Microbial Infection of Burn Wounds: Difference between revisions
| Line 20: | Line 20: | ||
<br>Besides those that confer antibiotic resistance, MRSA virulence factors include adhesion proteins, colonization proteins, superantigens, exotoxins, and pore-forming toxins. Adhesion proteins allow MRSA to adhere exceptionally well to host tissues, which makes it difficult for the body to clear the pathogens. Colonization proteins help the bacteria to compete more effectively with other bacteria, both within their own species and with others. Some of these proteins also increase salt tolerance which could be beneficial in instances of infection where low perfusion results in high external osmolarity, such as in burn wounds. Superantigens instigate an elevated immune response in the body, sometimes up to 20% greater than would be triggered by bacteria not in possession of this virulence factor. This is particularly dangerous for patients because it can cause high fevers, shock, multiple organ failure and/or toxic shock syndrome. Pore-forming toxins can lead to vascular leakage, hypovolemic shock and tissue necrosis [Zetola]. It is for these reasons that MRSA infections are so dangerous to patients whom are already immuno-compromised.<br> | <br>Besides those that confer antibiotic resistance, MRSA virulence factors include adhesion proteins, colonization proteins, superantigens, exotoxins, and pore-forming toxins. Adhesion proteins allow MRSA to adhere exceptionally well to host tissues, which makes it difficult for the body to clear the pathogens. Colonization proteins help the bacteria to compete more effectively with other bacteria, both within their own species and with others. Some of these proteins also increase salt tolerance which could be beneficial in instances of infection where low perfusion results in high external osmolarity, such as in burn wounds. Superantigens instigate an elevated immune response in the body, sometimes up to 20% greater than would be triggered by bacteria not in possession of this virulence factor. This is particularly dangerous for patients because it can cause high fevers, shock, multiple organ failure and/or toxic shock syndrome. Pore-forming toxins can lead to vascular leakage, hypovolemic shock and tissue necrosis [Zetola]. It is for these reasons that MRSA infections are so dangerous to patients whom are already immuno-compromised.<br> | ||
===<i>Pseudomonas | ===<i>Pseudomonas areuginosa</i>=== | ||
<br><i>P. aeruginosa</i> are the most common source of burn infections [Church]. They are gram-negative bacilli that possess a single supercoiled circular chromosome. <i> P. aeruginosa</i> are facultative aerobes capable of fermentation that live in the human gut. These bacteria are known for their tendency to cause disease in immuno-compromised patients, such as those with AIDS or cystic fibrosis, but rarely in healthy individuals [Lyczak].<br> | <br><i>P. aeruginosa</i> are the most common source of burn infections [Church]. They are gram-negative bacilli that possess a single supercoiled circular chromosome. <i> P. aeruginosa</i> are facultative aerobes capable of fermentation that live in the human gut. These bacteria are known for their tendency to cause disease in immuno-compromised patients, such as those with AIDS or cystic fibrosis, but rarely in healthy individuals [Lyczak].<br> | ||
<br>These microbes use quorum sensing to form biofilms and induce the production of virulence factors such as proteases, hemolysins, exotoxin A and pyocyanin [Lyczak; Van Deldyn]. <i>P. aeruginosa</i> posses two quorum-sensing systems: one that regulates proteases and another that regulates hemolysins. Though separate systems, the two interact through products of the protease system controlling the hemoysin system at both transcriptional and posttranslational levels [Van Deldyn]. Proteases degrade the integrity of the host’s physical barriers by splitting proteins and amino acids, allowing for deeper infiltration of infection [Lyczak]. Exotoxin A halts the synthesis of proteins, causing local tissue damage, immunosuppression and cell death [Van Delden]. Hemolysins act like detergents to break down lipids in epithelial cells allowing, like the proteases, the bacilli to penetrate the host resulting in the spread of infection [Van Deldyn]. In addition, genes encoding proteins for pili and flagella are also important to <i>P. aeruginosa</i> since without these structures, bacteria are unable to navigate their environment and form biofilms [Lyczak]. <i>P. aeruginosa</i> infections are difficult to treat because these microbes possess multiple strategies for eluding predators, including multidrug efflux pumps, antibiotic-modifying enzymes, and tough outer membranes with low permeability [Van Delden].Therefore, the best way to treat these infections is to head them off early by interfering with cell-to-cell signaling [Van Delden].<br> | <br>These microbes use quorum sensing to form biofilms and induce the production of virulence factors such as proteases, hemolysins, exotoxin A and pyocyanin [Lyczak; Van Deldyn]. <i>P. aeruginosa</i> posses two quorum-sensing systems: one that regulates proteases and another that regulates hemolysins. Though separate systems, the two interact through products of the protease system controlling the hemoysin system at both transcriptional and posttranslational levels [Van Deldyn]. Proteases degrade the integrity of the host’s physical barriers by splitting proteins and amino acids, allowing for deeper infiltration of infection [Lyczak]. Exotoxin A halts the synthesis of proteins, causing local tissue damage, immunosuppression and cell death [Van Delden]. Hemolysins act like detergents to break down lipids in epithelial cells allowing, like the proteases, the bacilli to penetrate the host resulting in the spread of infection [Van Deldyn]. In addition, genes encoding proteins for pili and flagella are also important to <i>P. aeruginosa</i> since without these structures, bacteria are unable to navigate their environment and form biofilms [Lyczak]. <i>P. aeruginosa</i> infections are difficult to treat because these microbes possess multiple strategies for eluding predators, including multidrug efflux pumps, antibiotic-modifying enzymes, and tough outer membranes with low permeability [Van Delden].Therefore, the best way to treat these infections is to head them off early by interfering with cell-to-cell signaling [Van Delden].<br> | ||
Revision as of 01:21, 16 April 2009
By Erin Pienciak
Overview of Burns
Burns are damage to the skin caused by chemicals, electricity, heat, sunlight or nuclear radiation [ ]. Overall burn severity is determined based on the degree of tissue damage and the size of the area affected.
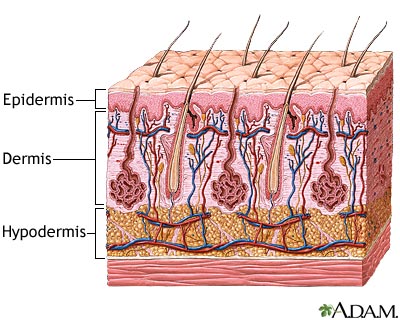
The tissue damage incurred is classified into three categories: first, second and third-degree burns [ ]. First-degree burns involve only damage to the topmost layer of the skin, the epidermis. Second-degree burns contain damage to the epidermis as well the dermis, the underlying layer of the skin. Third-degree burns refer to damage or destruction of the entire depth of the skin as well as tissues that lie beneath it. These are three-dimensional injuries with damage extending in all direction from the center of the injury.
The area of a burn is often determined using the “Rule of Nines,” which divides the body up into sections that correspond with approximately 9% of the body’s surface area [ ]. For example, an arm, the abdomen and the entire head each account for 9%. If all three of these body parts were burned, it would be estimated that the patient sustains injuries to 27% of his body.
Burns wounds have three separate zones of concern. The zone of coagulation is located where the skin came in contact with the burn source, at the center of the wound. It is made up of dead, leathery tissue that forms the burn eschar, or scab. The zone of stasis surrounds the zone of coagulation; tissue is this zone is alive but at a high risk of infection and necrosis due to decreased perfusion to the area. Lastly, the zone of hyperemia surrounds the zone of stasis and contains healthy skin though vasodilatation in this area is common as a result of the injury [Church].
Infection of burns is common because the skin, a physical barrier against microbes, has been compromised. Furthermore, in moderate and severe burns the underlying vasculature of the skin has been damaged or destroyed and so immunity agents, such as T cells, cannot reach sites of infection. Accordingly, the risk of infection increases proportionately with the size of the burn [Church].
Burn Infections
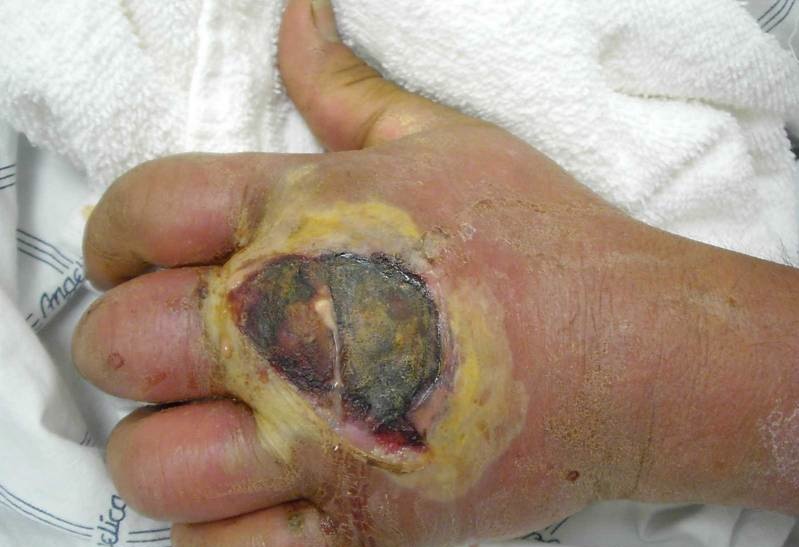
Burn wound infection is problematic because it delays healing, encourages scarring and may result in bacteremia, sepsis or multiple-organ dysfunction syndrome (a.k.a. organ failure) whereby organs from several systems are unable to maintain homeostasis on their own, requiring immediate medical attention [Church].
Bacteria and fungi are the most common pathogens of burn wounds. These microbes form multi-species biofilms on burn wounds within 48 – 72 hours of injury [Church]. Organisms originate from the patient’s own skin, gut and respiratory flora, as well as from contact with contaminated health care environments and workers [Church; Murray]. Gram-positive bacteria are some of the first to colonize burns, followed quickly by gram-negative . Fungal infection tends to occur in the later stages after the majority of bacteria have been eliminated by topical antibiotics [Church]. Two bacterial species, methicillin-resistant Staphylococcus aureus (MRSA) and Pseudomonas areuginosas will be examined in depth in this page as they are two of the most prevalent infective agents. These two species have proven particularly difficult to treat because they posses a large number of virulence factors and antimicrobial resistance genes.
methicillin-resistant Staphylococcus aureus
MRSA are gram-positive, spherical microbes and some of the earliest colonizers of burn wounds. Their genome is contained on one circular chromosome, with antibiotic resistance encoded in transposons. MRSA dwell in the sweat glands, hair follicles and mucous membranes of humans.
Staphylococcus aureus resistance to methicillin and other similar antibiotics is due to the altered structure of penicillin binding proteins. This mutation is caused by resistance genes that are carried in the staphylococcal cassette chromosome (SCC) mec, a mobile genetic element. The cassette encodes for an insertion sequence element, recombinases and regulatory genes. Five versions of SCCmec have been identified, each of which confers resistance to slightly different sets of agents [Zetola].
Besides those that confer antibiotic resistance, MRSA virulence factors include adhesion proteins, colonization proteins, superantigens, exotoxins, and pore-forming toxins. Adhesion proteins allow MRSA to adhere exceptionally well to host tissues, which makes it difficult for the body to clear the pathogens. Colonization proteins help the bacteria to compete more effectively with other bacteria, both within their own species and with others. Some of these proteins also increase salt tolerance which could be beneficial in instances of infection where low perfusion results in high external osmolarity, such as in burn wounds. Superantigens instigate an elevated immune response in the body, sometimes up to 20% greater than would be triggered by bacteria not in possession of this virulence factor. This is particularly dangerous for patients because it can cause high fevers, shock, multiple organ failure and/or toxic shock syndrome. Pore-forming toxins can lead to vascular leakage, hypovolemic shock and tissue necrosis [Zetola]. It is for these reasons that MRSA infections are so dangerous to patients whom are already immuno-compromised.
Pseudomonas areuginosa
P. aeruginosa are the most common source of burn infections [Church]. They are gram-negative bacilli that possess a single supercoiled circular chromosome. P. aeruginosa are facultative aerobes capable of fermentation that live in the human gut. These bacteria are known for their tendency to cause disease in immuno-compromised patients, such as those with AIDS or cystic fibrosis, but rarely in healthy individuals [Lyczak].
These microbes use quorum sensing to form biofilms and induce the production of virulence factors such as proteases, hemolysins, exotoxin A and pyocyanin [Lyczak; Van Deldyn]. P. aeruginosa posses two quorum-sensing systems: one that regulates proteases and another that regulates hemolysins. Though separate systems, the two interact through products of the protease system controlling the hemoysin system at both transcriptional and posttranslational levels [Van Deldyn]. Proteases degrade the integrity of the host’s physical barriers by splitting proteins and amino acids, allowing for deeper infiltration of infection [Lyczak]. Exotoxin A halts the synthesis of proteins, causing local tissue damage, immunosuppression and cell death [Van Delden]. Hemolysins act like detergents to break down lipids in epithelial cells allowing, like the proteases, the bacilli to penetrate the host resulting in the spread of infection [Van Deldyn]. In addition, genes encoding proteins for pili and flagella are also important to P. aeruginosa since without these structures, bacteria are unable to navigate their environment and form biofilms [Lyczak]. P. aeruginosa infections are difficult to treat because these microbes possess multiple strategies for eluding predators, including multidrug efflux pumps, antibiotic-modifying enzymes, and tough outer membranes with low permeability [Van Delden].Therefore, the best way to treat these infections is to head them off early by interfering with cell-to-cell signaling [Van Delden].
Treatment
Burn patients have a uniqe set of requirements while recovering from their trauma. Of the utmost importance is airway, breathing and circulation maintenance. Patients may have sustained inhalation injuries when they were burned and thus could require additional interventions. Hemodynamic homeostasis can also be problematic as a result of disrupted blood flow and fluid loss. Furthermore, the metabolism of burn victims actually increases in response to the injury and so nutritional intake must increase accordingly [Church]. Interestingly, meeting the nutritional needs of gastrointestinal flora can help mitigate wound infection because they do not need to go in search of a food source. All of these issues can affect temperature regulation, so care must be taken that a patient stays within normal limits. Pain management also needs to be considered. These issues must be addressed before the burn itself can be treated.
Traditional
Currently, the most widely accepted methods of treatment of moderate and severe burns include wound excision and the application of topical antimicrobial agents [Church]. The presence of the eschar tends to produce localized inflammation. The purpose of excision is to surgically remove the eschar, thereby reducing inflammation and minimizing scaring. The wound can then be debrided, cleansed and closed using a skin graft or a synthetic alternative [Church].
In order to not encourage resistance, topical antimicrobials must be specific to the species colonizing a wound. Species can be discerned by taking a simple swab culture of the wound [Church].
Laminar-airflow systems are a precaution taken against infection that is typically utilized in burn units [Church]. In laminar flow systems, air only flows in one direction (out of the room through a vent), which reduces the chance of contaminated air circulating to other areas of a floor or building.
Oral antibiotics are not widely used because they have been shown to be largely ineffective in preventing infection, and may actually promote infection by encouraging colonization by antibiotic-resistant strains [Church].
Alternative and Developing
Researchers are looking to develop alternative therapies to commercial antibiotics due to the emergence of resistant strains. The use of essential oils to combat infection has intrigued the pharmaceutical industry, possibly due to growing enthusiasm for organics and all-natural products in other sectors such as food and make-up. Edward-Jones and colleagues (2004) investigated the usefulness of lavender, geranium, patchouli, and tea tree oils, as well as grapefruit seed extract, in treating MRSA infections. Essential oils were tested singly and in various combinations in vitro. Solutions were placed on filter paper disks and were either placed directly on the agar plates or secured to the top of the Petri dish so that the vapors alone had contact with bacteria. Direct contact with tea tree oil was shown to be the most effective against MRSA out of the individual oils, while the combination of geranium oil and grapefruit seed extract was especially successful against MRSA as a vapor. While these results are auspicious, essential oils can be highly toxic and irritating, warranting caution as the leap is made from in vitro to in vivo studies.
Interest in the use of bacteriophages to treat antibiotic-resistant infections has experienced a renaissance in recent years. A 2007 study by McVay et al. examined the success of P. aeruginosa-specific phages in the prevention of sepsis and mortality in a mouse burn wound model. Subjects were thermally injured and then infected with a lethal dose of P. aeruginosa. Immediately following infection, mice received a phage cocktail intramuscularly, subcutaneously, or intraperitoneally. The mortality rate of the control group was 94%. In stark contrast, mortality was reduced to just 12% when the phage cocktail was administered intraperitoneally. Less, though still significant, success was seen in response to administration of the phages intramuscularly (72% mortality) and subcutaneously (78%).
As of March 2009, the development a phage cocktail against both S. aureus and P. aeruginosa had begun and is in the preliminary stages of clinical testing [Merabishvili]. It is intended that this cocktail be used as an alternative to or in conjunction with tradition antimicrobial therapies. Further experiments and testing will be required before phage therapies become widespread commercially, yet this remains an exciting and promising step forward in the treatment of burn patients.
Conclusion
Overall paper length should be 3,000 words, with at least 3 figures.
References
“Burn incidence and treatment in the U.S.: 2007 Fact sheet.” (2005). American Burn Association. http://www.ameriburn.org/resources_factsheet.php (Accessed 14 Apr 2009).
Church, D., Elsayed, S., Reid, O., Winston, B., Lindsay, R. (2006) Burn Wound Infections. Clinical Microbiology Reviews, 19 (2), 403–434.
McVay, C.S., Velasquez, M., Fralick, J.A. (2007). Phage therapy of Pseudomonas aeruginosa infection in a mouse burn wound model. Antimicrobial Agents and Chemotherapy 51 (6), 1934–1938.
Merabishvili, M., Pirnay, J., Verbeken, G., Chanishvili, N., Tediashivili, M., Lashkhi, N., Glonti, T., Kroylov, V., Mast, J., Van Parys, L., Lavigne, R., Volckaert, G., Mattheus, W., Verween, G., De Corte, P., Rose, T., Jennes, S., Zizi, M., De Vos, D., Vaneechoutte, M. (2009). Quality-Controlled Small-Scale Production of a Well-Defined Bacteriophage Cocktail for Use in Human Clinical Trials. PLoS ONE 4(3): e4944.
Murray, C., Hospenthal, D.R. (2008). "Burn Wound Infections" emedicine 16 Apr 2008. http://emedicine.medscape.com/article/213595-overview (Accessed 6 Apr 2009).
Vorvick, L. (2008). Medical encyclopedia: Skin layers. Medline Plus: a service of the U.S. National Library of Medicine and the National Institutes of Health. http://www.nlm.nih.gov/MEDLINEPLUS/ency/imagepages/8912.htm (Accessed 14 Apr 2009).
Edited by student of Joan Slonczewski for BIOL 238 Microbiology, 2009, Kenyon College.