internal surface, and F and HN proteins on the outer surface. One important role of the M protein is to assemble viral proteins for links between N proteins of the RNP and the tails of F and HN proteins. In addition, the M protein contributes to viral budding from infected cells. The HN and F proteins on the outer surface work in tandem to induce fusion of the host cell membrane and virion membrane to create cell-to-cell fusion after infection. To circumvent the IFN-mediated antiviral responses, the V protein limits IFN production and blocks IFN signaling. The small hydrophobic protein (SH) also contributes to the evasion of the host antiviral response by blocking the TNF-α-mediated apoptotic signaling pathway. The SH and V proteins are not essential to virus replication, and the I protein lacks a fundamental role concerning viral infection. Twelve genotypes have been designated to this virus: A-L. Other viral proteins in the genome of the mumps virus are not targets of a protective immune response. Their virulence roles remain obscure. To discriminate among mumps virus strains, nucleotide sequence analyses of N, H, P, F, and HN genes have been used. Most of their gene sequence is conserved though, making the discriminatory differences less noticeable. Both the F and HN proteins within the mumps genome have been identified as the primary virulence factors. Antibodies that target the F and HN proteins have provided definitive evidence of the neutralization of the infectivity of the virus in vitro and provide protection in vivo. [9].
Clinical Features
Most people that become infected with mumps fully recover. Although some people are asymptomatic there are general symptoms associated with mumps that usually develop within two weeks of infection. Normally the mumps virus causes fever, headache, muscle aches, malaise, loss of appetite, and swollen salivary glands. Complications from mumps usually occur in people past puberty. Complications can include inflammation of the testicles (orchitis) in 50% of post-pubertal males. Inflammation of the brain, encephalitis, and inflammation of the tissue covering the brain and spinal cord, or meningitis, can develop as well. Encephalitis is due to a primary infection of the neurons, or is caused by post-infection encephalitis with demyelination [4], [7]. Also, temporary or permanent hearing loss can result because of a vestibular reaction. In rare cases pancreatitis will manifest, but the patient often recovers within a week. Symptoms of pancreatitis include, abdominal pain, fever, nausea, and possibly vomiting[10].
The symptom most often associated with mumps is the swelling of the parotid gland that takes place over several days, otherwise known as parotitis [4]. Mumps has become an uncommon illness and is sometimes misdiagnosed with a high fever and swollen salivary glands that are actually indicative of tonsillitis [3]. If mumps occurs during pregnancy there is an increased risk of miscarriage, especially in the first 12-16 weeks. More mild symptoms that can accompany a case of mumps would be ear pain while chewing, a sour taste in the mouth while swallowing, joint ache, and mild nausea [11].
Diagnosis
Mumps can be diagnosed upon physical examination, especially if the patient has developed swollen glands. Laboratory test are often used to confirm and specify the viral strain of the diagnosis. In the laboratory, several tests can be used to identify the mumps virus. However, it is often difficult to use laboratories to confirm a mumps case in vaccinated individuals or repeat cases. In a case of mumps involving parotitis or pancreatitis, serum amylase levels are elevated. In the blood system, white blood cell levels can fluctuate, reflecting lymphocytosis. Elevated C-reactive protein or erythrocyte sedimentation rate (ESR) act as sera inflammatory markers that indicate a nonspecific systemic inflammatory response. In a general case of the mumps, viral particles can be detected in the urine in the first two weeks of sickness. Isolation of the mumps virus can also come from fluid from the oral cavity, nasopharyngeal swabs, and blood from seven days before and up to nine days after the onset of parotitis. In a cell culture the virus can be isolated from spinal fluid, urine or throat fluid. An assay of the CSF and polymerase chain reaction (PCR) assay can both detect mumps RNA, and gives a rapid confirmation for the diagnosis. In a case of mumps infection, diagnosis can be confirmed illustrating an increase in mumps-specific immunoglobulin G (IgG) antibodies. Processes used to detect IgG antibodies include, complement fixation, hemagglutinin inhibition, or enzyme immuno assay. The detection of IgM antibodies is a strong indicator of presence of the mumps virus as well. In some cases, interpretation of the mumps virus could cross-react with other parainfluenza viruses. Mumps cases involving meningitis or encephalitis often use computed tomography (CT) scanning to provide a more concise diagnosis [4], [7].
Treatment
Mumps is a self-limiting disease, therefore it will be resolved if proper medical care is taken in cases without complications. Current research shows that patients with mumps should be isolated for five days after the initiation of symptoms. For physical relief in mild to normal cases, increased fluid intake will allow the patient to stay hydrated with a fever [10]. Foods and liquids with high acidity are not recommended because they could be difficult to ingest and cause gastric irritation. Ibuprofen is prescribed to relieve pain from headaches and tenderness from parotitis. Repeated applications of warm or cold packs to swollen areas will help relieve additional discomfort. Hospital management is used to treat the more serious complications in association with mumps. Most of the time, complications are not life threatening, and with proper treatment can be resolved [4].
Prevention
If a person has previously been infected with mumps or received the vaccine, they are considered immune. In 1967 an effective vaccine was developed. Currently, this vaccine is delivered in combination with a vaccination against measles and rubella; known as the MMR inoculation. The mumps-measles-rubella-varicella vaccine is also administered, but poses a slightly higher risk of febrile seizures in children of 12-23 months than the MMR and varicella vaccines. For the most effective results, two doses of the vaccine are recommended. The first should be delivered between the ages of 12 and 15 months of age; the second should be delivered between the ages of four and six years old. If a child was not previously vaccinated then a dose should be administered between the ages of 11 and 12. The recommendation of a second dose of the vaccine was not common knowledge until the late 1980s. One vaccination does not offer effective protection during an outbreak. Yet, some people who previously received the first dose have failed, for numerous reasons, to receive a second dose. People who live or work in close quarters such as, hospitals and schools should receive the full vaccination. Otherwise, they risk a potential outbreak if the virus is circulating through the environment [3]. From a study in 2011, it was shown that people who received one dose of the vaccine had a 49-82% success rate of preventing the virus. While those who had received two doses of vaccine showed a 66-88% success rate of prevention. Based on this study, prevention is more effective with routine vaccination, especially in areas susceptible to outbreaks. This vaccine does not increase the risk of illness following a normal dosage. Autism and atypical bowel disease have been concerns associated with the administration of MMR, but have been disproven by reports from the CDC and the Institute of Medicine. Because of these pre-mature claims, vaccine coverage in certain countries has decreased, and measles eradication has been delayed [4], [13]. This vaccine is not recommended for people who are immuno-compromised by diseases like cancer of HIV. People who work in healthcare settings, or who attend universities, should provide documentation or act to receive the proper dosage of the vaccine [3], [7].
Host Immune Response
Studies on the host immune response are limited in comparison to measles and rubella infections. To control and defeat the mumps virus, the immune system combines cell-mediated and humoral immune responses. Paramyxoviruses must be controlled immediately at the onset of an infection because they replicate at a rapid rate. At the onset of infection, the host responds by activating the innate immune response, and produces natural killer cells to provide temporary defense against the virus. IgM antibodies are created in a measurable amount within a few days after symptoms occur. About three weeks after the initial symptoms IgG antibodies rise from low levels and increase to a maximum. It takes two to three months for IgG antibodies to return to a normal level. Salivary IgA bodies are produced in accordance with a mumps infection that gradually decrease after the initial onset of the illness. Overall, these antibodies neutralize the virus by binding and blocking access to target cells. Scientific studies have provided evidence supporting the production of these antibodies in response to a mumps infection. However, the specific details of the response of the humoral immune system to infection are still debated among scientists. Lymphocytes in the form of cytotoxic T cells have been observed to specifically target the mumps virus with a peak at two to four weeks after infection. Mostly, the host responds with a strong humoral response by proliferating T cells. Generally after a mumps infection, the host is endowed with long-lasting immunity. This is noted by the presence of hemaglutination-inhibiting antibodies detected after infection. The HN protein is a primary target for antibodies produced during a humoral immune response. It is difficult to measure cell-mediated response in the mumps virus because of T cell cross-reactivity that could occur among Paramyxoviridae species. In the host response though, an increase in CD 4 and CD 8 T cells has been proven in lab tests. Along with this increase in T cell proliferation, it has recently been illustrated that IL-10 increases when a host is infected with the virus. Some scientists argue that the IL-10 has been produced to counter-react against the virus' defense mechanism of IFN system suppression [12], [13].
References
1 University of Oklahoma Faculty and Staff.
2 NHS in the UK
3 "Diseases and Conditions Mumps" Mayo Clinic.
4 "Mumps" Medscape.
5 [ http://www.medicinenet.com/mumps/page2.htm#what_causes_mumps_how_is_mumps_ transmitted Mersch, J. "Mumps." MedicineNet.com.]
6 "Measles, Mumps, Rubella, and Varicella Virus Vaccine, Live" Drugs.com.
7 "Mumps." CDC.
8 "Disease Risk-Mumps." Smart Vax.
9 [ https://www.inkling.com/read/vaccines-plotkin-orenstein-offit-6th/chapter-22/chapter22-reader-2 Plotkin, S.A., Orenstein, W.A., Offit, P.A. Vaccines - Virology. Inkling.]
10 Krucik, G. "Mumps-Symptoms." Healthline.
11 "Mumps."WebMD.
12 [http://whqlibdoc.who.int/publications/2010/9789241500661_eng.pdf Mclean, H.Q., Hickman, C.J., Seward, J.F. "The Immunological Basis
for Immunization Series: Module 16: Mumps" WHO.]
13 [http://eprints.nuim.ie/156/1/Flynn%26Mahon2003.pdf Flynn, M., Mahon, B.P. "Cell Mediated And Humoral Immune
Responses To Mumps Virus:
Recent Developments." Mucosal Immunology Laboratory, Institute of Immunology, NUI.]
Created by Mary Kate Lowe
Student of Dr. Tyrrell Conway, University of Oklahoma
