User:MorrisonK
A Microbial Biorealm page on the genus MorrisonK
Classification
Higher order taxa
Bacteria; Proteobacteria; Gammaproteobacteria; Pseudomonadales; Moraxellaceae [Others may be used. Use NCBI link to find]
Species
|
NCBI: Taxonomy |
Moraxella catarrhalis
Description and significance
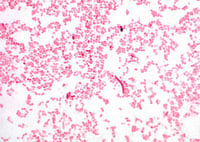
M. catarrhalis is a gram-negative, non-motile un-capsulated diplococcus. Upon its discovery in 1896 it was given the name Micrococcus catarrhalis and then later renamed Neisseria catarrhalis because of its phenotypic and genetic transformation similarities with the genus Neisseriaceae (7). In 1963, scientists realized that Micrococcus catarrhalis consisted of two distinct species and N. catarrhalis was moved to the genus Branhamella. With the genus Moraxellaceae created in the late 1970s consisting of two subgenera Moraxella (Moraxella) and Moraxella (Branhamella), B. catarrhalis switched to a new genus in 1984 (7). The reassignment of genus changed the bacteria’s name to Moraxella (Branhamella) catarrhalis.
M. catarrhalis is considered to be part of the human resident flora in the mucosal epithelial cells of the upper respiratory tract, specifically the nasopharynx (10). In its natural habitat M. catarrhalis is nonpathogenic. However, its presence in the ear and/or contact with other pathogenic bacteria can cause respiratory and ear infections.
Genome structure
M. catarrhalis is characterized by a single chromosome containing 1,863,286 nucleotides with an overall G+C content of 41.7% (2). 1,964 genes are coded for in the chromosome with 1,886 of these being protein-coding genes. Of the 1,886 protein-coding genes only 63.6% are determined to be functional and 172 of these functions are unknown (2). Non-protein coding genes code for four identical rRNA operons and 50 tRNA’s to synthesize all twenty amino acids. M. catarrhalis has alternative mechanisms for adapting gene expression to changing environmental conditions. The chromosome is able to change to phase-variable expression or noncoding RNA based regulation when placed in unfavorable conditions (2).
Cell structure and metabolism
M. catarrhalis is a gram-negative, motile, pathogenic diplococcus. Its cocci morphology differs itself from the rest of the species in the Moraxella genus (9). It is an obligate aerobe; however, it lacks genes for certain oxidative metabolism stages. M. catarrhalis lacks genes encoding for carbohydrate transport and catabolism components of metabolism and there is also an incomplete glycolytic pathway (2). The TCA cycle lacks important subunits for succinyl-CoA synthetase. M. catarrhalis has all genes for long-chain fatty acids beta oxidation. Iron is a necessary cofactor for metabolism and is brought into the cell through specific protein components for acquisition and transport (2). Enzymes for oxidative stages of pentose phosphate pathway are not present in all strains, but enzymes for the non-oxidative branch of the pentose phosphate pathway are present (2). Similarly there is difference in strains though production of catalase enzymes (2).
Recent research indicates that M. catarrhalis may have a predicted truncate denitrification pathway (10). M. catarrhalis forms biofilms and nitrite is an important component of this biofilm formation. Since nitrite is essential, growth does not occur in the presence of low nitrite concentrations. While nitrite is necessary for growth, reduction of nitrite to nitric oxide is potentially toxic (10).
Ecology
M. catarrhalis is present in the natural flora of the human upper and lower respiratory tract. M. catarrhalis is especially predominant in the nasopharynx region of the upper respiratory tract (3). If kept in check by other bacteria, M. catarrhalis is not harmful. However, it is a human pathogen causing infection if population exceeds normal limits in the respiratory tract or by migration to middle ear (10).
Pathology
M. catarrhalis is a human pathogen best known for causing otitis media in infants and children. Approximately 15-20% of acute otitis media cases are caused by M. catarrhalis annually (5). Other related infections include otitis media with effusion and chronic obstructive pulmonary disease, COPD. The pathway leading to infection is still under investigation but is related to the ability to form biofilms (5). In order to begin an infection that leads to otitis media, M. catarrhalis migrates from the nasopharynx to the middle ear through the eustachian tube (5). The migration of the bacteria does not start the infection; instead upon arrival in the middle ear M. catarrhalis must meet with a preceding viral infection to make the bacteria pathogenic.
Virulence factors are still under active investigation. There are ubiquitous surface proteins that mediate binding to epithelial cells and extracellular matrix (2). Binding allows the bacteria to anchor to the environment before starting an infection. Recent research indicates that a type-IV pilus subunit PilA contributes to pathogenic mucosal colonization of M. catarrhalis (4). A specific protein on the membrane surface is the CD protein also contributes to the pathogenic nature of the bacteria. The CD protein attaches to a mucin molecule in both the nasopharynx and middle ear allowing the bacteria to stay in its environment (8). Not a lot is known of the mechanisms for infection but M. catarrhalis is significantly less toxic if lipooligosaccharides are not present on the membrane surface (6).
Otitis media patients have clinically milder systems when M. catarrhalis is the causing agent for the infection. Patients tend to have a lower fever and have a lower likelihood of observing a red bulging tympanic membrane. COPD patients have exacerbations associated with emergency room visits and hospital admissions, lost work time, respiratory failure and death (5). Patients experience fever, sputum production, sputum purulence and dyspnea (5). A chest examination reveals rhonchi and generalized decreased air entry in the bronchi.
Current Research and or Application to Biotechnology
In January of 2011, Nicole R. Luke-Marshall, Shauna L. Saubera, and Anthony A. Campagnari performed an experiment to determine how M. catarrhalis effectively colonized and established an infection through the expression of type IV pili (TFP) (4). The research aimed at showing that this specific pili is critical for M. catarrhalis becoming pathogenic. They discovered that unlike the similar Neisseria species, this pilin subunit is highly conserved. There are no major pilin variants between strains and only two major PilA antigenic variants were observed in M. catarrhalis strains (4). The lack of pilin variants shows the importance of the type IV pili (TFP) and the role of PilA in infectious colonization. If therapeutic or vaccine-based interventions focused on this specific surface subunit, acute and recurrent M. catarrhalis infections would likely decrease. From this realization, the researchers concluded that additional studies aimed at elucidating the role of PilA in M. catarrhalis become pathogenic are warranted (4).
Wei Wang, Traci Kinkel, Willm Martens-Habbena, David A. Stahl, Ferric C. Fang, and Eric J. Hansen examined the nitrite reductase genes of M. Catarrhalis in June, 2011 (10). Previous research showed that the genome encodes a predicted truncated denitrification pathway reducing nitrate to nitrous oxide. Expression of the M. catarrhalis aniiA, gene encoding for nitrite reductase, and M. catarrhalis norB, gene encoding a putative nitric oxide reductase, is repressed by transcriptional regulators during aerobic conditions (10). Similarly strains with mutants of this transcriptional regulator, nsrR, are unable to grow in the presence of low concentrations of nitrite. They showed this inability to grow by constructing a norB mutant to determine if growth was inhibited with or without the nsrR mutant. Growth did not occur in the norB mutant as it was unable to reduce nitric oxide and produced little or no nitrous oxide from nitrite (10). These results suggested that that nitric oxide catabolism in M. catarrhalis is primarily an accomplishment of the norB gene.
Todd Hoopman, in September 2011, studied nasopharyngeal colonization of M. catarrhalis to study gene expression in chinchillas (3). While M. catarrhalis is strictly a human pathogen, it did grow in chinchillas which allowed experimenters to examine the species without infection. This study allowed for more detailed analyses of gene expression when the bacteria are subjected to physiological stresses and immune response systems (3). Recent efforts of mining the genome revealed presence of numerous genes encoding proteins with signal sequences that become surface signals or are secreted into the environment. These proteins and signal sequences could help explain the mechanisms by which M. catarrhalis begins an infection (3).
References
1. Chapter 35 antibacterial drugs. (n.d.). Retrieved from http://www.pharmacology2000.com/Antibacterial/antibactobj.htm
2. de Vres, S., van Hijum, S., Schueler, W., Riesbeck, K., Hays, J., Hermans, R., and Bootsmai, H. (2010). Genome analysis of Moraxella catarrhalis strain RH4, a human respiratory tract pathogen. Journal of Bacteriology 192(14), 3574-3583.
3. Hoopman, T. (2011). Use of the chinchilla model for nasopharyngeal colonization to study gene expression by moraxellai catarrhalis. Infection and Immunity, 80(3), 982-995.
4. Luke-Marshall, N., i, S., and Campagnari, A (2011). Comparative analyses of the Moraxella catarrhalis type-IV pilus structural subunit PilA. Gene, 477, 19-23.
5. Murphy, T., and Parameswaran, G. (2009). Moraxella catarrhalis, a human respiratory tract pathogen.Clinical Practice, 49, 124-131.
6. Peng, D., Hong, W., Choudhury, B., Carlson, R., and Gu, X (2005). Moraxella catarrhalis bacterium without endotoxin, a potentiala vaccine candidate. Infection and Immunity, 73(11), 7569-7577.
7. Rossau, R., Van Landschoot A., Gillis, M., and De Ley, J. (1991). Taxonomy of Moraxellaceae fam. nov., a new bacterial family to accommodate the genera Moraxella, Acinetobacter, and psychrobacter and relate organisms. International Journal of Systemic Bacteriology,41(2), 310-319.
8. Verduin, C., Hol, C., Fleer, A., van Dijk, H., and van Belkum, A (2002). Moraxella catarrhalis: From emerging to established pathogen.Clinical Microbiology Reviews, 15(1), 125-144.
9. Vroides, A., Dagan, R., Greenberg, D., Givon-Lavi, N., and Leibovitz, E. (2009). Acute otitis media caused by Moraxella catarrhalis epidemiologic and clinical characteristics. CID, 49, 1641-1647.
10. Wang, W., Kinkel, T., Martens-Habbena, W., Stahl, D., Fang, F., and Hansen, E (2011). The Moraxella catarrhalis nitric oxide reductase is essential for nitric oxide detoxification. Journal of Bacteriology, 193(11), 2804-2813.
Edited by student of Dr. Lynn M Bedard, DePauw University http://www.depauw.edu