Tea Tree Oil and its Effectiveness in Treating Acne Vulgaris
Propionibacterium acnes is a gram-positive species of bacteria that is found on most people's skin no matter if they exhibit signs of acne lesions or not. Recent studies indicate that traditional antibiotic treatment may not be as effective as it once was in treating acne vulgaris, and essential oils have been targeted as a potential antimicrobial treatment option. Specifically, the antimicrobial behavior of the hydrocarbon composition of tea tree oil (TTO) has been linked to the destruction of P. acnes in sebaceous glands beneath the surface of the skin.
Introduction to Acne Vulgaris
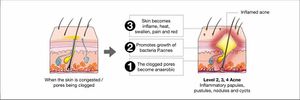
Acne vulgaris is a skin disease that affects more than half of the population at one point during their lifetime. Acne vulgaris may be most prevalent during adolescent years and development, however certain strains can persist through adulthood. The clinical features and prevalence of acne vulgaris have gained increased attention in more recent years. Acne vulgaris, or common acne, involves the pilosebaceous unit. Pilosebaceous units are hair follicles in the skin that are associated with an oil gland 12. Generally speaking, acne arises during puberty and resolves prior to adulthood. However, there are some variations or factors that persist long into adulthood.
Seborrhea, comedones, papules and pustules are clinical features that distinguish acne from other diseases 12. Seborrhoea is defined as excess grease while comedones are a result of a clogged hair follicle 12. Comedones are manifested as either blackheads or white heads and are distinguishable by whether or not they are covered or open. Lastly, papules and pustules are categorized as inflammatory lesions and constitute final clinical features of acne 12. Both are distinguished by an elevation of the skin and the production of pus.
Acne is typically found in parts of the body where there is a high density of pilosebaceous units 12. Specific body parts include the face, shoulders, back, neck, arms, and upper chest. The cause of acne can vary from one individual to the next and may include heredity, sweating, diet, the consumption of certain drugs, and can even be influenced by environmental conditions such as humidity 12.
There are multiple mechanisms by which acne lesions can be formed. Such mechanisms include the release of inflammatory mediators into the skin, changes in sebum production, a modification to the process leading to the formation of comedones, and a colonization of the bacteria species Propionibacterium acnes 12.
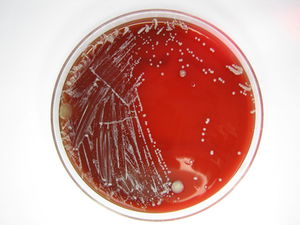
Propionibacterium acnes
The genome of Propionibacterium acnes was recently sequenced and reveals numerous proteins that assist P. Acnes in colonizing and residing in human skin under a variety of conditions 2.
Propionibacterium acnes is a gram-positive bacterium that prefers anaerobic growth conditions and is present on the skin of most individuals regardless of whether or not they have visible acne lesions 1. The transformation of the sebaceous gland into an acne lesion is the result of excessive sebum secretion. Acne lesions form when P. acnes gets trapped under the layers of sebum and begin to colonize the comedones 1. When P. acnes is trapped under layers of sebum and is unable to reach the surface of the skin, inflammation is more likely to occur. Researchers believe that P. acnes produces substances that are involved in the breakdown of the comedone lining and thus aide in the spread of bacteria from one comedone to the next 1. Following the breakdown of the comedone lining, P. acnes begins to secrete polypeptides and extracellular enzymes that play a role in the visible inflammatory response most often associated with acne vulgaris. The inflammatory response triggers a chain reaction in nearby sebaceous glands and P. acnes spreads.
Propionibacterium acnes and Antibiotic Resistance
Propionibacterium acnes is highly sensitive to a variety of antibiotics 5. The challenge in treating P. acnes with antibiotics is that the antimicrobial element must somehow pass through the lipid rich layers of the microcomedo that encapsulate the multiplying P. acnes 5.
Prior to the identification of clinically resistant strains of acne, drugs such as tetracycline and erythromycin were commonly administered modes of treatment 5. However, with the onset of topical antibiotic treatments, researchers noted the steady increase in resistant strains of P. acnes in multiple countries 5. In the general study of the antibiotic resistance of P. acnes, no mobile genetic elements have been identified as playing a role in the efflux of antibiotics away from the bacterial strain 5. On the other hand, researchers have noted that the resistance of P. acnes to certain antibiotics can be attributed to point mutations in the genes of the bacteria that code for the 23S rRNA and 16S rRNA subunits 5. Resistance to specific antibiotic acne treatments is determined by the specific location of base-pair mutations in the encoding genes 5. For example, resistance to the drug erythromycin is attributed to mutations in genes encoding the 23S rRNA subunit while mutations in the genes encoding the 16S rRNA subunit are associated with resistance to the drug called tetracycline 5.
Background Information: Tea Tree Oil

Many essential oils have been found to have antimicrobial and antioxidant properties 8. Of these essential oils, tea tree oil (TTO) may be one of the most widely studied due to its broad spectrum of known activities 8. Tea tree oil comes from Melaleuca alternifolia, a tree species that is native to Australia. The Melaleuca genus has over 230 species 3. In its natural habitat of swampy, subtropical, coastal ground, the M. alternifolia tree grows approximately 5 to 8 meters and produces white fluffy flowers like the one pictured to the left 3. Via a steam distillation process, the tea tree oil can be isolated from the leaves, twigs, and branches of M. alternifolia 9.
Component Properties of Tea Tree Oil
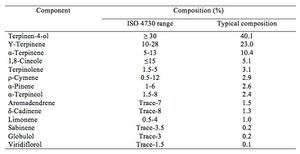
Tea tree oil is mainly comprised of terpene hydrocarbons 9. Furthermore, tea tree oil is made up of over 100 components that aid in its antimicrobial and antioxidant capabilities. Some of these components include, monoterpenes, sesquiterpenes, and their alcohol derivatives 8.
According to the International Organization for Standardization (ISO) 4730 guidelines, the various components of tea tree oil must be defined and should not exceed certain percentage parameters. Since tea tree oil (TTO) can vary from one batch to the next, the international guidelines set both physical and chemical criteria for each desired chemotype of tea tree oil 3. For example, the ISO guidelines dictate that 14 components make up the composition of M.alternifolia (tea tree) oil as is depicted in the chart to the right. For this particular chemotype of tea tree oil, the concentration of terpinen-4-ol should exceed 30% while the concentration of 1,8-cineole should not exceed 15% 9. However, more than just the components terpinene-4-ol and 1,8-cineole make up tea tree oil. Lee and colleagues (2013) note that the composition of devised tea tree oil formulas have included ϒ-Terpinene, α-Terpinene, ρ-Cymene, α-Pinene, and α-Terpineol.
The tea tree oil most commonly used in commercial production is called terpinen-4-ol chemotype 3. The antimicrobial activity of tea tree oil is most often associated with the terpinen-4-ol component 3.
The Effects of Tea Tree Oil in the Treatment of Acne
As was previously mentioned, the over activation of Propionibacterium acnes results in the formation of inflammatory responses visible on the surface of the skin. Typically, doctors would prescribe antibiotic medication in order to suppress and control the clinical features of acne 9. Examples of such antibiotics include neomycin, tetracycline, and erythromycin 9.
However, in recent years, the emergence of new antibiotic resistant strains has limited the effectiveness of antibiotics in their ability to suppress and treat Propionibacterium acnes 6. Alternative medicines, such as essential oils, have been studied in recent years in order to determine an alternative mechanism by which to combat the symptoms of over activation of P. acnes. Essential oils provide a possible alternative to antibiotic treatment of acne because they have been shown to have antimicrobial and anti-inflammatory responses 9. The medicinal properties of tea tree oil were first discovered in the 1920s by a researcher named Penfold who was conducting a survey of Australia's essential oils with the most economic potential 3.
Previous studies have indicated significant differences in the efficacy of tea tree oil compared to placebos and other traditional antibiotic treatments. The percentage of components of each tea tree oil formula can be adjusted to demonstrate varying efficacy against P. acnes. Previous studies have indicated that skin irritation and other side effects can result from varying degrees of percentage components as well as prolonged exposure 9.
The Antimicrobial Behaviors of Tea Tree Oil
Researchers note that the concentration of tea tree oil plays a role in its antimicrobial activity. Prior to the availability of extensive data collection, assumptions regarding the antimicrobial behavior of tea tree oil were made based on its hydrocarbon structure 3. Based on the typical behavior of hydrocarbon structures, Sikkema and colleagues (1995) noted that the hydrocarbons from the tea tree oil gather in the membrane lipid bilayer of the target bacteria. The binding of the hydrocarbons to the membrane of the bacteria disrupts the structure and function of the target bacterium's membrane, in this case, the membrane of Propionibacterium acnes. The altered state of the bacterium's membrane results in the altered movement of protons and membranes across the membrane, thus disrupting the internal homeostasis and the proper function of the membrane proteins 11. Overall, after coming into contact with the components of the tea tree oil, the Propionibacterium acnes cells lose their intracellular material, are unable to maintain internal homeostasis, and their respiration is inhibited 3. Contact with the components of the tea tree oil inhibit the proper functioning of the P. acnes cells.
While further research is necessary in order to more adequately understand the specific antimicrobial mechanism of tea tree oil in relation to Propionibacterium acnes, the basic antimicrobial behaviors of tea tree oil can be understood in terms of the behavior of hydrocarbon structures.
Specific Studies Pertaining to the Efficacy of Tea Tree Oil
Perhaps one of the most well studied antimicrobial activities include that of the tea tree oil component called terpinen-4-ol 9. In their study conducted in 2013, Chia-Jung Lee and colleagues performed an agar well diffusion test in order to determine the minimum inhibitory concentrations of multiple components of tea tree oil, and their effectiveness in suppressing acne. Agar media containing bacterial growth were placed in a petri dish and stainless steel cylinders were dispersed throughout the dish creating wells 9. Among the components that make up tea tree oil, researchers found that terpinen-4-ol, α-terpineol, α-terpinolene, and α-terpinene demonstrated the greatest antimicrobial activities 9. This is evident in the diameter of their inhibition zone and their minimum inhibitory concentration. A specific composition of tea tree oil was created that contained both terpinen-4-ol and 1,8-cineole in varying percentages, and their efficacy and antimicrobial activities were monitored 9. Results indicated that the terpinen-4-ol component of tea tree oil had a greater antimicrobial efficacy compared to that of 1,8-cineole 9.
Additional studies have analyzed the effects of tea tree oil on acne treatment. In particular, via a double-blind placebo controlled study, Enshaieh and colleagues (2007) found that 5% tea tree oil demonstrated a significant effect in reducing both the inflamed and non-inflamed lesions indicative of acne. The effect of tea tree oil, or other treatments, on acne vulgaris can be measured by assessing the total acne lesion count (TLC) or the acne severity index (ASI) 6. Following treatment with tea tree oil, Enshaieh and colleagues (2007) observed that the mean total lesion count (TLC) reduced by 43.64% following treatment with tea tree oil, thus making the efficacy of tea tree oil significantly different from that of the placebo treatment. Furthermore, tea tree oil was found to reduce the mean acne severity index (ASI) by 40.49% while the placebo group demonstrated a 7.04% reduction of ASI 6.
Further Reading
As was previously mentioned, Carson and colleagues (2006) noted that more recent data demonstrates the antibacterial, antiviral, antifungal, and antiprotozoal activities of tea tree oil. However, the activity of the components of tea tree oil have not been thoroughly studied in in vitro, due in part to the barriers established by the physical components of the oil. Namely, the components of tea tree oil are not very soluble in water 3. Thus, their minimal solubility limits tea tree oil components' ability to mix thoroughly in test media and agar broths. This physical property impedes the proper evaluation of tea tree oil's antimicrobial activity to a certain extent. While efforts have been made to minimize these problems, still more work is needed to eliminate the problem all together.
Furthermore, while this subsection was not of particular focus on this page, it is important to understand the possible outcomes of the interaction between tea tree oil and antibiotics. In order to more fully understand the potential benefits of tea tree oil in the treatment of Acne Vulgaris, one may want to more fully understand the mechanisms by which the components of tea tree oil may interfere with antibiotic treatment and the effects this has on the growth of Propionibacterium acnes.
References
4. Cellnique Cosmaceutical. (17 March 2010). Cellnique- About Acne. Animation.
7. Gerus, Tatiana. (11 October 2009). Snow in Summer. Photograph.
10. Mostly*harmless. (27 August 2013). Propionibacterium acnes. Photograph.
12. Williams, H.C., Dellavalle, R.P., & Garner, S. (2012). Acne Vulgaris. Lancet, 379, 361-371.
Edited by Alex Sheridan, a student of Nora Sullivan in BIOL168L (Microbiology) in The Keck Science Department of the Claremont Colleges Spring 2014.
