Free Fatty Acids as antibacterial agents against several super pathogens including MRSA
Eliana McCann Smith
An Introduction to Super Pathogens
Over the past century, modern science has been overusing and misusing antibiotics, leading to the evolution of many “super pathogens”, or microbes that are resistant to most of the common antibiotics and other methods normally used to treat them. Bacteria and viruses that evade modern treatment through mutation and resistance are health dangers to hospital patients as well as to community members. Free fatty acids are a potential "natural" treatment that can be effective against certain microbes. For example, Staphylococcus aureus a bacterium that colonizes the human nose and skin is susceptible to certain kinds of free fatty acids. This is important because recently, overuse of antibiotics has led to the mutation of this pest bacteria to the super pathogen that is MRSA, Methicillin Resistant Staphylococcus aureus [Figure 1]. MRSA cannot be effectively treated by an entire class of common antibiotics called beta-lactams (which include penicillin and methicillin among others) [4]. Even the most potent “last line of defense” antibiotic, vancomycin, is ineffective on some strains of MRSA (VRSA, for vancomycin resistant Staphylococcus aureus)[5]. There are many of these pathogens - named super pathogens - that have developed resistance, including Clostridium difficile[6], several Enterococcus species including E. avium[7], along with many others.
These super pathogens demand alternate treatments from the scientific community, preferably treatments that pathogens cannot mutate around by developing resistance. Another solution might be to find treatments that could be used instead of antibiotics for non-threatening pathogens, and therefore prevent mutation/resistance in all bacteria. This would reduce the need for more potent antibiotics because super-pathogens would not evolve as quickly. A promising lead is, surprisingly, something that is already in high abundance on our own skin: fatty acids. The fatty acids found in abundance in human sebum are essential for defense against pathogens, and in healthy individuals are a sufficient barrier to gram positive harmful bacteria [8]. Commercially, fatty acids are used to treat acne (which is also caused by bacteria) and to prevent aging. Other fatty acids that do not naturally occur on our skin are in many of the foods we eat, such as coconuts [9]. Surprisingly, the potential benefits to using fatty acids as antimicrobials have been hinted at and studied for decades, but they have not achieved wide usage in the medical field.
About Free Fatty Acids
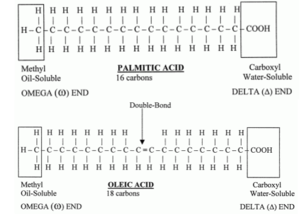
Fatty acids are a group of amphipathic biologically available compounds comprised of a carboxylic acid and a hydrophobic tail of varying carbon chain lengths [Figure 2]. If there are any double bonds in the carbon chain, the molecule is an unsaturated fatty acid, and the number of double bonds in the carbon chain determines how unsaturated it is. If there are no double bonds, then the fatty acid is considered saturated. The “free” part of the term free fatty acid, just means that it is not attached to any other compound in the cell. Fatty acids are found in many biological systems, including the human system. They are considered macronutrients, along with proteins and carbohydrates, and they yield the most ATP per gram out of all three. When fatty acids are used for energy storage in the body, they are stored as triglycerides, which are molecules containing three fatty acids attached to a glycerol molecule. When we eat fats, we normally are ingesting triglycerides. [10]
Another very important aspect of fatty acids in the body is cell membrane phospholipids, which are composed of two fatty acids attached by a phosphate group. The cell membrane is one of the primary characteristics of life. Some fatty acids even act as important signaling molecules, different from others because they can passively diffuse through hydrophobic membranes.[11] There are so many diverse uses for fatty acids in the human body, but what tends to get overlooked, is their role in epidermal defense. Yes, there are tons of fatty acids, some that we produce ourselves, and some that we need to ingest, that we come into contact with every day. They are on our skin, protecting us from external factors like microbes, but only the ones in their carboxylic acid forms.[12]
Fatty acids that are present in the epidermis, specifically in the stratum corneum, the outermost layer of the skin, consist primarily of palmitic acid, stearic acid, palmitoleic acid, oleic acid, linoleic acid (an essential fatty acid), and (cis)-11,14,17-eicosatrienoic acid (ETA).[13] However, epidermal fatty acid types and amounts vary among individuals, and do not change according to environmental factors, indicating that the type and amount produced is controlled by genetics.[14] Humans do not synthesize linoleic or linolenic acid, and therefore must be consumed in the diet. Since fatty acids play an important role in the protection of the body, these differences may be a reason why some people are more susceptible to skin disease or infection.
History of Fatty Acids as Antimicrobial Agents
Scientists have known about acids as anti-fungal products since 1899, when the “Toxic Effect of Deleterious Agents” was seen on fungi development.[15] Slightly later, in 1948, a review of “surface active agents” noted that quaternary ammonium salts increased their bactericidal activity with longer chain lengths.[16] Anionic compounds (fatty acids fit into this category) were shown to have activity only against gram-positive organisms. The toxicity of these quaternary agents affixed with groups such as chlorine, mercury, permanganate, alcohol, or formadehyde, with the least toxic being ammonium. We know now that these groups generally toxic to animal tissues, and more recent research has been looking at these fatty acids that are found in large quantities in other living systems (including our own).
Hydrolyzed fatty acids seem to have a higher antimicrobial effect than un-hydrolyzed fatty acids. An example of this is seen with virgin coconut oil, where the hydrolyzed coconut oil had antibacterial activity, but the unhydrolyzed oil did not. With increased addition of NaOH, antimicrobial activity increased, suggesting that the formation of the hydrolyzed coconut oil was what was antimicrobial.[17]
Some viruses are also susceptible to select free fatty acids [24] Medium and long-chained unsaturated free fatty acids inactivate enveloped viruses, but not non-enveloped viruses, suggesting that the mechanism of action of fatty acids is through disrupting the viral membrane. Confirming this hypothesis, in 1987 researchers found that when they incubated Vesicular stomatitis virus (VSV) with linoleic acid, an acid commonly found in human milk, they observed leakage out of the viral envelopes. Mother’s milk functions as an antiviral for the infant, which explains the difference in infection rate between breast-fed infants and formula fed infants. [24]
A different way fatty acids are being used, is to combat severe viral infections by way of fatty acid antiviral conjugates that produce fewer side effects in the host. [25] Antiviral medications are known to have a lot of side effects, especially in HIV patients. Fatty acid antiviral conjugates have a higher specificity for which cell type they effect, meaning that they show promise in selectively entering T helper lymphocytes, the cells that are attacked by the HIV virus that are very important in immune function. A fatty acid antiviral conjugate is covalently bound to an antiviral agent and a fatty acid that is usually an omega-3 fatty acid (DHA or EPA), or a fatty acid that is metabolized into an omega-3 fatty acid. The conjugation allows for the conjugated compound to be stable in the plasma, but once inside the cell, undergo hydrolysis to yield the two components, the antiviral agent and the omega-3 fatty acid. The omega-3 fatty acids are important because they exhibit anti-inflammatory properties, which aid in certain applications of viral treatment where inflammation could harm the effectiveness of the antiviral component.[24] These fatty acid components can target different cell types (i.e. lymph node, or liver) therefore increasing selectivity of antiviral therapy.
In 1972 a research group from Michigan Sate University published extensive data on the effects of several fatty acids on both gram-positive and gram-negative bacteria.[18] They demonstrated that by increasing the unsaturation of the fatty acids through the addition of cis double bonds, they could make these fatty acids more effective against gram-positive bacteria, but when the carboxylic acid was esterified the compounds lost their antibacterial effect. Strangely, they found that lauric acid, a saturated fatty acid, had the highest bacteriostatic potential towards these gram-positive bacteria of which included Staphylococcus genus, (which includes MRSA). Lauric acid was found to have the highest antimicrobial activity out a pool of saturated fatty acids, but overall, saturated fatty acids had lower activity than those that were unsaturated.[19] Palmitoleic acid, a monoene of human skin, was found to be most active against gram-positive bacteria, although in combination with ethanol, a synergistic effect against gram-negative bacteria (P. aeruginosa, P. acnes, E. coli) was seen.
Staphylococci epidermidis are found in abundance on healthy skin, whereas S. aureus are usually only found on damaged skin, but the reasons for this are unknown. A study in 1985 showed that staphylococci that were coagulase-positive, i.e. S. aureus, on the skin were sensitive to linolenic acid,[20] while other fatty acids were determined to have the same activity against coagulase-positive versus coagulase-negative staphylococci suggesting interference with the enzyme coagulase as a possible mechanism of action. This finding supports the premise that treatment with linolenic acid may be species specific, which is important because preserving Staphylococcus not of the species S. aureus is beneficial to the human system. The researchers even mutated the S. aureus, changing the characteristics of the bacteria in an attempt to mimic rapid evolution associated with resistance, to find a resistant strain towards linoleic acid. They were unsuccessful, suggesting linolenic acid will not cause resistance in bacteria, like other forms of treatment such as antibiotics. They also found that if human skin was covered in linolenic acid prior to the seeding of S. aureus, the bacteria were rapidly killed. However, the same group also found that antibacterial effects of this acid were reversed in vitro when low concentrations of human serum were present. They suggest a potential “detergent” mechanism, possibly the change in the functional group of the acid. This suggests potential problems with internal treatment of bacterial infections with linolenic acid. Another group got similar results with a different fatty acid, lauric acid, where interactions with human blood plasma decreased its antimicrobial activity.[21]
Bactericidal Effects of Fatty Acids on Methicillin Resistant and Susceptible Staphylococcus aureus
The mechanism of mutation from methicillin sensitive Staphylococcus aureus to methicillin resistant S. aureus (MRSA) is through the acquisition of the gene mecA, which after integration into the chromosome, codes for the penicillin-binding protein 2a, PBP2a. This protein can continue to crosslink peptidoglycan, the component of the cell wall, because it does not bind to methicillin or other beta-lactam antibiotics, making them all useless in treatment of MRSA.[26] It is important to study many strains of S. aureus, both resistant and not-resistant to typical antibiotic treatments, to be sure that the treatment in question will behave appropriately towards strains with different genetic variation. Of course, it is most important to find treatments against MRSA, as this has the highest current medical demand for a treatment. But eventually, finding compounds (or a combination of compounds) that prevent mutation in all variations of the species would be beneficial to everyone around the globe, and a way to practice preventative medicine, rather than reactive medicine.
Free fatty acids on human skin have been shown to have antibacterial properties against both methicillin susceptible (MSSA) and resistant (MRSA) Staphylococcus aureus. However, in order for the colonization of the bacteria to occur in the first place, the external mechanisms of protection must be nonfunctioning (i.e. the fatty acids living on the skin normally are not working effectively in protection). This could be because of a pre-existing skin disorder such as eczema (which will be addressed later on in this section), or because of mutations in the bacteria that allow it to survive regardless of the presence of the fatty acids. S. aureus possess surface proteins that interact with human serum proteins and human extracellular matrix proteins. A surface protein IsdA that is covalently attached to the bacterium, is needed in order to colonize the human nose. This is only expressed, however, under iron starvation, which is how the bacteria know they are in contact with their host: the skin is a biologically available iron poor environment.[27]. The presence of this protein makes S. aureus more hydrophilic and negatively charged, complicating the interaction between itself and the hydrophobic fatty acids.
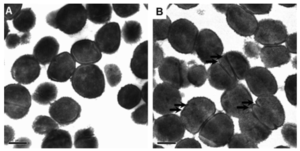
The most effective fatty acid against S. aureus colonization was found to be cis-6-Hexadecanoic acid (commonly known as sapienic acid).[28] This fatty acid was linked to S. aureus when it was found that people with atopic dermatitis (eczema) had higher levels of S. aureus on their skin, corresponding with lower levels of sapienic acid. [29]. MRSA is a big enough problem for people without skin disorders, but for individuals with atopic dermatitis, recurrent infections often lead to eczema exacerbation. There is currently no standard treatment for prevention of recurrent infections in either this patient group or the total patient group with MRSA. [30]. People with atopic dermatitis are also more likely to be colonized by S. aureus, prompting a closer look at their skin composition compared to those without a skin disorder. A difference in concentration of sapienic acid, a fatty acid usually found in high abundance on human skin in healthy patients, was found between groups. Patients with atopic dermatitis had lower amounts of acid on their skin, which correlated with higher colonization of S. aureus. Most interesting is that this is a reversible problem. When patients with atopic dermatitis were topically
treated with sapienic acid, colonization of S. aureus decreased, excitingly suggesting that sapienic acid is a pivotal factor in the skin’s innate immune system against S. aureus specifically.
The mechanism of sapienic acid on MSSA, was determined to be a multi component mechanism. Sapienic acid leads to the inability of S. aureus to control its internal pH because of a loss of membrane potential. This happens because at low pH, the carboxylic acid is deprotonated and can release a proton into the cytoplasm, increasing the pH. This explains the inhibitory effects of salts on fatty acids. The salts may bind to the fatty acid, rendering it useless, or they may stabilize the membrane of the bacteria. Another proposed mechanism of action is that since the acid increases the membrane fluidity, it may also disrupt membrane processes that lead to the cell division problems seen in Figure 3. A third possible mechanism of action is that the fatty acids disrupt the production of mitochondrial reactive oxygen species by interfering with electron transport.
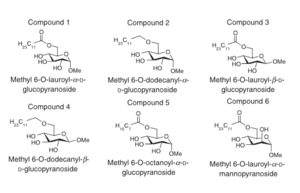
Novel carbohydrate fatty acid derivatives have been recently shown to have antimicrobial effects on several strains of S. aureus and MRSA.[31] The configuration of the hydroxyl group on the carbohydrate (not the fatty acid) part of the molecule determined the activity of the compound [Figure 4]. The mechanism of action of these compounds has to do with the cytoplasmic membrane, as well as other possible sites in the bacterium.
Conclusion
Super pathogens such as methicillin-resistant Staphylococcus aureus are evolving through mutations that overcome our treatment methods faster than we can create new ones. Natural products offer a huge repository of compounds that have potential value as treatments. The amazing aspect of this is that humans ourselves harbor known and unknown compounds that are innate to our immune function, and that the majority of the time protect us from pathogens overwhelmingly well. The fatty acids on our skin, including sapienic acid and palmitoleic acid, are pivotal players in our bodies’ external defenses. Other fatty acids and their derivatives that are not naturally occurring on human skin, but can be obtained relatively easily from essential oils (such as linolenic acid and lauric acid from coconut oil) and are included in these potential wonder drugs. While it is clear that there are still many questions about the mechanisms of these fatty acids against pathogens, it seems to be a ripening field of study that is worth studying for future treatments. Perhaps sometime in the near future, we will be able to use supplements of our own bodies’ protective mechanisms in bulk to ward off pathogens more efficiently without putting harmful drugs (antibiotics) into our systems or the systems of the pathogens, which would then slow the mutation rate and therefore diminish the speed of the super pathogens’ evolution.
References
[1] http://www.ncbi.nlm.nih.gov/pubmedhealth/PMHT0025827/?figure=1
[5] http://www.niaid.nih.gov/topics/antimicrobialResistance/Examples/mrsa/
[6] Gould, IM. 2010. VRSA-doomsday superbug or damp squib? Lancet Infect Dis 10 (12): 816–8. doi:10.1016/S1473-3099(10)70259-0. PMID 21109164.
[7] http://www.cdc.gov/drugresistance/threat-report-2013/index.html
[8] http://www.antimicrobe.org/new/b03.asp
[9] Clarke, S. R., R. Mohamed, L. Bian, A. F. Routh, J. Kokai-Kun, J. J. Mond, A. Tarkowski, and S. J. Foster. 2007. The Staphylococcus aureus surface protein IsdA mediates resistance to innate defenses of human skin. Cell Host Microbe 1:199-212
[10] Verallo‐Rowell, V.M., Dillague, K.; Syah‐Tjundawan, B.S. 2008. Novel Antibacterial and Emollient Effects of Coconut and Virgin Olive Oils in Adult Atopic Dermatitis. Journal of Dermatitis. 19 (6):301-358
[11] https://en.wikipedia.org/wiki/Fatty_acid
[12] http://www.nature.com/scitable/topicpage/fatty-acid-molecules-a-role-in-cell-14231940
[13] Butcher GW, King G, Dyke KG. 1976. Sensitivity of Staphylococcus aureus to unsaturated fatty acids. J. Gen. Microbiol. 94:290 –296. http://dx .doi.org/10.1099/00221287-94-2-290.
[14] Kim, E. J., Kim, M.-K., Jin, X.-J., Oh, J.-H., Kim, J. E., & Chung, J. H. (2010). Skin Aging and Photoaging Alter Fatty Acids Composition, Including 11,14,17-eicosatrienoic Acid, in the Epidermis of Human Skin. Journal of Korean Medical Science, 25(6), 980–983. http://doi.org/10.3346/jkms.2010.25.6.980
[15] Green, S.C.S, M.E., Downing, D.T. (1984). Variation in Sebum Fatty Acid Composition Among Adult Humans. 1984 J Investig Dermatol. 83 (2): 114-117 http://dx.doi.org/10.1111/1523-1747.ep12263287
[16] Clark, J. R. 1899. On the toxic effect of deleterious agents on the germination and development cf certain filamentous fungi. Botan. Gaz. 28:289-327.
[17] Glassman, H. N. 1948. Surface active agents and their application in bacteriology. Bacteriol.Rev. 12:105-148
[18] http://innovareacademics.in/journals/index.php/ajpcr/article/view/1042
[19] Kabara, J. J., Swieczkowski, D. M., Conley, A. J., & Truant, J. P. (1972). Fatty Acids and Derivatives as Antimicrobial Agents. Antimicrobial Agents and Chemotherapy, 2(1), 23–28.
[20] Wille J, J, Kydonieus A, Palmitoleic Acid Isomer (C16:1Δ6) in Human Skin Sebum Is Effective against Gram-Positive Bacteria. Skin Pharmacol Physiol 2003;16:176-187
[21] Lacey, R., Lord V.J. Med. Microbiol. 14(1):41-49 doi:10.1099/00222615-14-1-41
[22] Kitahara T, Koyama N, Matsuda J et al. (2004) Antimicrobial activity of saturated fatty acids and fatty amines against methicillin-resistant Staphylococcus aureus. Biol Pharm Bull 27:1321–1326
[23] http://www.benbest.com/health/essfat.html
[24] Thormar, H., Isaacs, C. E., Brown, H. R., Barshatzky, M. R., & Pessolano, T. (1987). Inactivation of enveloped viruses and killing of cells by fatty acids and monoglycerides. Antimicrobial agents and chemotherapy, 31(1): 27-31
[25] http://patents.justia.com/inventor/amal-ting
[26] Lowy FD (May 2003). "Antimicrobial resistance: the example of Staphylococcus aureus". J. Clin. Invest. 111 (9): 1265–73. doi:10.1172/JCI18535
[27] http://europepmc.org/abstract/MED/18005699
[28] http://aac.asm.org/content/58/7/3599.full
[29] http://www.karger.com/Article/Abstract/87018
[30] http://www.sciencedirect.com/science/article/pii/S2213219814001718
[31] http://onlinelibrary.wiley.com/doi/10.1111/j.1365-2672.2009.04622.x/epdf
Authored for BIOL 291.00 Health Service and Biomedical Analysis, by Eliana McCann Smith, taught by Joan Slonczewski, 2016, Kenyon College.
